Difficult Direct Laryngoscopy Followed by Easy Video Laryngoscopic Intubation in a Patient with Bilateral Mandibular Tori: Should the Patient be Labeled as Having a "Difficult Airway?"
Abstract
Mandibular tori are intraoral bony prominences which can make direct laryngoscopic intubation difficult. We present a case where we were unable to intubate a patient with bilateral mandibular tori using direct laryngoscopy, but then succeeded using video laryngoscopy. A post-procedure retrospective chart review found previous anesthetics where the patient had also been successfully intubated using video laryngoscopy but the patient was not informed verbally or with a letter that he was difficult to intubate. We informed the patient that he was a difficult direct laryngoscopic intubation and that appropriate equipment (e.g. video laryngoscope) should be available if the need arises to secure his airway in the future. With the increasing availability of video laryngoscopy, anesthesia providers should consider the circumstances under which a patient is informed that they are difficult to intubate.
Keywords
Difficult intubation, Difficult airway, Video laryngoscopy, Mandibular tori
Introduction
Mandibular tori are common intraoral bony prominences that have previously been reported as increasing difficulty in the performance of direct laryngoscopic intubation [1,2]. A simple inspection under the tongue during a basic airway exam could alert anesthesia providers of the possibility of potential difficulties. We present a case where the patient had multiple anesthetics and the airway was secured with the use of Video Laryngoscopy (VL), but the patient was not informed that he has "a difficult airway".
The patient has provided written consent to report this case.
Case Description
A 70-year-old male presented for a Computer Tomography (CT) guided microwave ablation of a metastatic right colon carcinoma involving the liver. Significant comorbidities included obstructive sleep apnea, hypertension, noninsulin dependent diabetes mellitus and obesity (BMI 30.13 kg/m2; 191 cm, 110 kg).
Since our institution had recently transitioned to a new electronic health record system (EPIC Software), the only previous anesthetic record available for immediate review was from four months prior to the current case. That record contained details of a colonoscopy performed under TIVA (Total Intravenous Anesthetic), with spontaneous, unsupported ventilation.
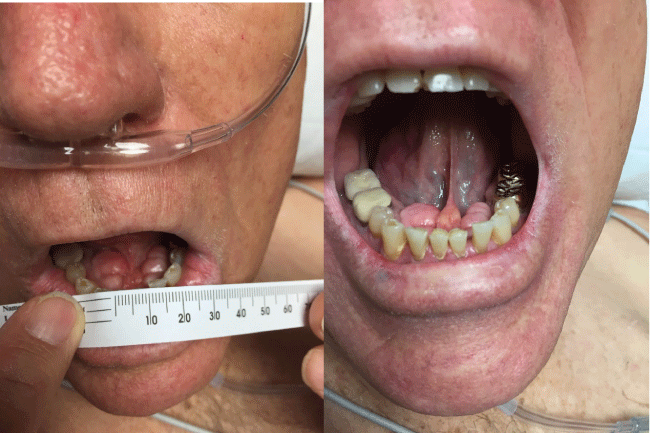
General anesthesia was planned for the current procedure using direct laryngoscopy to secure the airway. A C-MAC (C-MAC®, Karl Storz Video Laryngoscope) was available in the room. Our airway exam found adequate mouth opening, visualization of part of the uvula and entire soft palate (Mallampati Airway Class II) (Figure 1), slightly limited atlanto-occipital extension, > 3 fingerbreadths thyromental distance, and a neck circumference of 44 cm. The patient was placed in standard sniffing position (neck flexion, head extension) and induced with 50 micrograms of fentanyl, 4 mL of 2% lidocaine and 200 mg of propofol. Following confirmation of easy mask ventilation, 70 mg of rocuronium was administered. After 3 minutes, the CRNA (certified registered nurse anesthetist) performed direct laryngoscopy with a Macintosh #4 blade and obtained a Cormack-Lehane (CL) Grade 4 view, (CL Grade 3 view with a Backward, Upward, Rightward Pressure (BURP) maneuver). The supervising physician anesthesiologist (25 years of experience) improved the neck position by enhancing flexion and achieved a CL Grade 3 view with a Miller #2 blade. Upon further inspection below the tongue, bilateral mandibular tori were identified (Figure 2).
The Miller blade was then removed and a CL Grade 1 view was achieved by the CRNA with a C-MAC #3 blade, however she was unable to pass the Endo Tracheal Tube (ETT). The supervising anesthesiologist then used a regular sized Airtraq video laryngoscope (Airtraq, Prodol Meditec) and successfully passed a 7.5 mm ETT over a bougie under visualization through the Airtraq. Bilateral breath sounds were equal, and end tidal CO2 was confirmed. Throughout airway management, the patient was easily bag mask ventilated and the lowest recorded pulse oximetry saturation was 98%. The patient was extubated at the end of the 4 hour procedure without sequelae. The event was fully disclosed and an Anesthesia Patient Safety Foundation (APFS) "difficult airway letter" was given to the patient.
Post procedure, we were able to access the patient's anesthesia records from our previous electronic health record. The relevant details for those cases were as follows:
• 8 months prior, General Endo Tracheal Anesthesia (GETA) for left thoracotomy, 1st attempt successful with C-MAC #3 blade (CL Grade 1 view) VL.
• 11 months prior, TIVA for CT guided microwave ablation of the liver, two unsuccessful attempts with C-MAC #4 blade (CL Grade 3 view) VL, successful intubation with an Airtraq (CL Grade 1 view).
• 19 months prior, GETA for hepatic resection, one unsuccessful attempt with a Miller 2 blade by direct laryngoscopy ("no view"), successful intubation with an Airtraq (CL Grade 1 view).
• 20 months prior, TIVA for colonoscopy, with spontaneous unsupported ventilation.
Discussion
A preoperative dedicated airway physical exam should be conducted before all anesthetics [3]. Typically, a complete examination for prediction of difficult airway would include Mallampati (Samsoon Young modification) pharyngeal classification [4], incisor prominence, mandibular protrusion, inter-incisor gap and thyromental distance (cm) measured with the neck extended, sternomental distance, BMI, neck circumference (cm) measured at the level of the thyroid cartilage, dentition status, presence of facial hair, facial or neck trauma, nasal deficiencies, and neck mobility grade [5]. Airway exams for predicting difficult intubations often do not include inspection under the tongue.
Mandibular tori are exostoses found along the line of fusion of the palate or on the hemi-mandibular bodies that have both congenital and environmental etiologies [6,7]. The bony prominences may result in pain, food entrapment, poor oral hygiene and difficulty in the fitting of dentures [7]. They are relatively common with a prevalence reported from 12.3% to 26.9%, and not restricted to specific ethnic populations [6,7].
Elevation of the occiput and atlanto-occipital joint extension ("sniffing position") allows alignment of the mouth and pharynx while the laryngoscope aligns the tracheo-laryngeal axis with the line of vision facilitating intubation [8]. While the patient's increased BMI and large neck circumference may also have contributed to difficulty with direct laryngoscopy, we surmised that the presence of an immobile mass in the sublingual space and some obstruction to sweeping the tongue to left [1], made it difficult to align these axes. Preoperatively, a simple tongue to roof of mouth exam would have revealed the tori.
In our scenario, a retrospective review of anesthetic records indicated that the patient had been previously intubated on different occasions using a C-MAC and Airtraq (the superiority of an Airtraq over C-MAC in the case of mandibular tori may be explained by the shape of the Airtraq [9]). He was not given any letters identifying him as a difficult direct laryngoscopic intubation. We also had a CL Grade I view with two different video laryngoscopes (C-Mac and Airtraq) but successful intubation only with the Airtraq. The decision was made to inform the patient of our difficulties; that he was a difficult direct laryngoscopy and appropriate advanced airway equipment is available for subsequent anesthetics in which his airway must be secured.
This case illustrates a dilemma regarding routine VL use: when do we conclude that a patient is a difficult intubation and provide them with the appropriate documentation to inform future anesthesia providers? Even before the popularity of VL, there was no consensus on the term "difficult intubation", although difficult laryngoscopy would usually be present as part of the definition [3]. With VL often becoming the first line technique on suspicion that a patient may be difficult to intubate [10], there is the potential for false positive documentation of a difficult intubation if it is that facility's decision to apply that label every time a technique other than direct laryngoscopy is used (many electronic anesthetic charting programs may automatically link VL to the designation of difficult intubation). The corollary situation may also occur: a patient may report that they did not have a history of difficult intubation because only VL was successfully used, but would have proved difficult had direct laryngoscopy been attempted (false negative). This last scenario would be particularly problematic in environments where VL is not so readily available, such as the floors or anywhere outside main operating rooms where direct laryngoscopes may be the only tools available.
One advantage of video laryngoscopes with standard size blades (e.g. C-MAC) then, is that they afford the ability to visualize the glottis directly and obtain a CL laryngoscopy grade. Thus, two laryngoscopic grades could be listed in the anesthetic record (direct and indirect).
In our case, we labelled the patient a difficult intubation and provided him with a letter because we had documentation of difficult laryngoscopy with the standard technique. Our institution currently does not have guidelines to determine when to label a patient a difficult intubation and therefore the designation is left up to the individual practitioner. We suggest that institutions develop such a protocol and that letters to the patient be as specific as possible when describing the details of the intubation, including whenever possible, the laryngoscopic view from standard direct laryngoscopy.
Conflicts of Interest
None.
Written informed consent for the publication of this case report was obtained from the patient.
References
- Durrani MA, Barwise JA (2000) Difficult endotracheal intubation associated with torus mandibularis. Anesth Analg 90: 757-759.
- Woods GM (1995) Mandibular tori as a cause of inability to visualize the larynx. Anesth Analg 81: 870-871.
- Apfelbaum JL, Hagberg CA, Caplan RA, et al. (2013) Practice guidelines for management of the difficult airway: an updated report by the American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Anesthesiology 118: 251-270.
- Samsoon GL, Young JR (1987) Difficult tracheal intubation: a retrospective study. Anaesthesia 42: 487-490.
- Cattano D, Katsiampoura A, Corso RM, et al. (2014) Predictive factors for difficult mask ventilation in the obese surgical population. F1000Res 3: 239.
- Garcia-Garcia AS, Martinez-Gonzalez JM, Gomez-Font R, et al. (2010) Current status of the torus palatinus and torus mandibularis. Med Oral Patol Oral Cir Bucal 15: e353-e360.
- Sarma J (2014) Unexpected Difficult Intubation in a Patient with Prominent Mandibular Tori. The Open Anesthesiology Journal 8: 1-3.
- Berry JM, Harvey S (2013) Laryngoscopic Orotracheal and Nasotracheal Intubation: Preparation and Positioning. In: Hagberg CA, Benumof and Hagberg's Airway Management. (3rd edn), Elsevier Saunders, Philadelphia, 347-348.
- Yoshida H, Sawada M, Takada N, et al. (2011) Rigid Videolaryngoscope for difficult intubation caused by mandibular tori. J Anesth 25: 473-474.
- Paolini JB, Donati F, Drolet P (2013) Review article: Video-laryngoscopy: another tool for difficult intubation or a new paradigm in airway management? Canadian Journal of Anesthesia 60: 184-191.
Corresponding Author
Jens Tan, MD, Assistant Professor, Department of Anesthesiology and Perioperative Medicine, The University of Texas MD Anderson Cancer Center, 1400 Holcombe Blvd, Unit 409, Houston, TX 77030, Texas, USA, Tel: 713-792-6911.
Copyright
© 2017 Tan J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.