Minimally Invasive Radical Prostatectomy: 1000 Cases Performed by a Single Surgeon
Abstract
Purpose
We describe the first 1000 cases of minimally invasive radical prostatectomy performed by a single surgeon in a developing country. Aspects related to the learning curve, technical modifications over time and the transition LRP-RARP were also included.
Materials and methods
Analysis of retrospective data from 1000 patients who underwent LRP, RARP and RSP between 2001-2016. Data of operative and postoperative variables and outcomes were compared between LRP and RARP. Many technical modifications have been made along the period: Mainly number of ports, access approach and dissection techniques. A subanalysis of RSP results was performed too. Postoperative complications were reported following Clavien-Dindo Classification.
Results
In sixteen years, 863 LRP and 137 RARP were accounted. RSP technique was performed in 37 RARP patients. There were no differences in baseline characteristics among 2 groups. Mean operative time was longer to RARP group. However, there was no difference between RSP subgroup and LRP operative time (197 min vs. 194 min; p = 0.61). Hospital length was shorter in RARP (1.8 vs. 2.7; p < 0.001). Perioperative complications were more likely in LRP group-mainly in the first 100 cases. No grade IV-V complications occurred. At 12 months, urinary continence was similar among the groups (91.5% vs. 95.6%; p = 0.05). The subgroup RSP, presented a trend to earlier continence recovery. RARP correlated with better sexual function outcomes (90% vs. 75%; p < 0.001).
Conclusions
In an experienced LRP surgeon, the transition to RARP seems to occur naturally with good oncological and functional results in a midterm analysis. In addition, RARP results are expected to outperform LRP beyond sexual potency in a long-term evaluation. Finally, in the RARP group, those of RSP presented a shorter surgical time with a tendency toward an earlier recovery of continence. Thus, this technique seems to have the potential to offer the best functional results.
Introduction
Radical Prostatectomy (RP) was first described in 1905 by Young, but only at the end of the last century, with the Walsh descriptions of periprostatic anatomy, it became the treatment of choice for localized Prostate Cancer (PCa). Despite great oncologic outcomes, better functional results have been pursued by surgeons since that. In last decades, minimally invasive surgery has spread with oncological outcomes at least similar to open approach [1-3]. Also, the image magnification and better visualization of prostatic anatomy allowed an improvement in dissection which in turn has a close correlation with the functional results.
In developed countries, the Robot-Assisted Radical Prostatectomy (RARP) has received widespread acceptance by patients and physicians and has been established as the standard surgical treatment for localized PCa. However, the high cost involved in this technology is still a huge limitation to its expansion with limited number of da Vinci Surgical System in Latin America according to Intuitive Surgical data. In Brazil for instance, despite the recent expansion of robotic surgery, there are only 30 robotic devices available, thus only few people are covered by this technology. Taking that into account and driven by patients desire for more minimally invasive approaches, several centers in Brazil has been performing Laparoscopic Radical Prostatectomy (LRP) as the therapy of choice in prostate cancer treatment [4].
We describe the first 1000 cases experience of a single surgeon in these minimally invasive treatments of prostate cancer in a developing country. Aspects related to technique modifications over time were also included.
Materials and Methods
This is a retrospective analysis of prospectively collected data of first 1000 minimally invasive radical prostatectomies performed by a single surgeon in sixteen years (2001-2016). In this period, LRP procedures were performed in six different hospitals and RARP cases have been performed at private hospitals since 2010.
Many LPR technical modifications have been made along this period. At the beginning, six-port transperitoneal approach with an anterograde dissection was preferred for all cases following Montsouris technique [5]. Then, evolutions related to the learning curve and the surgeons expertise occurred gradually. Main changes occurred in the number of ports, access approach and dissection techniques (retrograde and mixed were also included) [6]. Since 2009, our standard is a four-to-five-port extraperitoneal approach as previously described [7]. Vesicourethral anastomosis is performed following van Velthoven technique. No posterior reconstruction or anterior suspension stitch has been performed. Bilateral neurovascular bundles preservation has been carried out in all cases of localized disease. In cases where macroscopic extracapsular extension is present unilaterally, contralateral neurovascular bundle preservation has been performed. In high-risk patients with bilateral disease, partial neurovascular preservation is attempted but if there is bilateral extracapsular extension no preservation is pursued. Extended pelvic lymphadenectomy has been performed in cases which the risk of positive lymph nodes is greater than 5% at Briganti nomogram, through transperitoneal access with an additional port.
In RARP cases, both S and Si da Vinci Robotic Systems (Intuitive Surgical, Sunnyvale, CA) has been used. Conventional transperitoneal six-port approach has been performed in all cases according to Menon and cols. technical description without any posterior reconstruction step or anterior stitch. We perform anastomosis similar to van Velthoven technique, but two threads at 5:30 and 6:30-o'clock position run to 11:00-o'clock position. We have performed Retzius-Sparing technique (RSP) as described by Galfano, et al. in selected low- and intermediate-risk cases, since 2016 [8]. Closure of Denonvillier fascia was performed as an additional step in first 10 cases.
Data regarding to operative time, transfusion rate, intraoperative complications, length of hospital stay, positive surgical margins rates were compared between LRP and RARP. Biochemical Recurrence (BCR) was defined as PSA > 0.2 ng/mL. Positive surgical margins rates were also assessed.
Concerning functional outcomes, urinary continence was defined as 0-1 pads/day at 12 months of follow-up. Patients able to have erectile function enough to a vaginal penetration at 12 months were considered sexually potent. Postoperative complications were reported following Clavien-Dindo Classification [9].
Student's t-test was used to continue variables, while categorical variables were statistically analyzed by chi-square test. All tests of significance were two-tailed, and the significance level was defined as α = 0.05. Analyses were conducted using the R statistical package v.3.3.3 (R Foundation for Statistical Computing, Vienna, Austria).
Results
Baseline demographics
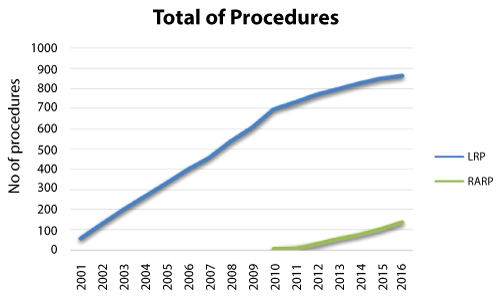
The Table 1 shows preoperative clinical characteristics of both LRP and RARP groups. In sixteen years, 863 LRP and 137 RARP procedures were included. RSP technique was performed in 37 of RARP cases. There were no differences in mean age, BMI, clinical stage, PSA level and Gleason score among the groups. Most of patients were classified as low-risk group (49.3% and 50.3%, respectively for LRP and RARP). The curves on Figure 1 show the number of procedures per year during this period.
Perioperative data
Mean operative time was longer in RARP group compared to LRP group (222 min vs. 194 min; p < 0.001), but not if considered only the 37 RSP cases (RSP 197 min vs. LRP 194 min; p = 0.61). Operative time was longer in obese patients and in those underwent to Extended Lymphadenectomy (eLND). In that scenario, mean operative time in RARP group was even longer than LRP group. Extended lymphadenectomy was performed in 25.8% of LRP patients and 31.3% of RARP patients. The median number of lymph nodes yield after extended lymphadenectomy in both groups was similar (LRP: 11 (5-16) vs. RARP: 13 (6-18); p = 0.21). There were no significant differences in blood loss (LRP: 209 mL vs. 226 mL; p = 0.30) and transfusions rates (LRP: 6.3% vs. RARP: 2.9%; p = 0.11) among the groups. Bilateral Neurovascular Bundle (NVB) preservation was performed in 75.3% of LRP and 82.4% of RARP patients (p = 0.06). Time to discharge was shorter in RARP group (1.8 vs. 2.7; p < 0.001). However, there was no difference in hospital length between procedures performed from 2010 onwards.
Perioperative complication rates were higher in LRP group, as showed in Table 2. Most of complications were classified as grade I and in LRP group it was more likely in first 100 cases. Overall complication rates were 25.7% in LRP and 9.4% in RARP groups (p < 0.001), however no difference was seen considering procedures performed from 2010 onwards. Grade III complications were similar among the groups (around 0.7%). Lymphocele (around 0.3%) and urinary leakage (around 0.2%) were the two more frequent complications, without differences among the groups. There were no grade IV-V complications in both groups.
Oncological and functional outcomes
Oncological and functional results are shown in Table 3. Positive margin status was present in 10.6% and 9.3% for pT2 and 24.7% and 23.4% for pT3 disease in LRP and RARP groups, respectively (p = 0.80). In this series, RSP group had lower rate of positive surgical margins than conventional RARP (Table 4). Total Biochemical Recurrence Rate (BCR) was 21.5% in LRP group and 16.4% in RARP group (p = 0.2) in different follow-up period. Mean follow-up was 96 months for LRP and 36 months for RARP patients. In LRP group 592 of 651 (90.1%) patients that complete 3-yrs of follow-up were free of BCR at this time. On the other hand, 53 of 59 (89.8%) patients were BCR-free at the same time.
Urinary continence after 12 months was slightly greater in RARP than LRP group (95.6% vs. 91.5% respectively; p = 0.05). Bilateral nerve-sparing patients had higher urinary continence rates, showing the role of preservation in urinary continence. The difference between RARP and LRP was sustained in this subset, but no statistically significant difference was seen as less number of patients was analyzed. There was a trend in earlier urinary continence recovery favoring RARP group, especially in RSP subgroup (RSP 97.3% vs. LRP 87% at 3 months; p = 0.06). When compared RSP and conventional RARP, there was also a trend toward earlier urinary continence recovery in RSP group (RSP 97.3% vs. cRARP 89% at 3 months; p = 0.12), as showed in Table 4. Sexual function recovery was more likely after RARP. At 1 year, 75% of previous sexual potent patients that underwent bilateral nerve sparing procedure were potent in LRP Group and 90% in RARP Group (p < 0.001), regardless of oral medication use. RARP conventional approach showed no difference in sexual function in comparison to RSP subgroup (RSP 91.9% vs. cRARP 89.5%; p = 0.67).
Discussion
Although LRP has been successful in providing the benefits of minimally invasive surgeries while keeping the functional results of the open approach, several inherent aspects of laparoscopy as its steep learning curve have limited its expansion.
RARP have overcome these aspects by providing ergonomics and multi-joints devices with increased degree of movements. Also, RARP has proven to decrease the learning curve of LRP. According to literature, LRP learning curve for oncological outcomes reaches plateau at approximately 200 to 250 cases and the number of cases required to achieve proficiency ranges from 200 to 700 [10-12]. Regarding RARP, several authors demonstrated that a laparoscopically naïve surgeon reaches an initial learning curve after 12-18 cases [13-15]. Therefore, RARP procedures became the preferred surgical approach for prostate cancer worldwide.
Even with those benefits, the expansion of robotic surgery has an important limiting factor: Its cost. Despite of this, developing countries such as Brazil have been showing an increasing number of robotic procedures within a transition phase in which all prostatectomy approaches are performed (Open, laparoscopic and robotic-assisted). As noted in Figure 1, the LRP curve reaches a plateau while the RARP curve shows an annual growth trend. However, most radical prostatectomies in Brazil have been yet performed by open approach.
Several multi-institutional and multi-professional studies have compared LRP and RALP oncological and functional outcomes. Our study shows the experience of a single surgeon who remains performing both techniques.
We must consider some factors when analyzing these results, such as the influence of surgeon's learning curve. For instance, a greater number of complications and length of hospital stay was detected in the LRP group, otherwise, when only the last cases of both groups were considered, the complication rates were equivalent. Thus, the transition from the LRP technique to RARP at least in experienced surgeons seems to be safe: A low level of complications has been seen even in earlier cases. Previous studies in high volume centers had already verified this and now it was confirmed in a slower RARP transition scenario [4,16].
Many technical modifications have been made along the way in both LRP and RARP. In LRP we have reduced the number of ports since we increased our expertise. Transperitoneal approach allows a larger field to work, but we have adopted extraperitoneal approach as standard, since we have noted faster recovery in those patients. If extended lymphadenectomy is needed we still prefer transperitoneal access. After many attempts, we are sure van Velthoven technique is the best way to perform vesicourethral anastomosis laparoscopically. Since we have had great functional outcomes with the technique performed we had not seen benefits with additional steps as posterior reconstruction, but further studies would be necessary.
In RARP, a well established conventional technique was initially adopted at the beginning of the learning curve. As one has been experienced in RARP, other techniques can be performed. Currently, RSP has been purposed for low- and intermediate-risk patients and we presented only our preliminary data regarding this more recent approach. At this moment, we are leading a prospective study comparing RSP with conventional RARP.
There are some tips a laparoscopic surgeon must keep in mind while the transition to RARP. First, the surgeon should not try to reproduce the laparoscopic surgery with the robot-device. RARP allows a closer view of anatomical structures that must be enjoyed. Dissection in RARP must be handled with both first and second arms, thus exposure is in charge of the fourth arm, as opposed to LPR. Follow a well described RARP technique is essential, at least at the beginning of learning curve, so the new RARP surgeon can avoid habits brought from LRP. We must emphasize that although robotic surgery is a technological advance that can smooth the minimally invasive procedures learning curve, robotic surgeons have yet a learning curve to pursue. It is especially correlated to the system features such as multi-joints devices and absence of tactile feedback.
In our series, RARP operative time was longer in comparison to LRP, following what has been seen in several series. Procedures performed in obese or in patients who underwent eLND are longer for obvious reasons and differences in time related to the approach were sustained. A similar and adequate number of lymph nodes was retrieved in both techniques, thus either RARP or LRP are suitable to perform eLND. RSP subgroup shorter operative time is probably related to surgeon robotic expertise when the technique was introduced and to inherent aspects of this approach.
Positive surgical margins were more likely in first cases in both approaches, as it is related to surgeon expertise. It trends to reduce along the learning curve, but one should keep in mind that pursuing an extremely preservative surgery must lead to higher positive margins rates. Higher rates of positive margins in RARP compared to RSP are probably related to greater surgeon expertise when performing RSP. A BCR-free comparison between LRP and RARP groups is unsuitable because of RARP group short follow up. At 3 years of follow-up BCR data are comparable. High rates of urinary continence in LRP group did not allow us to show differences in this outcome, although there is a trend toward better urinary continence results in RARP group, especially earlier outcomes in RSP subgroup. Considering the benefits of RSP are more evident in the first weeks (or even days), our evaluation at 3-12 months had a limited role to assess early functional outcomes [17]. The impact of neurovascular bundle preservation in functional outcomes could not be well stated since we have data of patients with bilateral preservation, but it lacks of details which kind of preservation the other patients underwent. Nevertheless, it has been seen greater urinary continence and sexual potency outcomes in those patients assigned as bilateral neurovascular bundle preservation. RARP group presented greater sexual potency status than LRP, without differences compared to the subgroup RSP. It can be attributed to the experience achieved for the surgeon in preserving neurovascular bundles along his learning curve. There were no others significant differences in oncological and functional out comes between the groups, including bladder catheterization days and margin status.
Previous studies have already demonstrated some benefits of RSP, mainly regarding early recovery of urinary continence [18]. Preserving the anterior compartment (Retzius compartment) which contains several anatomical structures related to the support of the bladder and urethra may be responsible for those early good results.
Although rates of BCR have been similar, there is significantly disparity in follow-up between groups. Long-term rates including disease-specific survival data are required, even so the results achieved can be considered acceptable. Javier and colleagues [15] demonstrated abrupt break-points in RARP learning curves of surgeons experienced in LRP with continued improvement in operative and pathologic parameters as their experience increases. Thus, it is expected that our long-term results of RARP get even better.
Limitations of the current study are the retrospective nature although with prospectively collected data, lack of validated instruments to assess urinary function and overall sexual function. Also, the disparity among number of patients, follow-up period and the time where procedures were performed are great limitations of our study and make groups comparisons difficult. However, a large series of a single surgeon helps one to understand the role of LRP-RARP transition in real life and to get some tips and tricks to do your own transition. Some favorable aspects are the long period of study, the use of a tool to report complication rates and despite some changes in the team over time, all procedures were performed by a single surgeon.
Conclusion
In a LRP experienced surgeon, transition to RARP seems to occur naturally, warranting similar or better oncological and functional results with a similar complication rate in a midterm analysis. Also, as the surgeon progress in learning curve, it is expected that RARP outcomes, especially functional ones, overcome those achieved with LPR. Finally, the subgroup Retzius-sparing presented shorter surgical time with a trend toward earlier recovery of urinary continence even in the early learning curve. We believe this technique has the potential to offer the best functional outcomes in selected patients.
References
-
Schuessler WW, Schulam PG, Clayman RV, et al. (1997) Laparoscopic radical prostatectomy: Initial short-term experience. Urology 50: 854-857.
-
Guillonneau B, Rozet F, Barret E, et al. (2001) Laparoscopic radical prostatectomy: Assessment after 240 procedures. Urol Clin North Am 28: 189-202.
-
Poulakis V, Dillenburg W, Moeckel M, et al. (2005) Laparoscopic radical prostatectomy: Prospective evaluation of the learning curve. Eur Urol 47: 167-175.
-
Tobias-Machado M, Mitre AI, Rubinstein M, et al. (2016) Robotic-assisted radical prostatectomy learning curve for experienced laparoscopic surgeons: Does it really exist? Int Braz J Urol 42: 83-89.
-
Guillonneau B, Vallancien G (2000) Laparoscopic radical prostatectomy: The Montsouris technique. J Urol 163: 1643-1649.
-
Tobias-Machado M, Forseto P Jr, Medina JA, et al. (2004) Laparoscopic radical prostatectomy by extraperitoneal access with duplication of the open technique. Int Braz J Urol 30: 221-226.
-
Starling ES, Reis LO, Vaz Juliano R, et al. (2010) Extraperitoneal endoscopic radical prostatectomy: How steep is the learning curve? Overheads on the personal evolution technique in 5-years experience. Actas Urol Esp 34: 598-602.
-
Galfano A, Di Trapani D, Sozzi F, et al. (2013) Beyond the learning curve of the Retzius-sparing approach for robot-assisted laparoscopic radical prostatectomy: Oncologic and functional results of the first 200 patients with 1 year of follow-up. Eur Urol 64: 974-980.
-
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications. Ann Surg 240: 205-213.
-
Secin FP, Savage C, Abbou C, et al. (2010) The learning curve for laparoscopic radical prostatectomy: An international multicenter study. J Urol 184: 2291-2296.
-
Martínez-Pineiro L, Caceres F, Sanchez C, et al. (2006) Learning curve of laparoscopic radical prostatectomy in a University Teaching Hospital: Experience after the First 600 Cases. Eur Urol Suppl 5: 914-924.
-
Sandhu GS, Nepple KG, Tanagho YS, et al. (2013) Laparoscopic prostatectomy for prostate cancer: Continued role in urology. Surg Oncol Clin N Am 22: 125-141.
-
Menon M, Shrivastava A, Tewari A, et al. (2002) Laparoscopic and robot assisted radical prostatectomy: Establishment of a structured program and preliminary analysis of outcomes. J Urol 168: 945-949.
-
Ahlering TE, Skarecky D, Lee D, et al. (2003) Successful transfer of open surgical skills to a laparoscopic environment using a robotic interface: Initial experience with laparoscopic radical prostatectomy. J Urol 170: 1738-1741.
-
Jaffe J, Castellucci S, Cathelineau X, et al. (2009) Robot-assisted laparoscopic prostatectomy: A single-institutions learning curve. Urology 73: 127-133.
-
Park JW, Lee HW, Kim W, et al. (2011) Comparative assessment of a single surgeon's series of laparoscopic radical prostatectomy: Convetional versus robot-assisted. J Endourol 25: 597-602.
-
Dalela D, Jeong W, Prasad MA, et al. (2017) A Pragmatic Randomized Controlled Trial Examining the Impact of the Retzius-sparing Approach on Early Urinary Continence Recovery After Robot-assisted Radical Prostatectomy. Eur Urol.
-
Lim SK, Kim KH, Shin TY, et al. (2014) Retzius-sparing robot-assisted laparoscopic radical prostatectomy: Combining the best of retropubic and perineal approaches. BJU Int 114: 236-244.
Corresponding Author
Marcos Tobias-Machado, MD, PhD, Head, Section of Urologic Oncology, Department of Urology, ABC Medical School, Rua Grauna, 104 ap 131, Sao Paulo, SP, Brazil, ZIP: 04514-000, Tel: +55-11-9932-9944.
Copyright
© 2017 Tobias-Machado M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.