The Combination of Sufentanil and Remifentanil on Hemodynamic Changes during Anesthetic Induction and Endotracheal Intubation
Abstract
Introduction: A low dose of sufentanil was insufficient to suppress endotracheal intubation (ETI) induced cardiovascular response. This study investigated the effects of combined sufentanil and remifentanil on hemodynamic changes during anesthetic induction and ETI.
Methods: 70 adult patients were divided into two groups (n = 35). General anesthesia was induced by sufentanil, propofol, and cisatracurium. Group S received sufentanil 0.3 mcg/kg, while Group R received sufentanil 0.3 mcg/kg and remifentanil 1 mcg/kg. The systolic arterial pressure (SAP), diastolic arterial pressure (DAP), mean arterial pressure (MAP), and heart rate (HR), incidence and severity of hypotension, hypertension, bradycardia, and tachycardia, doses of propofol during anesthetic induction and ETI were compared.
Results: After anesthetic induction, the changes of SAP, DAP, MAP and HR were comparable between the groups (p > 0.05). Right after ETI, the HR in Group R was significantly lower than Group S (p < 0.001). 5 min after ETI, the SAP, DAP, and MAP in Group R was significantly higher than Group S (p < 0.03). The incidence and severity of hypotension, hypertension, bradycardia, and tachycardia was comparable between the groups (p > 0.07). The dose of propofol used in Group R was significantly lower than Group S (p = 0.001).
Conclusion: The combination of sufentanil and remifentanil is superior to sufentanil alone for attenuating ETI induced cardiovascular response without cardiovascular compromise.
Keywords
Remifentanil, Sufentanil, Induction, Intubation
Introduction
Anesthetic induction and endotracheal intubation (ETI) can cause hemodynamic fluctuation. Achieving a stable hemodynamic profile during anesthetic induction and ETI is important to anesthetists in daily practice [1,2]. Opioids in combination with propofol are widely used for suppressing ETI induced cardiovascular response during anesthetic induction [3]. Sufentanil, an analog of fentanyl, is a proper opioid for anesthetic induction because of less impact on hemodynamics. A previous study showed that sufentanil dose-dependently suppressed ETI induced cardiovascular response [4]. However, a low dose of sufentanil combined with propofol is inadequate to well suppress ETI induced increase of heart rate (HR) and blood pressure (BP) [4]. On the other hand, although a larger dose of sufentanil may effectively suppress the increase of HR and BP induced by ETI, it may prolong the patient emergence from anesthesia and may lead to respiratory depression after a short surgery because the analgesic duration of sufentanil is long (30 to 50 min) [5,6]. Hence, it is reasonable to use an additional drug to suppress cardiovascular response induced by ETI during low dose sufentanil based anesthetic induction.
Remifentanil is another kind of opioid, which has a short time of onset and elimination [7]. It is also widely used for anesthetic induction and ETI [3]. However, a low dose of remifentanil is also inadequate to suppress ETI induced cardiovascular response. On the other hand, a larger dose of remifentanil may induce severe hypotension and bradycardia [8-10]. Previous studies showed that remifentanil suppressed ETI induced cardiovascular response better than sufentanil, however, with more adverse cardiovascular depression [3,10]. Based on the characteristics of sufentanil and remifentanil, we hypothesized that using a low dose of sufentanil for anesthetic induction and adding a low dose of remifentanil for ETI may provide a relatively stable hemodynamic profile. To the best of our knowledge, the relevant study is limited. Therefore, the present study was to investigate the effects of combined sufentanil and remifentanil on the hemodynamic changes during anesthetic induction and ETI.
Methods
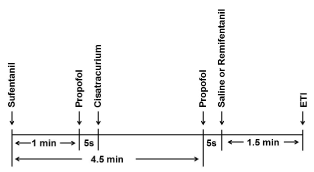
The randomized, single blind, controlled clinical trial was approved by the Ethics Committee of Hunan Provincial People's Hospital. After consents were obtained, 70 patients scheduled for elective surgery who were aged 18-65 years with American Society of Anesthesiologists (ASA) physical status I-II were recruited. Exclusion criteria included: Predicted difficult airway, body mass index (BMI) ≥ 30 kg/m2, cardiovascular disease, cardiac arrhythmia, respiratory disease, cerebral disease, and alcohol abuse. No premedication was given to the patients before surgery. On arrival in the operating room, the patients were monitored by electrocardiography, non-invasive BP, and pulse oximetry. Ringer's solution was infused at a rate of 4 - 6 mL/min via a peripheral intravenous line. When the patients were preoxygenated via a facemask with a fresh gas flow of 6 L/min, sufentanil (Yi chang Human well Pharmaceutical Co, Ltd, Hubei, China) 0.3 mcg/kg (5 mcg/ml) was injected intermittently in 30 seconds in case of cough. 1 min after the completion of sufentanil injection, propofol (10 mg/ml) 0.4-1 mg/kg (depending on the ages) was injected in 5 seconds followed by injection of cisatracurium 0.2 mg/kg (2 mg/ml) in 10 seconds. After the loss of consciousness, the patients were ventilated manually. The patients were randomized into 2 groups according to computer-generated random numbers (n = 35): Group S: 4.5 min after the completion of sufentanil injection, a bolus of propofol 1-2 mg/kg (depending on the age and the BP after the first injection of propofol) was injected in 5 seconds. 5 seconds later, a bolus of saline (0.1 ml/kg) was injected in 10 seconds. Group R: 4.5 min after the completion of sufentanil injection, a bolus of propofol 0.2-1 mg/kg (depending on the age and the BP after the first injection of propofol) was injected in 5 seconds 5 seconds later, a bolus of remifentanil (Yi chang Human well Pharmaceutical Co, Ltd, Hubei, China) 1 mcg/kg (10 mcg/ml) was injected in 10 seconds. 1.5 min after the injection of saline or remifentanil, oral ETI assisted by a video-laryngoscope was performed by an experienced anesthetist in 30 seconds (Figure 1). The cuff of the tube was inflated immediately after ETI. Anesthesia was maintained by inhalation of sevoflurane with an inhaled concentration of 0.7-1.5% (depending on the age and the BP after ETI).
The systolic arterial pressure (SAP), diastolic arterial pressure (DAP), mean arterial pressure (MAP), and HR were recorded at 6 time points:
T0: The baseline before anesthetic induction.
T1: 1 min after the first bolus of propofol.
T2: 1 min after saline or remifentanil injection.
T3: Right after inflating the cuff of endotracheal tube.
T4: 2 min after ETI.
T5: 5 min after ETI.
During the anesthetic process, atropine 0.2-0.5 mg was injected for HR < 45 bpm before ETI (because laryngoscopy may aggravate bradycardia), dopamine 1-2 mg was injected for SAP < 80 mmHg. SAP ≥ 180 mmHg or HR ≥ 100 bpm after ETI was considered to be inadequate anesthesia and propofol 30-50 mg was injected. The incidences of hypotension (MAP < 65 mmHg), hypertension (SAP ≥ 180 mmHg), bradycardia (HR < 50 bpm), and tachycardia (HR ≥ 100 bpm) in each group before ETI (T0, T1, T2) and after ETI (T3, T4, T5) were also recorded. The severity of hypotension were categorized into MAP < 65, MAP < 60, and MAP < 55, the severity of bradycardia were categorized into HR < 50 bpm and HR < 45 bpm. The doses of propofol for anesthetic induction were also recorded.
Statistical Analysis
In our pilot study, an additional low dose of remifentanil 1 mcg/kg could suppress ETI induced HR increase by nearly 10% compared with sufentanil 0.3 mcg/kg alone. With α = 0.05 and β = 0.8,32 patients in each group is required in this study, and we finally included 35 patients in each group. Data were expressed as mean (SD), median (25th, 75th percentiles), number (percentage), and proportion. The normality of data distribution was tested by the Shapiro-Wilk test, the homogeneity of variance was tested by the Levene's test. Comparison of age, weight, height, BMI, and propofol injection dose were analyzed with Student's t-test or the Mann-Whitney U test. The gender, ASA physical status, and incidences of hypertension and tachycardia were compared using Chi-square test or Fisher's exact test. The severity categories of hypotension and bradycardia were compared by the Mann-Whitney U test. Comparison of SAP, DAP, MAP, and HR were analyzed with repeated-measures analysis of variance (ANOVA), multiple comparisons were analyzed using the Bonferroni correction test. SPSS 22.0 (SPSS Inc, Chicago, IL, USA) was used for statistical analysis. A p value of < 0.05 was considered statistically significant.
Results
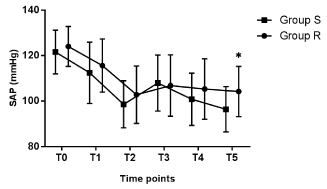
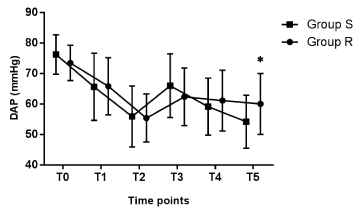
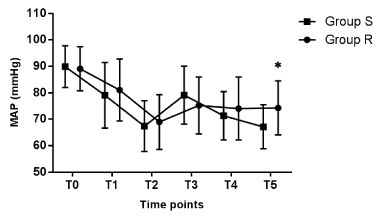
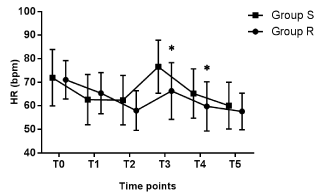
The characteristics of the patients were comparable between the two groups with respect to age, gender, weight, height, BMI, and ASA classification (Table 1). The hemodynamic profiles of the two groups showed that the cardiovascular responses after ETI in Group R were less fluctuated than in Group S. As shown in Figure 2, Figure 3, Figure 4, and Figure 5, the baseline of the vital signs were comparable between the two groups (p > 0.05). After the first injection of propofol, the SAP, DAP, MAP and HR decreased significantly in both of the groups at T1 (p < 0.002) with no significant differences between the groups (p > 0.298). After the second propofol injection, the SAP, DAP, and MAP further decreased at T2 (p < 0.001). In Group R, after the injection of propofol and remifentanil, the HR decreased further at T2 (p = 0.000), while in Group S, the second injection of propofol did not further decrease the HR (p = 1). Right after ETI at T3, the SAP, DAP, MAP, and HR significantly increased in both of the groups (p < 0.002) except for the SAP in Group R was not significantly different compared with T2 (p = 0.318). However, the HR at T3 in Group R was significantly lower than Group S (p = 0.000, Figure 5). 2 min after ETI, the SAP, DAP, MAP, and HR in Group S decreased significantly at T4 (p < 0.002) and further decreased at T5 (p < 0.005). However, the SAP DAP, and MAP in Group R at T4 and T5 were not significantly different compared with T3 (p = 1). Furthermore, at T5, the SAP, DAP, and MAP in Group R were significantly higher than Group S (p < 0.03, Figure 2, Figure 3, and Figure 4). The HR in Group R decreased significantly at T4 (p = 0.003) but did not decreased further at T5 (p = 0.113). Besides, the HR at T4 in Group R was significantly lower than Group S (p = 0.017, Figure 5).
Before ETI, the severity of hypotension and bradycardia were not significantly different between the two groups (p = 0.986 and p = 0.841, respectively). After ETI, the severity of hypotension and bradycardia in both of the groups were similar to those before ETI without significant differences between the groups (p = 0.071 and p = 0.955, respectively). Besides, there was no patient had hypertension (SAP ≥ 180 mmHg) during the anesthetic induction and ETI in both of the groups. Only one patient had tachycardia (HR ≥ 100 bpm) right after ETI at T3 in Group S, while no patient suffered tachycardia in Group R (p = 1, Table 2).
As shown in Table 3, the doses of the first injection of propofol were not significantly different between the two groups (p = 0.115). However, the dose of the second injection of propofol in Group R was significantly lower compared to Group S (p = 0.001).
Discussion
The present study showed that despite significantly suppressed hemodynamics after anesthetic induction, intravenous sufentanil 0.3 mcg/kg was insufficient to suppress ETI induced increase of BP and HR. An additional bolus of 1 mcg/kg remifentanil 1.5 min before ETI attenuated ETI induced increase of BP and HR without significant hemodynamic depression during anesthetic induction. The onset of sufentanil is 1 to 2 min, and 3 to 6 min is needed to reach the peak concentration [5]. To intubate the patient at the peak effect of analgesia, sufentanil was injected firstly in the anesthetic induction, and ETI was performed at least 6 min after the completion of sufentanil injection. On the other hand, it takes 2 to 3 min for intravenous cisatracurium to reach the maximal muscular relaxation for ETI at dosage of 0.2 mg/kg [11], hence cisatracurium was injected after the first bolus of propofol, and manual ventilation was performed after the patient lost consciousness.
Propofol is one of the most widely used anesthetic drugs for anesthetic induction, it possesses rapid onset, fast distribution, and fast elimination profiles after an intravenous bolus injection [12]. However, hypotension is a common side-effect of propofol injection. An intravenous bolus of an induction dose of propofol (2 mg/kg) frequently induces hypotension (MAP < 60 mmHg) with an incidence up to 45% [13]. The mechanism was considered to bepropofol induced sedation, venodilation and cardiac depression [14]. Shah, et al. [15] found that if propofol was injected intermittently, less dosage of propofol was required to achieve the same level of hypnosis with reduced hemodynamic depression during anesthetic induction. Therefore, propofol was injected twice to reduce hemodynamic depression in the present study. The first injection of propofol was for hypnotizing the patient, waiting for sufentanil and cisatracurium to achieve the maximal effect, and to observe if the patient was susceptible to propofol-induced hypotension. The second bolus of propofol was injected for ETI.
Opioids such as fentanyl, sufentanil, and remifentanil could enhance the hypnotic effect of propofol [16]. Therefore, less propofol was needed in combination with opioids for anesthetic induction. In the present study, after the onset of sufentanil, the dose of the first injection of propofol was 0.6 (0.5, 0.7) mg/kg, which effectively hypnotized the patients with a significant decrease of BP and HR. However, the first low dose of propofol was insufficient to provide an adequate depth of anesthesia for ETI, and propofol was eliminated fast after a bolus injection [12]. Therefore, a second bolus of propofol was injected. To perform ETI after 6 min of sufentanil injection, the second bolus of propofol was injected 4.5 min after the completion of sufentanil injection because the maximal hypnotic effect was achieved after 1.5 min of propofol bolus [12]. Hence ETI could be performed at the maximal effects of sufentanil, propofol, and cisatracurium.
The second bolus dose of propofol in Group S was 1.5 (1.1, 1.7) mg/kg, which was based on the total induction dose of propofol (1.5 to 2 mg/kg) [13,15]. Our results showed that the BP in Group P decreased further after the second bolus of propofol.The incidence of MAP lower than 60 mmHg was 25.7% before ETI, which was less than previously reported (45%) [13]. We considered that separated injection of propofol might have less impact on hemodynamics. In addition, we defined hypotension as MAP < 65 mmHg, and was categorized into MAP < 65 mmHg, MAP < 60 mmHg, and MAP < 55 mmHg. This categorization was based on that intraoperative MAP lower than 65 to 55 mmHg was associated with increased risk of postoperative acute kidney injury and myocardial injury [17]. Hence the present study also indicated that despite separated injection of propofol, the incidence of risky hypotension (MAP < 65 mmHg) was still high (45.7%).
Right after ETI, the HR and BP significantly increased at T3, this indicated that the common induction doses of sufentanil and propofol were still insufficient to suppress ETI induced cardiovascular response. Therefore, to suppress the stimulation of ETI in this induction protocol, an additional short acting drug may be helpful. Previous studies showed that a bolus dose of remifentanil 1 mcg/kg and 2 mcg/kg dose dependently suppressed ETI induced cardiovascular response, and 2 mcg/kg of remifentanil was associated with more adverse cardiovascular depression [10,18]. The mechanism might be remifentanil induced depression on baroreceptor reflexes and sympathetic activity [8,10]. Based on the combination of sufentanil, 1 mcg/kg remifentanil was added before ETI in the present study. Since the peak effect of remifentanil was achieved 1.5 min after a bolus injection in adults [7], remifentanil was injected immediately after the second bolus of propofol. Moreover, remifentanil could reduce the dose of propofol required to hypnotize patients [16,19], hence the second bolus dose of propofol was reduced to 0.5(0.3, 0.5) mg/kg, which was based on our pilot study.
In the present study, the BP and HR in Group R decreased further after the bolus of remifentanil with similar incidence and severity of hypotension and bradycardia compared with Group S. The effects may due remifentanil induced sympathetic depression and propofol induced venodilation and cardiac depression [8,10,14]. Right after ETI at T3, the DAP, MAP, and HR increased significantly in the Group R. However, the SAP in Group R did not significantly increase after ETI. Moreover, the HR at T 3 in Group R was significantly lower than Group S. These results indicated that despite similar hemodynamic depression after anesthetic induction, additional remifentanil combined with less propofol was more effective in suppressing ETI induced cardiovascular response.
Furthermore, the BP decreased significantly again after ETI in Group S but not in Group R. Meanwhile, the BP at T5 in Group R was significantly higher than Group S. This difference may due to less propofol use in Group R than Group S. Besides, the incidence and severity of hypotension and bradycardia before or after ETI was not significantly different between the groups, these results indicated that the additional remifentanil combined with a low dose of propofol may cause less hemodynamic fluctuation during sufentanil based induction of anesthesia.
Limitations
There are certain limitations of the present study. First, we did not use invasive blood pressure monitor, hence we could not observe the continuous change of blood pressure during anesthetic induction, and the lowest and highest blood pressure were unable to record. Second, we did not set another group which was consisted with remifentanil, propofol, and cisatracurium because of different protocols for anesthetic induction. Third, we did not test different doses of sufentanil or remifentanil in the anesthetic induction protocol, and the dose of propofol was also different based on the age and BP. Since drug tolerance is correlated with age, titrated doses of different drugs could be individualized [1,7].
Conclusions
The combination of sufentanil and remifentanil is superior to sufentanil alone for attenuating the cardiovascular response induced by ETI without cardiovascular compromise during anesthetic induction. The induction dose of propofol could be reduced.
Acknowledgement
This research is funded by Health and Family Planning Commission of Hunan Province (20200210) and Hunan Provincial Science and Technology Department (2018SK7001).
Authors Contribution
Qian Huang, Le Zhang, and Yan Mou are of equal contribution to this work.
Conflicts of Interest
The authors declare no competing interests.
Source of Funding Statement
This research is funded by Health and Family Planning Commission of Hunan Province (20200210) and Hunan Provincial Science and Technology Department (2018SK7001).
References
- Südfeld S, Brechnitz S, Wagner JY, et al. (2017) Post-induction hypotension and early intraoperative hypotension associated with general anaesthesia. Br J Anaesth 119: 57-64.
- El-Shmaa NS, El-Baradey GF (2016) The efficacy of labetalol vsdexmedetomidine for attenuation of hemodynamic stress response to laryngoscopy and endotracheal intubation. J Clin Anesth 31: 267-273.
- Zhang GH, Sun L (2009) Peri-intubation hemodynamic changes during low dose fentanyl, remifentanil and sufentanil combined with etomidate for anesthetic induction. Chin Med J 122: 2330-2334.
- Choi BH, Lee YC (2016) Effective bolus dose of sufentanil to attenuate cardiovascular responses in laryngoscopic double-lumen endobronchial intubation. Anesth Pain Med 6: e33640.
- Maciejewski D (2012) Sufentanil in anaesthesiology and intensive therapy. Anaesthesiol Intensive Ther 44: 35-41.
- Kay B, Nolan D, Mayall R, et al. (1987) The effect of sufentanil on the cardiovascular responses to tracheal intubation. Anaesthesia 42: 382-386.
- Minto CF, Schnider TW, Shafer SL (1997) Pharmacokinetics and pharmacodynamics of remifentanil. ii. model application. Anesthesiology 86: 24-33.
- Maruyama K, Nishikawa Y, Nakagawa H, et al. (2010) Can intravenous atropine prevent bradycardia and hypotension during induction of total intravenous anesthesia with propofol and remifentanil?. J Anesth 24: 293-296.
- Hayashi K, Tanaka A (2016) Effect-site concentrations of remifentanil causing bradycardia in hypnotic and non-hypnotic patients. J Clin Monit Comput 30: 919-924.
- Liao X, Yang QY, Xue FS, et al. (2009) Bolus dose remifentanil and sufentanil blunting cardiovascular intubation responses in children: A randomized, double-blind comparison. Eur J Anaesthesiol 26: 73-80.
- Deepika K, Kenaan CA, Bikhazi GB, et al. (1999) Influence of the priming technique on pharmacodynamics and intubating conditions of cisatracurium. J ClinAnesth 11: 572-575.
- Kim KM, Choi BM, Park SW, et al. (2007) Pharmacokinetics and pharmacodynamics of propofolmicroemulsion and lipid emulsion after an intravenous bolus and variable rate infusion. Anesthesiology 106: 924-934.
- Rüsch D, Arndt C, Eberhart L, et al. (2018) Bispectral index to guide induction of anesthesia: A randomized controlled study. BMC Anesthesiol 18: 66.
- Muzi M, Berens RA, Kampine JP, et al. (1992) Venodilation contributes to propofol-mediated hypotension in humans. Anesth Analg 74: 877-883.
- Shah NK, Harris M, Govindugari K, et al. (2011) Effect of propofol titration v/s bolus during induction of anesthesia on hemodynamics and bispectral index. Middle East J Anaesthesiol 21: 275-281.
- Lysakowski C, Dumont L, Pellegrini M, et al. (2001) Effects of fentanyl, alfentanil, remifentanil and sufentanil on loss of consciousness and bispectral index during propofol induction of anaesthesia. Br J Anaesth 86: 523-527.
- Salmasi V, Maheshwari K, Yang D, et al. (2017) Relationship between intraoperative hypotension, defined by either reduction from baseline or absolute thresholds, and acute kidney and myocardial injury after noncardiac surgery: A retrospective cohort analysis. Anesthesiology 126: 47-65.
- Barclay K, Kluger MT (2000) Effect of bolus dose of remifentanil on haemodynamic response to tracheal intubation. Anaesth Intensive Care 28: 403-407.
- Bouillon TW, Bruhn J, Radulescu L, et al. (2004) Pharmacodynamic interaction between propofol and remifentanil regarding hypnosis, tolerance of laryngoscopy, bispectral index, and electroencephalographic approximate entropy. Anesthesiology 100: 1353-1372.
Corresponding Author
Yi Zou and Gaoyin Kong, Department of Anesthesioloy, Hunan Provincial People's Hospital, The First Affiliated Hospital of Hunan Normal University, Clinical Research Center for Anesthesiology of ERAS in Hunan Province, No.61, Jiefang West Road, Changsha City, Hunan Province, China
Copyright
© 2021 Huang Q, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.