Ultrasound Guided Standalone Percutaneous Needle Tenotomy for Chronic Lateral Epicondylitis: A Systematic Review
Abstract
Objective
Identify if ultrasound guided stand-alone percutaneous needle tenotomy (PNT) is an effective treatment for chronic lateral epicondylitis and extract data for a protocol on how to administer the PNT.
Design
Systematic review of the available literature.
Methods
The research was done in March 2017 and it was restricted to articles published in the last fifteen years. Databases searched included PubMed and Google Scholar.
Results
5 articles met our requirements: 3 articles and 2 reviews, one about lateral elbow tendon needling treatment and one about every region of the body tendons treatment. No new interesting articles were found in a further scan of the review. None of the articles found had the quality level that we expected: Only one was a prospective randomized controlled study; The two remaining articles were prospective cohort studies. They have limitations in their design and in their execution, mainly due to the low number of patients recruited in the studies and the overall lack of a control placebo group.
Conclusions
Although all of the studies show good results in terms of pain improvement, and low rates of complications, the literature about the standalone dry needling procedure for the treatment of the lateral epicondylitis is scarce with a limited quality level of the studies.
Keywords
Epicondylitis needling, Epicondylitis fenestration, Epicondylitis tenotomy, Elbow needling, Elbow tenotomy, Elbow fenestration, Tendinopathy tenotomy, Tendinopathy fenestration, Tendinopathy needling, Tendon tenotomy, Tendon fenestration, Tendon needling
Introduction
Lateral epicondylitis is the most frequent cause of pain in the elbow. It is 7-10 times more frequent than medial epicondylitis [1], and one of the most common musculoskeletal disorders, affecting 1-3% of the adults each year [2,3]. It is most prevalent in the working age population and usually affects the dominant arm [4].
Lateral epicondylitis was first thought to be caused by a condition first described in 1873 [5]. It has also been called tennis elbow ("tennis elbow"), although it is not exclusively due to playing tennis but is actually more commonly observed in people who perform heavy manual jobs. It was assumed to be due to an inflammatory process of the common extensor tendon origin and lateral epicondyle periosteum. Therefore, anti-inflammatory agents (mainly corticosteroids) have often been used [1]. Pathophysiology is still not clear, although many theories have been suggested (e.g. bursitis, periostitis, infection, aseptic necrosis, neuritis of branches of the radial nerve, radiohumeral synovitis, and irritation of the collateral ligament etc.) [5]. According to the most widely accepted theory, there is a degenerative process due to recurrent mechanical overuse or overloading at the lateral elbow, with an abnormal auto-repairing process of the tendon with consequent scar formation and malalignment of collagen fibers in the extensor carpi radialis brevis [6]. This is supported by histological analysis, which has shown immature fibroblastic and vascular infiltration of the origin of the extensor carpi radialis [1].
For these reasons, the terms "tendinopathy" or "tendinosis" or "epicondylosis" are now preferred over "epicondylitis" or "tennis elbow".
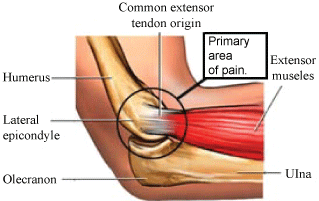
Clinically, the patients usually experience local tenderness over the lateral epicondyle, pain in the extensor muscles while holding something, and resistance to extension movements of the wrist. On examination, pain may be exacerbated by resisted wrist extension in the pronated position, which is worse with the elbow at full extension (Figure 1) [5].
Treatment procedures for chronic lateral epicondylitis can be divided into conservative, minimal invasive and operative.
The conservative treatment is often long-term physiotherapy, ranging from ten to eighteen months. It is successful in 90% of cases [7,8]. Also a wait-and-see approach can be considered. Some studies have shown that avoidance of aggravating activities lead to a spontaneous improvement in mid- to long-term follow-up, with results comparable with physiotherapy (i.e. success rates at 52 weeks 69% with corticosteroid injections, 91% with physiotherapy, 83% with a wait-and-see policy) [9,10].
For the non-responding 10% of cases, there is no consensus on a standard treatment. Therefore, based on the above mentioned pathophysiological theories, multiple therapeutic procedures have been tried and described. Examples of these procedures include Nonsteroidal Anti-Inflammatory Drugs (NSAIDs) [11], corticosteroid injections [12], extracorporeal shock wave therapy [13], orthotics [14], laser therapy [15], botulinum toxin injections [16], platelet-rich plasma injections [17], autologous blood injections [17] and topical nitrates [18].
The operative approach includes multiple open, percutaneous and arthroscopic techniques, all sharing the same goal of excising abnormal tissue within the origin of the extensor carpi radialis brevis tendon at the lateral epicondyle or a total release of the tendon [5]. These procedures have been effective in 75% to 90% of patients, but expose patients to operative risks; Moreover, recovery is often prolonged [3,5]. Therefore, surgery is recommended only when conservative strategies fail.
Compared to surgery, Percutaneous Needle Tenotomy (PNT) is a less invasive alternative.
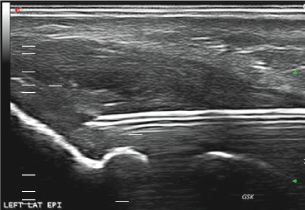
Also called "dry needling" or "percutaneous tendon fenestration", PNT has been used by orthopaedics for decades to treat tendinosis, and it is used by radiologist from less than 20 years. It was initially performed without imaging guidance, using palpation to locate the tendon. Anyway, ultrasound guidance can potentially improve the efficacy of percutaneous procedures, because it ensures an accurate placement of the needle into the abnormal tendon and prevents damage to other structures (e.g. lateral ligament complex, reducing the complications [19]), (Figure 2).
This technique is minimally invasive, safe, without significant complications, with low cost and low risk. Compared to an open procedure, it provides significantly better results, is faster and can be performed under local anesthesia [20].
Currently, the dry needling procedure is often performed together with injection of active substances (e.g. blood growth factors, platelet-rich plasma, corticosteroids). Even though the effectiveness of these extra injections has been debated [21], literature on the effectiveness of PNT without fluid injection is scarce.
Our aim is to study the effectiveness of ultrasound guided standalone Percutaneous Needle Tenotomy (PNT) in the treatment of the lateral epicondylitis, and to extract data for a protocol on how to administer the PNT, by performing a systematic review of the literature on PNT for lateral epicondylitis.
Materials and Methods
Literature search
We conducted a systematic review of the literature. Databases searches included PubMed and Google Scholar. The research was performed in March 2017 and it was restricted to articles published in the last fifteen years.
In the first step, keywords related to lateral epicondylitis percutaneous tenotomy treatment were included: "epicondylitis needling", "epicondylitis fenestration", "epicondylitis tenotomy", "elbow needling", "elbow tenotomy", "elbow fenestration".
In the second step, the search included non-specific terms like "tendinopathy tenotomy", "tendinopathy fenestration", "tendinopathy needling", "tendon tenotomy", "tendon fenestration", "tendon needling", in order to identify general treatments of tendinopathy in every region of the body, to find some lateral epicondylitis tenotomy treatment not mentioned in the titles, and to have a wider view of the technique effects in the other tendons.
Furthermore, also the references of identified studies were checked for studies that may have been missed in the initial search.
Exclusion criteria
Congress proceedings, posters, abstracts and case reports were excluded. We did not accept studies written in a language different from English.
Study selection
The initial search was performed by a single reviewer. All remaining stages were performed by two reviewers.
The identified records were subsequently analysed for a further selection, screening their titles and abstracts, and finally the full texts of identified publications potentially relevant to the present study.
Further selection criteria were then applied to the remaining studies: Articles had to be of level 1b or 2b evidence (respectively, prospective randomized controlled studies and retrospective cohort studies); Also previous systematic reviews of 1a and 2a level were accepted [22,23]; Furthermore, the PNT procedure had to be performed with ultrasound guidance, without injection of fluid during or after the initial needling (corticosteroids or platelet-rich plasma, blood growth factors), and without other applied procedures (e.g. with Tenex, which is a minimal invasive procedure that combines ultrasound imaging with a ultrasonic energy device that destroys scar and damages the tissue at the tendon insertion [24].
Reported outcome
From the relevant articles we summarized the way patients were selected, the outcomes, the adverse events, the conclusions. Moreover, we extracted and summarized the way the PNT had been performed in every study.
Results
Included studies
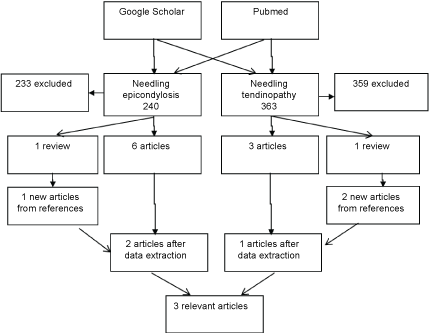
In the initial search, 603 studies were found (Figure 3). Of these, 240 studies were on needling treatment for lateral epicondylitis of the elbow and 363 studies were on needling treatment for tendinopathy of different regions. After screening of titles and abstracts, 592 studies were excluded due to irrelevant topic and based on the type of study.
With the criteria described previously (no ultrasound guidance, no other fluid injection or procedures), 5 studies met our requirements: 3 articles (Table 1) and 2 reviews (one about lateral elbow tendon needling treatment 2 and one about the treatment of tendons in every region of the body [25]). The reviews were further scanned for relevant articles, but no new articles were found.
Effectiveness of PNT
McShane, et al. [26] conducted a prospective study on 52 patients with recalcitrant lateral epicondyle pain. The aim of the study was to evaluate the effectiveness of needling alone in the treatment of chronic lateral epicondylitis. The mean age of the patients was 49 years. The patients' natural histories had been established by the fact that they had persistent, unresolved pain. They had had at least 3 of 5 failed nonsurgical treatments (corticosteroid injections, NSAIDs, bracing, physiotherapy and wrist splinting) and a confirmed ultrasonographic diagnosis of common extensor tendinopathy. The patients were interviewed at an average follow-up time of 22 months.
The method used to measure the therapeutic efficacy of the treatment was asking the patient directly to graduate the pain with the words "excellent" (if "very happy with the procedure and had no room for improvement"), "good" (if "happy with the outcome but had some room for improvement"), "fair" (if "slight dissatisfaction with the outcome of the procedure and had room for significant improvement") or "poor" (if "dissatisfied with the outcome of the procedure and had little or no improvement"). With the same graduation, they asked to the patient to categorize their ability to perform various tasks and a perception of overall procedure-related improvement. Outcomes scores about the perception of overall procedure-related improvement were: 57.7% excellent, 34.6% good, 1.9% fair, 5.8% poor. No adverse events were reported. The authors concluded that percutaneous tenotomy is a safe and effective treatment for chronic lateral epicondylitis.
Stenhouse, et al. [27] conducted a prospective, randomized controlled study comparing the outcomes in 28 patients with refractory lateral epicondylitis, 13 of which treated with percutaneous tenotomy and 15 treated with the same procedure with associated autologous conditioned plasma (ACP) injection. The aim of this study was to evaluate the benefit associated to the addition of ACP to needling. The mean age of the patients was 49 years and they all had symptoms for more than 6 months. In all patients, a common extensor tendinopathy was seen on ultrasound examinations, and physical therapy and steroid injections failed.
Both procedures, with needling followed by ACP and with needling alone, were performed twice, with the second repeated one month after the first.
The method used to measure the therapeutic efficacy of the treatment was the VAS score (a scale from 0 to 10 where 0 is no pain, 1-3 mild pain, 4-6 moderate pain and 7-10 severe pain) [28]. VAS was measured before the treatment and 2 and 6 months after the treatment. The outcome score pre-treatment in the first group was 8.07, while in the randomized group with dry needling alone procedure was 6.87; After 6 months the VAS was 4.15 and 4.50, respectively. Therefore, both groups demonstrated a decrease in the intensity of pain (VAS) from baseline at 6 months, with no significant difference between groups at those time points though.
Furthermore, Stenhouse, et al. used also the Nirschl scoring system, that includes different parameters like elbow pain, elbow function, patient satisfaction and elbow mobility, with maximum scoring of 80. Pre-treatment Nirschl scores were 22.9 in the dry needling group and 11.1 in the ACP group. After 6 months, the mean improvement compared to baseline was 22.5 points in the dry needling group and 40.0 points in the ACP group. Between-group differences were not significant.
No complications or adverse reactions were described.
The authors concluded that percutaneous tenotomy, with or without ACP injection, is an effective treatment for chronic lateral epicondylitis, with no substantial differences.
Housner, et al. [29] conducted a prospective cohort study on a total of 14 tendons in 13 patients with PNT stand-alone. The aim of this study was to evaluate the safety and short-term effectiveness of sonographically guided PNT in the treatment of tendinosis. The mean patient age was of 38.5 years and the average duration of symptoms was 53 months. The specific tendons treated were patellar (5), achilles (4), proximal gluteus medius (1), proximal iliotibial tract (1), proximal hamstring (1), common extensor elbow (1), and proximal rectus femoris (1).
Patients were included if the history and physical examination were consistent with a chronic tendon injury, followed by a sonographic examination identifying tendinosis. All patients had failed to respond to conservative treatment, including relative rest, pain medications, physical therapy and corticosteroid injections.
The pain of each patient was measured with a questionnaire using the VAS. The mean pain rating scores ± SEM (standard error of measurement) at the baseline and 4 and 12 weeks later were 5.8 ± 0.6, 2.4 ± 0.7, and 2.2 ± 0.7, respectively.
No complications were noted during the procedure, nor at the 4- and 12-week follow-up visits.
The results of this study of selected patients with chronic tendinopathy showed that sonographically guided tenotomy had no complications and resulted in a statistically significant reduction in mean pain scores after 4 weeks, maintained at the 12-week follow-up (Table 1).
How to diagnose lateral chronic epicondylitis and apply sonographically guided tenotomy?
In the three studies, a musculoskeletal radiologist performed an ultrasound examination to diagnose lateral chronic epicondylitis in all the patients that, based on clinical information, were considered eligible for the treatment.
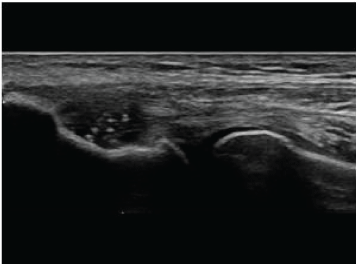
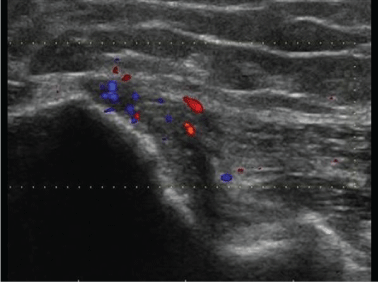
In the study by McShane, et al. all of the 52 sonographic reports described tendon thickening, heterogeneity and hypoechoic foci, and some of them intrasubstance tears or calcifications. In the study by Stenhouse, et al. all the patients treated had heterogeneity and neovascularization on power Doppler. In the study by Housner, et al. a single ultrasound sign of lateral chronic epicondylitis was deemed sufficient for the diagnosis: Pain in the lateral aspect of the elbow, at the common extensor tendon insertion, when pressure on the region was applied using the probe; Thickening of the common extensor tendon; Insertional calcifications; Tendon hyperaemia; Hypoechoic foci; Cortex irregularities in the lateral humeral epicondyle [30] (Figure 1 and Figure 4).
In all studies, the PNT was performed with the patient lying on a couch or sitting comfortably in a chair and the forearm resting passively by the side. The elbow was flexed to 90 degrees and the wrist passively flexed to around 60 degrees; The entire aspect of the lateral elbow was prepared with a disinfectant (Betadine or ethanol or other alcohol solution), and a sterile field was set up and maintained around the target area during all the procedure. A ranging 24-30 Gauge needle was used to inject a local anaesthetic (lidocaine, bupivacaine) around the entire common extensor origin and in the subcutaneous soft tissue under ultrasound guide. The amount of the anaesthetic was reported as "adequate" by McShane, et al. 1-2 ml by Stenhouse, et al. and ranging from 3 to 6 ml by Housner, et al. After the local anaesthetic had taken effect, a needle of different size (20 G in McShane, et al. 22 G in Housner, et al. 23 G in Stenhouse, et al.) was introduced through the skin. With continuous sonographic visualization, approximately 20-30 [26-29] or 40-50 [29] needle passes were made through the abnormal region of the tendon, or at least once in every abnormal part [27]. If present, calcifications within the substance of the tendon or enthesophytes at the tendon origin or both were mechanically fragmented [3,26,29] (Figure 5).
In the study by Stenhouse, the procedure was repeated after one month. After the procedure, all patients were given rest and postprocedural activity restrictions (patients were allowed to continue usual daily activities) for 4-6 weeks and scheduled for 2-6 weeks revaluation to decide how to proceed. In one study [17], NSAIDs were prescribed and, from the day after the procedure, physiotherapy was advised twice a week for 12 weeks.
Discussion
Main findings summary
The aim of our review was to collect articles published on PNT ultrasound guided in the treatment of chronic lateral epicondylitis, in order to understand the evidence and the limitations in the knowledge of this technique today and, in particular, if tendon needling can be beneficial as a stand-alone treatment for common extensor tendons tendinopathy. Only three articles meeting our selection criteria were found on this topic. Most of the studies were excluded because of the combined injection with a substance (e.g. corticosteroids, platelet-rich plasma or autologous blood) [31,32] or the lack of a ultrasonographical guide [33,34].
None of the articles found had the quality level that we expected (Table 2, Table 3 and Table 4). They have limitations in their design and in their execution, mainly due to the low number of patients recruited in the studies and the overall lack of a placebo control group.
The prospective study conducted by McShane, et al. in 2008 demonstrated that percutaneous tenotomy is a safe and effective treatment for chronic lateral epicondylitis, with at least 80% of patients achieving good to excellent results.
McShane, et al. had conducted a previous prospective cohort study in 2006 [31], where 55 patients were studied after treatment of lateral refractary epicondylitis with ultrasound guided PNT combined with corticosteroid injection (6 mg of betamethasone or 40 mg of triamcinolone acetonide), so it didn't met our criteria. The inclusion criteria of the patients were the same in both studies. The patients were interviewed at a mean follow-up time of 28 months. The perception of overall procedure-related improvement included these outcomes: 63.6% excellent, 16.4% good, 7.3 fair, 12.7% poor. No adverse events were reported. The authors concluded that PNT combined with corticosteroid injection is as safe and effective for chronic lateral epicondylitis as PNT alone. Although they consider the data not directly comparable, based on these two studies they decided not to use corticosteroids in the future. The limitation of the comparison is that it was not performed as a Retrospective Control Trial and a learning effect for performance of the procedure could not be excluded between the studies.
Despite this, the results are relatively comparable for the percutaneous tenotomy with and without corticosteroid injection, and it is suggested that there is not a significant difference between the two treatments, confirming the non-inflammatory etiology of the lateral epicondylitis chronic phase and the little added therapeutic value of corticosteroids.
The prospective randomized controlled study by Stenhouse, et al. demonstrated a VAS pain improvement from baseline to 6 months control in the two compared groups treated with PNT and with PNT combined with Autologous Conditioned Plasma (APC). All patients were selected with ultrasound examination, that had to show heterogeneity and neovascularity at the common extensor tendon origin, in order to exclude the patients with chronic elbow pain but no true tendinosis. Although the remaining patients represented an appropriated target for the two different treatments, these rigid criteria could actually be a limit of the study, because they had further reduced the number of patients to treat, not including some with tendinosis. Anyway, the small size of the sample (percutaneous tenotomy, n = 13; ACP, n = 15) is the main limitation of this study.
The two studied groups were homogeneous, with only some small difference, like the mean duration of the symptoms, that was 14.5 months in the dry needling group and 17.8 months in the ACP group, even if there was a big intragroup variability, with a range of symptoms duration of 2-64 months (including, therefore, some cases of acute epicondylitis).
Other limitations are that the study was conducted in a single center and that there was no a true placebo control group; The needling alone group was used as a control group because the author considered unethical to include a group with no effective treatment.
Despite these limitations, in both group the change of the VAS is comparable and this shows that needling is useful to reduce the pain in the lateral epicondylitis treatment, and that the effect of the ACP injection after the needling treatment is superfluous for the improvement of the clinical condition.
The randomized prospective study by Housner, et al. showed an improvement of the VAS score from the baseline to 4 weeks, that was maintained after 12 weeks.
Nevertheless, this study has multiple limitations. The population was a relatively inhomogeneous group of patients because the authors wanted to report the experience of multiple tendons treatment; In addition, previous clinical treatments were not standardized, there was no control placebo group and follow-up time was short, with the final control performed at 12 weeks.
The overall conclusion of this study is that ultrasound guided PNT without any other combined injection is an effective treatment to reduce pain in patients with chronic tendinopathy, also of the lateral epicondyle of the elbow. Anyway, because of the small number of the results with only one about elbow, it is not possible to have a real idea of the reliability of the study.
In our review, studies were excluded if the PNT was performed without ultrasound guidance, or when other treatments were performed during the PNT.
Although the injections of other substances can distort all the results, the same cannot be said about the studies with PNT performed without ultrasound guidance; In fact the results of these are similar to those performed with ultrasound guidance [34,35], as we could have expected due to the main problem of this treatment, that is the lack of certainty to act on the common extensor tendons. For this reason, the results found by these authors could be used to corroborate the results found in the procedures with US guide. It remains, however, the limitation related to the fact that a blinding procedure does not ensure a perfect execution of the treatment, and this would represent a limit for the patient and for a real comprehension of the outcomes. Furthermore, the use of sonographic guidance in the treatment of musculoskeletal injuries is constantly gaining exposure in the literature [36], because it offers dynamic and real-time tendon imaging, with essentially no harmful effects to the patient. From a procedural standpoint, sonography is helpful both to diagnose the precise location of tendon abnormalities [36] and to provide continual guidance regarding the needle location [36].
Thus, we thought it would be inappropriate to use the data resulting from an older technique as a theoretical support to a newer one designed to replace it.
We also found some studies about a PNT procedure performed under ultrasound guide with TNX1 [3,37], a recent minimally invasive technique that uses ultrasonic energy to produce oscillations of hollow-tip needle [38]. The rapid needle movement cuts through the tendon and emulsifies tendinotic tissues around the needle tip. The needle is inserted in the target region after a small incision on the skin (4 mm). The outcomes are very satisfactory when evaluated as VAS. Although the logic and the mechanism of this treatment is almost the same of PNT the two procedures are not comparable.
Diagnosis and Protocol
We did not find a complete conformity in the three studies on the criteria used to select patients to treat. The presence of chronic pain was not well defined in terms of time, and a large range in time was found within the studies. The poor response to nonsurgical therapies was uniformly cited in all the studies, although these previous treatments were different and often performed with different timing compared to the PNT.
For the ultrasound criteria of epicondylitis, the recruited patients had different patterns also within the studies, and different number of positive criteria (one was enough for Housner, et al.).
Thus, the protocols were applied to a relatively homogeneous sample of patients with epicondylitis in the study by Stenhouse, and in a non-uniform sample of patients in the studies by McShane and Housner.
Concerning the PNT protocol, this was performed similarly in the three studies, with some minor differences. After setting up a sterile field and injecting a variable amount of anaesthetic (lidocaine or bupivacaine), they passed the needle in the abnormal regions of the tendon 20-30 times in the studies by McShane and Housner, studies and 40-50 in Stenhouse with different needle (20, 22 and 23 G, respectively). Furthermore, some outcome distortions could be created by the different ways the PNT was performed): Stenhouse, et al. repeated the dry needling procedure after one month, while in the studies by McShane and Housner the procedure was done only one time. Stenhouse, et al. chose this strategy because this practice had been done elsewhere with autologous conditioned plasma and it had demonstrated that the pain relief is cumulative following each injection. The procedure was performed two times also in the group with needling alone treatment, with a clinical deterioration after the second injection. The reason of this phenomenon is unclear (interruption of the original healing cascade that had already started?), and other studies should be conducted comparing the results between a group with only one dry needling treatment and a group with two needling treatments. Anyway, in our study this could create a distortion, because we could not understand the influence of the second treatment on the outcomes).
In all the studies the post-treatment protocol was the same, including rest, slow return to daily activities and no corticosteroids.
Limitations
The main limitation is the lack of studies on the effectiveness of the dry needling procedure stand-alone in the treatment of the lateral epicondylitis compared to a placebo group. Only the study by had the aim to demonstrate whether dry needling was sufficient to treat the lateral epicondylitis or a combined injection of corticosteroids was useful. Housner, et al. studied the effectiveness of the PNT in the treatment of all the body tendons, therefore they did not focus on the common extensor tendons. Stenhouse was interested in the ACP effectiveness in the chronic lateral epicondylitis treatment, and used a control group with only dry needling treatment, that we can use for our study.
Conclusion
We conclude that the literature about the dry needling procedure stand-alone for the treatment of the lateral epicondylitis is scarce. The studies have a limited quality level. Despite this, all the studies show good results in terms of pain improvement, and low rates of complications. Furthermore, the treatment time is short, the anaesthesia doses are small, it does not require an operating room, with no hospital recovery, with a return-to-work time of 1 day and, therefore, shows an economical advantage compared to surgical treatment.
References
- Hoogvliet P, Randsdorp MS, Dingemanse R, et al. (2013) Does effectiveness of exercise therapy and mobilisation techniques offer guidance for the treatment of lateral and medial epicondylitis? A systematic review. Br J Sports Med 47: 1112-1119.
- Mattie R, Wong J, McCormick Z, et al. (2017) Percutaneous needle tenotomy for the treatment of lateral epicondylitis: A systematic review of the literature. PMR 9: 603-611.
- Barnes DE, Beckley JM, Smith J (2015) Percutaneous ultrasonic tenotomy for chronic elbow tendinosis: A prespective study. J Shoulder Elbow Surg 24: 67-73.
- Dimitrios S (2016) Lateral elbow tendinopathy: Evidence of physiotherapy management. World J Orthop 7: 463-466.
- Panthi S, Khatri K, Kharel K, et al. (2017) Outcome of percutaneous release of tennis elbow: A non-randomized controlled trial study. Cureus 9: e952.
- Bhabra G, Wang A, Ebert JR, et al. (2016) Lateral elbow tendinopathy: Development of a pathophysiology-based treatment algorithm. Orthop J Sports Med 4.
- Coombes B, Bisset L, Vicenzino B (2015) Management of lateral elbow tendinopathy: One size does not fit all. J Orthop Sport Phys Ther 45: 938-949.
- Bisset LM, Vicenzino B (2015) Physiotherapy management of lateral epicondylalgia. J Physiother 61: 174-181.
- Johnson GW, Cadwallader K, Scheffel SB, et al. (2007) Treatment of lateral epicondylitis. Am Fam Physician 76: 843-848.
- Smidt N, van der Windt DA, Assendelft WJ, et al. (2002) Corticosteroid injections, physiotherapy, or a wait-and-see policy for lateral epicondylitis: A randomised controlled trial. Lancet 359: 657-662.
- Wolf JM, Ozer K, Scott F, et al. (2011) Comparison of autologous blood, corticosteroid, and saline injection in the treatment of lateral epicondylitis: A prospective, randomized, controlled multicenter study. J Hand Surg Am 36: 1269-1272.
- Gulabi D, Uysal MA, Akça A, et al. (2017) USG-guided injection of corticosteroid for lateral epicondylitis does not improve clinical outcomes: A prospective randomised study. Arch Orthop Trauma Surg 137: 601-606.
- Buchbinder R, Green SE, Youd JM, et al. (2006) Systematic review of the efficacy and safety of shock wave therapy for lateral elbow pain. J Rheumatol 33: 1351-1363.
- Bisset LM, Collins NJ, Offord SS (2014) Immediate effects of 2 types of braces on pain and grip strength in people with lateral epicondylalgia: A randomized controlled trial. J Orthop Sports Phys Ther 44: 120-128.
- Bjordal JM, Lopes-Martins RA, Joensen J, et al. (2008) A systematic review with procedural assessments and meta-analysis of low level laser therapy in lateral elbow tendinopathy (tennis elbow). BMC Musculoskelet Disord 9: 75.
- Galvin R, Callaghan C, Chan WS, et al. (2011) Injection of botulinum toxin for treatment of chronic lateral epicondylitis: Systematic review and meta-analysis. Semin Arthritis Rheum 40: 585-587.
- Krogh TP, Bartels EM, Ellingsen T, et al. (2013) Comparative effectiveness of injection therapies in lateral epicondylitis: A systematic review and network meta-analysis of randomized controlled trials. Am J Sports Med 41: 1435-1446.
- Paoloni JA, Appleyard RC, Nelson J, et al. (2003) Topical nitric oxide application in the treatment of chronic extensor tendinosis at the elbow: A randomized, double-blinded, placebo-controlled clinical trial. Am J Sports Med 31: 915-920.
- Chiavaras MM, Jacobson JA (2013) Ultrasound-guided tendon fenestration. Semin Musculoskelet Radiol 17: 85-90.
- Dunkow PD, Jatti M, Muddu BN (2004) A comparison of open and percutaneous techniques in the surgical treatment of tennis elbow. J Bone Joint Surg Br 86: 701-704.
- Gosens T, Peerbooms JC, van Laar W, et al. (2011) Ongoing positive effect of platelet-rich plasma versus corticosteroid injection in lateral epicondylitis: A double-blind randomized controlled trial with 2-year follow-up. Am J Sports Med 39: 1200-1208.
- http://www.cebm.net/oxford-centre-evidence-based-medicine-levels-evidence-march-2009/
- https://en.wikipedia.org/wiki/Levels_of_evidence
- Darryl E Barnes (2013) Ultrasonic energy in tendon treatment. Oper Tech Orthop 23: 78-83.
- Krey D, Borchers J, McCamey K (2015) Tendon needling for treatment of tendinopathy: A systematic review. Phys Sportsmed 43: 80-86.
- McShane JM, Shah VN, Nazarian LN (2008) Sonographically guided percutaneous needle tenotomy for treatment of common extensor tendinosis in the elbow: Is a corticosteroid necessary? J Ultrasound Med 27: 1137-1144.
- Stenhouse G, Sookur P, Watson M (2013) Do blood growth factors offer additional benefit in refractory lateral epicondylitis? A prospective, randomized pilot trial of dry needling as a standalone procedure versus dry needling and autologous conditioned plasma. Skeletal Radiol 42: 1515-1520.
- Miller MD, Ferris DG (1993) Measurement of subjective phenomena in primary care research: The visual analogue scale. Fam Pract Res J 13: 15-24.
- Housner JA, Jacobson JA, Misko R (2009) Sonographically guided percutaneous needle tenotomy for the treatment of chronic tendinosis. J Ultrasound Med 28: 1187-1192.
- Obradov M, Anderson PG (2012) Ultrasonographic findings for chronic lateral epicondylitis. JBR-BTR 95: 66-70.
- McShane JM, Nazarian LN, Harwood MI (2006) Sonographically guided percutaneous needle tenotomy for treatment of common extensor tendinosis in the elbow. J Ultrasound Med 25: 1281-1289.
- Zhu J, Hu B, Xing C, et al. (2008) Ultrasound-guided, minimally invasive, percutaneous needle puncture treatment for tennis elbow. Adv Ther 25: 1031-1036.
- Lakhey S, Mansfield M, Pradhan RL, et al. (2007) Percutaneous extensor tenotomy for chronic tennis elbow using an 18G needle. Kathmandu Univ Med J 5: 446-448.
- Mishra AK, Skrepnik NV, Edwards SG, et al. (2014) Efficacy of platelet-rich plasma for chronic tennis elbow: A double-blind, prospective, multicenter, randomized controlled trial of 230 patients. Am J Sports Med 42: 463-471.
- Altay T, Gunal I, Ozturk H, et al. (2002) Local injection treatment for lateral epicondylitis. Clin Orthop Relat Res 127-130.
- Jacobson JA, van Holsbeeck MT (1998) Ultrasound-guided interventional procedures in the musculoskeletal system. Musculoskeletal ultrasonography. Orthop Clin North Am 29: 135-167.
- Seng C, Mohan PC, Koh SB, et al. (2016) Ultrasonic percutaneous tenotomy for recalcitrant lateral elbow tendinopathy: Sustainability and sonographic progression at 3 years. Am J Sports Med 44: 504-510.
- Barnes DE (2013) Ultrasonic energy in tendon treatment. Op Tech Orthop 23: 78-83.
Corresponding Author
Enrico Casu, Radiologist, ASST Ovest Milanese, Legnano Hospital, Milan, Italy.
Copyright
© 2018 Casu E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.