Hepatorrhexis with Bleeding and Shock Twice of Choriocarcinoma: A Case Report
Abstract
Gestational trophoblastic neoplasia (GTN) derives from the abnormal proliferation of placental trophoblastic cells and it has various of clinical manifestations. However, some patients have had the metastases before admitted to hospital or see the doctor due to the metastatic site symptom. Here we report a case of a young woman followed fatal hepatorrhexis with haemorrhage and shock twice after admitted to hospital and she is diagnosed as choriocarcinoma with liver and lung metastasis finally.
Keywords
Hepatorrhexis, Gestational trophoblastic neoplasia, choriocarcinoma, Liver metastasis, Lung metastasis
Introduction
Gestational trophoblastic neoplasia (GTN) derives from the abnormal proliferation of placental trophoblastic cells, including invasive hydatidiform mole, choriocarcinoma (CC), placental site trophoblastic tumor and epithelioid trophoblastic tumor [1]. GTN has various of clinical manifestations, for instance irregular vaginal bleeding, uneven uterine enlargement and abdominal pain. However, some patients have had the metastasis of vagina, lung, liver, brain et al. due to different histological types before admitted to hospital [2].
GTN can be diagnosed after any type of pregnancy, approximately 50% hydatidiform mole, 25% miscarriage or ectopic pregnancy, and 25% term or preterm delivery [3]. It is necessary to pay attention to the continuous high-level of human chorionic gonasotropin (HCG) in the context of various pregnancy. If not, it can endanger the life of patients. Choriocarcinoma is a rare and highly malignant neoplasm with mixed proliferation of cytotrophoblasts, syncytiotrophoblasts and intermediate trophoblasts, which has a stronger ability to destroy blood vessels both local site and metastasize via blood channels. Many organs and tissues can be disturbed, such as lung (80%), vagina (30%), liver (10%) and brain (10%) [4]. The pathological features of choriocarcinoma are that the hyperplastic trophoblast cell invades myometrium and veins accompanied by extensive hemorrhage, necrosis and distant metastasis. No villus can be seen under the microscope [5].
Here we report a case of a young woman in the setting of life-threatening hepatorrhexis with haemorrhage and shock twice and she was diagnosed as choriocarcinoma with liver and lung metastasis finally.
Case Presentation
A 29-year-old woman with amenorrhea, elevating HCG that is 12000 IU/L (0-7IU/L) and minor vaginal bleeding presented to the hospital. Considering "ectopic pregnancy", she was administered at a local hospital by right partial ovariectomy under laparoscopy. Pathological results showed that no excellent villi were noted. However, the HCG levels rose to 300000 mIU/ml and she was transferred to a tertiary care center. Two infants were delivered in full term in 2012 and 2014, and curettage was performed after medical abortion in 2018.
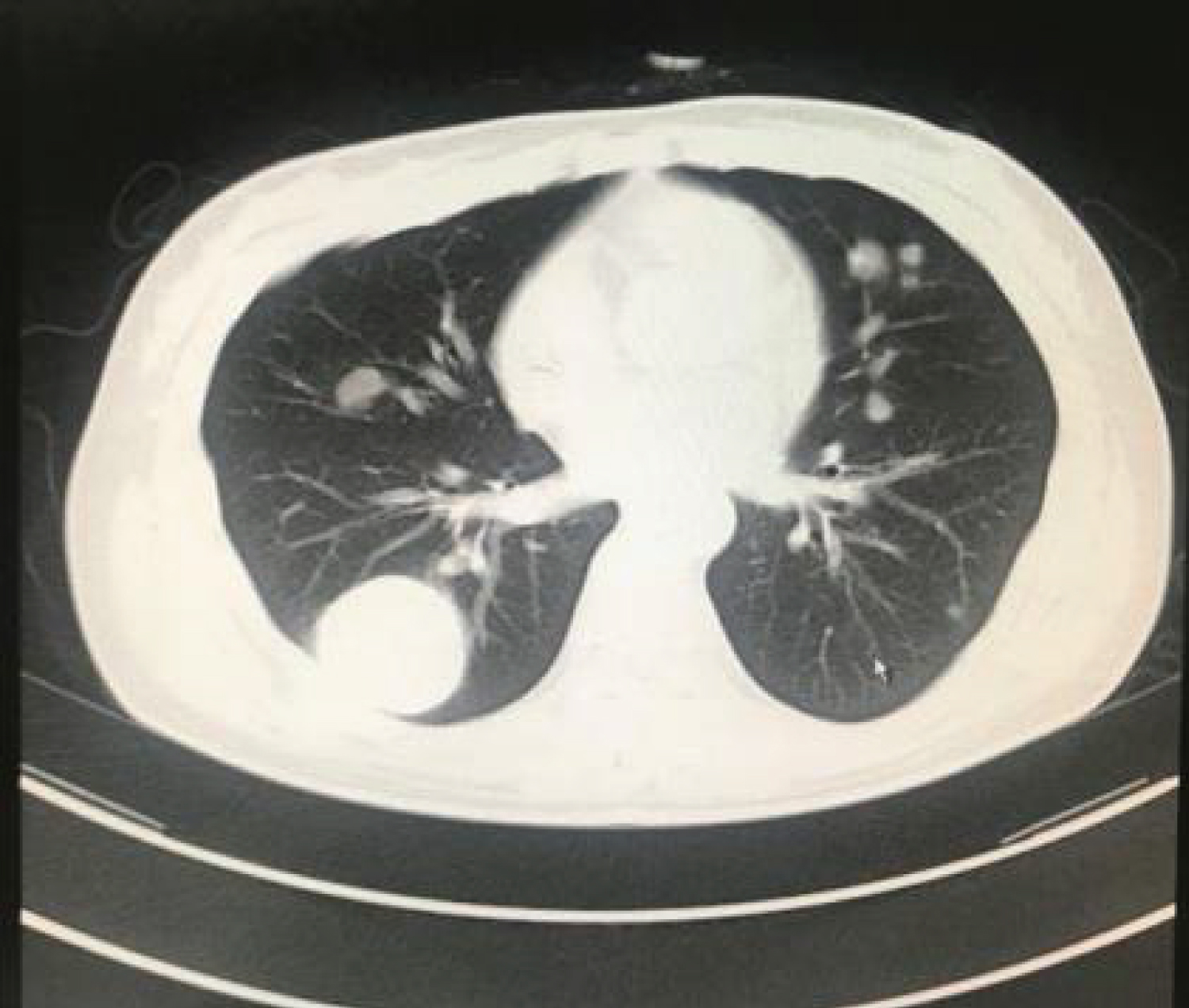
The relevant inspection was performed as soon as she was admitted. Chemical examinations revealed blood HCG of 564600 mIU/ml (0-3 mIU/ml) and normalized liver function. Pertinent findings on the chest CT scan (Figure 1) revealed multiple quasi-circular high density shadows in bilateral pulmonary, and her abdomen CT scan revealed a change of liver and spleen. Prior to initiation of diagnosis, patient was rescued with increased heart rate, decreased blood pressure, severe abdominal distension with nausea and vomiting and near syncopal episodes, except remarkable diffuse tenderness and rebound. Whole abdominal ultrasound immediately revealed massive hematocele and blood clots in the pelvic and abdominal cavity, A 11 cm space occupying lesion on the liver. Nonthrombogenic approximately 20 ml was withdrawn by diagnostic abdominocentesis. Considering the rupture of liver metastases, we stabilized the patient with transfusion of blood products and interventional embolization simultaneously. After this operation, the reason why the patient underwent laparotomy is that she suffered from progressive blood loss, which found a 15 cm mass in the left lateral lobe of the liver and a 2 cm diameter rupture near the round ligament of the liver. Postoperative histopathology rooted from left lateral lobectomy of liver revealed choriocarcinoma consistent with hemorrhage and necrosis. Follow-up HCG showed 43909 mIU/ml and PET-CT considered both liver and lung metastases. The patient was diagnosed with high-risk IV: 13 according to the Federation of Gynecology and Obstetrics (FIGO) and treated with EMA (Etoposide + Methotrexate + Actinomycin-D) and EMA-CO (Etoposide + Methotrexate + Actinomycin-D/Vincristine + Cyclophosphamide) chemotherapy regimen.
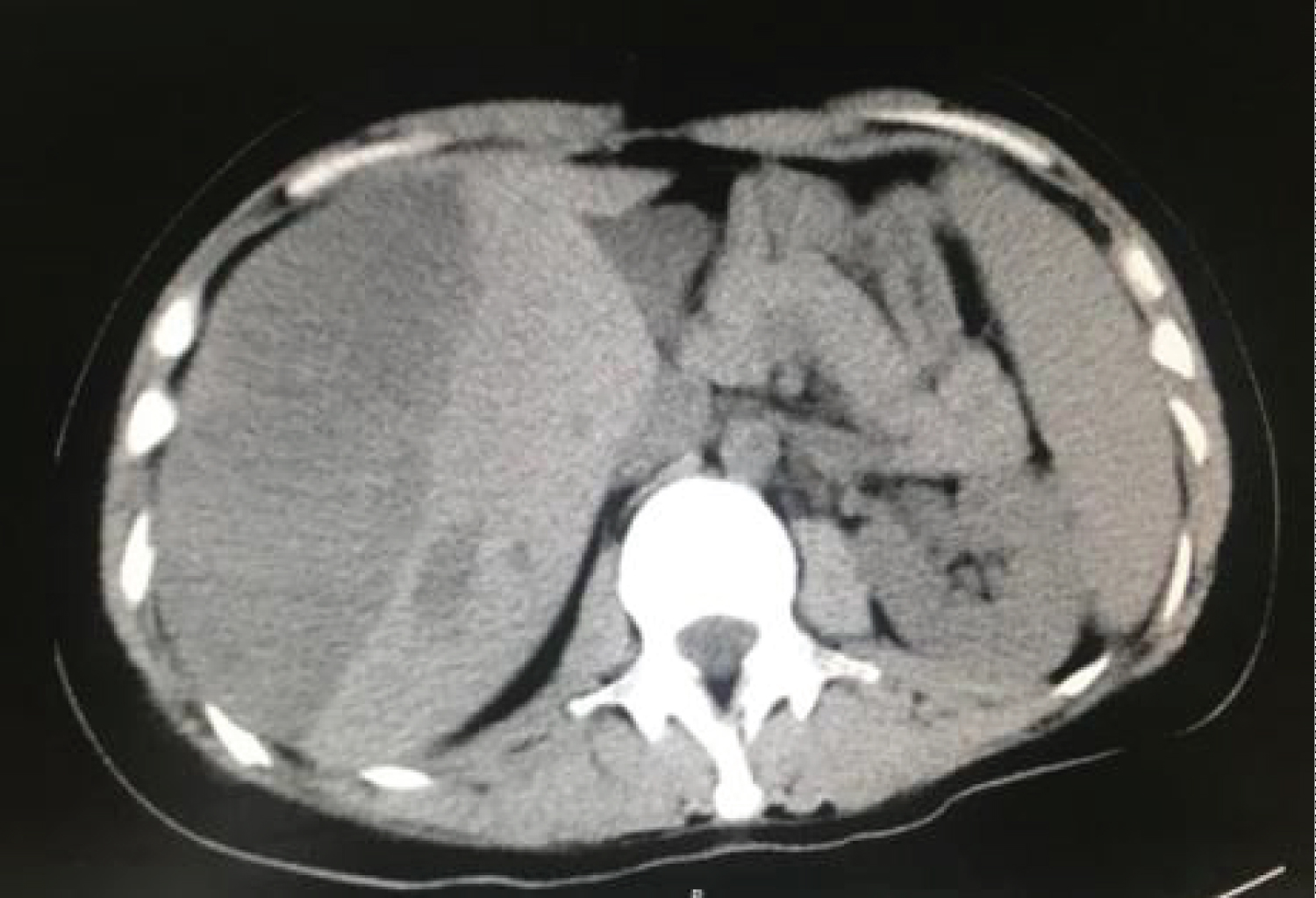
Upper abdominal discomfort, increased heart rate and decreased blood pressure appeared again during chemotherapy. The whole abdominal CT (Figure 2) revealed changes in liver, spleen and pancreas and multiple nodules in both lungs. In consider of sub capsular hematoma of the liver at this time, we managed the woman by anti shock and hemostasis again for ruptured liver metastases.
Another 3 cycles of chemotherapy regimen was performed after the last operation. The clinical treatment effect is obvious, HCG was normal and chest and abdominal CT scan indicated that all metastatic lesions were narrow significantly. Although she received 4 additional cycles for consolidation with EMA-CO regimen, the metastatic heterogeneous mass still existed in liver. At present, the woman has survival with tumors over 8 months during follow up visit.
Discussion
Clinical manifestations of choriocarcinoma with liver metastasis
There are no obvious symptoms and signs of liver metastasis at choriocarcinoma in the early stage [6]. Poor appetite, discomfort or dull pain, hepatomegaly and tenderness only appear in the terminal period but liver function and jaundice is rarely abnormal. Although the diagnosis of advanced liver metastasis is not difficult, once the disease progresses to the terminal stage of liver metastasis, its recovery is extremely terrible. Providing that liver metastasis expand which will rupture and hemorrhage, most of which appear on the sub capsular liver, sufferers might feel hepatalgia on that time. Metastasis may also rupture directly to the abdominal cavity, which leads to drop dead rapidly but rarely.
The patient with normal liver function, hepatorrhexis and shock as the first symptom consistent with advanced hepatic metastases. After the first operation due to hepatorrhexis and shock, the patient was out of danger and recovered well by second surgical operation as a result of the rupture and haemorrhagia of the metastatic nidus again. What the incidence of secondary rupture in choriocarcinoma with liver metastases is exceedingly low, there are few case reports concerning that. This case presentation enriches the clinical manifestations of liver metastasis of choriocarcinoma, and provides reference for the diagnosis and treatment of later patients.
Diagnosis of choriocarcinoma with liver metastasis
Auxiliary examinations including radionuclide hepatic scanning and computed tomography (CT) contribute to preliminary diagnosis of liver metastasis of choriocarcinoma. Positron emission tomography (PET) can detect micro metastasis. When there is fatal haemorrhage originated from metastatic lesions, feasible laparotomy could be used to confirmed.
Treatment of choriocarcinoma with liver metastasis
Patients will be categorized by FIGO Stage and WHO risk score, which dictate the initial treatment regimen. "FIGO Cancer Report 2015" proposed a new concept involving extra high-risk GTN [7] that is defined as patients with metastasis in liver, brain or extensive areas or score ≥ 12. May [8] reported that the survival rate of patients with stage IV in the New England Trophoblastic Disease Center was only 30% before 1975 and then the rate increased to 80% due to the application of multiple combination chemotherapy. GTN is the only gynecological malignant tumor that can be cured by chemotherapy at present and the EMA-CO regimen is the optimal choice. In consider of various clinical scenario, a protocol of low dose induction chemotherapy with cisplatin and etoposide can be initial.
As the tumor is sensitive to chemotherapy regimen, there is large tumor burden and risk of rupture and hemorrhage of liver metastases from rapid tumor destruction from full dose chemotherapy, which is the most serious complication. Selective hepatic artery embolization can be used to temporize bleeding when hemorrhage occurred [9]. In addition, embolization is more effective to multiple metastases and chemotherapy combined with lesionectomy can improve the therapeutic effect on the limited, resistant and recurrent lesions. Chen Chen [10] reported that patients were treated with systemic chemotherapy and selective hepatic arterial intubation chemotherapy, three patients had hemostasis after embolization, two patients complete remission and one serological remission (the metastasis still exists, and alive with tumor). During the second course of chemotherapy, hepatic metastasis rupture and bleeding occurred again which was defined as the early complication on account of that the tumor cells are sensitive to chemotherapy. The patient still alive with tumor now.
In summary, the possibility of GTN should be considered for reproductive woman with abnormal elevation level of HCG, especially those with a recent history of fertility. Detailed medical history, comprehensive physical examination, gynecological Doppler ultrasound and HCG are all conducive to the diagnosis of this disease. Liver metastases of GTN are often combined with other organs metastasis, therefore standardized combination chemotherapy is the optimal treatment for liver metastasis. According to the clinical characteristics of illness, individual therapy could be selected, for example, hepatic artery embolization or hepatic lobectomy, which can not only save lives but create opportunities for further treatment.
References
- Yang X, Fang J (2020) Progress in drug therapy of gestational trophoblastic tumor. Chinese Journal of Practical Gynecology and Obstetrics 36: 25-28.
- Huifei W, Yujing G, Yi L, et al. (2019) A case of gestational trophoblastic tumor with cerebral hemorrhage as the first manifestation. Journal of International Obstetrics and Gynecology 46: 670-673.
- Braga A, Mora P, de Melo AC, et al. (2019) Challenges in the diagnosis and treatment of gestational trophoblastic neoplasia worldwide. World J Clin Oncol 10: 28-37.
- Xing X, Jianhua Q, Zhiming D, et al. (2006) Gestational Trophoblastic Disease. Progress in Obstetrics and Gynecology 2006: 241-256.
- Yang X, Qi Z, Xiaohua W, et al. (2018) Guidelines for diagnosis and treatment of gestational trophoblastic disease. (4th edn). Chinese Journal of Practical Gynecology and Obstetrics 34: 994-1001.
- Yang X (2011) Trophoblastic Oncology of Song Hongzhao. (3rd edn), Beijing: People's Medical Publishing House, 2011: 208-209.
- Ngan HY, Seckl MJ, Berkowitz RS, et al. (2015) Update on the diagnosis and management of gestational trophoblastic disease. Int J Gynaecol Obstet 131: S123-S126.
- May T,Goldstein DP,Berkowitz RS (2011) Current chemotherapeutic management of patients with gestational trophoblastic neoplasia. Chemother Res Pract 2011: 806256.
- Lok CA, Reekers JA, Westermann AM, et al. (2005) Embolization for hemorrhage of liver metastases from choriocarcinoma. Gynecol Oncol 98: 506-509.
- Chen C, Yang X (2020) Selective hepatic artery catheterization for the treatment of 8 cases of hepatic metastasis of trophoblastic tumor. Journal of New Medicine 540-541.
Corresponding Author
Yicun Pang, Department of Obstetrics and Gynecology, The Third Hospital of Hebei Medical University, No. 139, Zhongshan West Road, Qiaoxi District, Shijiazhuang City, Hebei Province 050011, China.
Copyright
© 2022 Zhang Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.