The Preliminary Impact of Pain Management Integration into an HIV Specialty Clinic
Abstract
Objective
A significant number of HIV (human immunodeficiency virus) infected patients suffer from chronic pain where providers often lack access to specialty pain management services. Emerging evidence about risks of chronic opioid use has resulted in closer scrutiny of long-term opioid therapy. While some health systems are beginning to employ blanket restrictions on opioid use, others attempt to preserve individualized care by investigating cost-effective ways to extend pain management services to underserved areas. The purpose of this review was to determine the impact of a Clinical Pharmacy Specialist in pain management, collaborating with a subspecialty HIV practice over a ten month period.
Methods
A retrospective medical chart review was undertaken for all HIV positive veterans receiving opioid prescriptions through the Stratton VA Medical Center (SVAMC) HIV clinic from August 2013 to May 2014.
Results
A total of 86 patient records were reviewed. Twenty (23.3%) patients were on opioids at baseline, and during the course of the study, 13 (65%) patients either had their opioids discontinued (7 patients, 35%) or reduced (6 patients, 30%). Among those whose opioids were reduced, the mean percent reduction in opioids was 32% measured as overall reduction from baseline.
Conclusion
The integration of pharmacy pain management services into a subspecialty HIV clinic had a profound impact on patient care and provider morale. Dedicating the equivalent of one day per week, this collaborative model proved to be cost-effective while improving management in a high risk area and delivering specialty services that could improve outcomes, mitigate risk, and reduce burden to providers.
Keywords
Opioids, Pain management, Human Immunodeficiency Virus (HIV)
Background
Human immunodeficiency virus (HIV) affects approximately 35 million people worldwide. The number of people estimated to live with HIV and suffer from chronic pain is reported to be 40%-60% which may be conservative given the large variation between sources [1-5]. This can be attributed to HIV disease and iatrogenic antiretroviral neuropathic pain syndromes in addition to common chronic musculoskeletal and neuropathic pain etiologies [6]. The treatment approach to pain management in the HIV setting was originally, by necessity, a palliative approach focusing on the relief of suffering and symptom management for a terminal illness [7]. With the advent and widespread use of potent anti-retroviral therapy, deaths are now considered a tragedy often resulting from late diagnosis or lack of adherence with less than 50% of deaths attributable to disease progression [8,9]. Increased longevity raises treatment complexity for a number of reasons including high comorbid disease burden, substance abuse disorders, and psychiatric diagnoses associated with HIV which must transition to chronic disease management [7,10-12].
Chronic pain management remains a challenging area for many health care providers and it may be a particularly arduous task for those treating an HIV population. Barriers to pain management services for HIV infected individuals include: lack of training, appointment time constraints, reluctance to prescribe opioids, potential drug-drug, drug-disease, drug-food interactions, pharmacogenetic variability, lack of access to pain specialists with expertise in advanced pharmacotherapeutics, concerns about drug addiction, substance abuse, lack of psychological support, and drug treatment services [13]. Utilizing a chronic pain approach in the HIV population has many advantages including comprehensive assessment, risk stratification, UDS monitoring, patient education, maximizing adjunct medications or therapies, and incorporation or referral to specialty services as appropriate.
Formerly there was a focus on the "inadequate" treatment of pain and underutilization of pain medications [14-17]. However, over the last few years there has been a comprehensive paradigm shift criticizing pain as the "fifth vital sign" and emphasizing new initiatives to reduce chronic opioid prescribing [18]. In large part this is due to an upsurge in regulatory policies, increased mortality and morbidity associated with prescription abuse and misuse, and political influences [19-21]. Increased scrutiny surrounding opioid utilization in the chronic pain population has prompted health systems to explore strategies to reduce opioid utilization. This often takes the form of blanket restrictions on opioid prescribing with maximum daily limits set in terms of morphine equivalent daily dose (MEDD) for each patient regardless of pain history or pathology [18,22]. Alternatively, to preserve individualized care, some health systems, including our own facility, are exploring strategies that attempt to cost-effectively integrate pain specialty services to improve outcomes.
The Stratton VA Medical Center in Albany, NY was fortunate to have initiated a collaboration with the clinical pharmacy pain management service and select specialty care in 2013. The Infectious Diseases Section and Pain Management Service began concurrent chronic pain management evaluations in August 2013 and this process has continued to the present day. A quality assurance review was initiated and the preliminary results of this collaboration are reported herein. All providers play an integral role in patient care. Each patient is seen first by the physician and subsequently by a postgraduate year 2 (PGY2) pain & palliative care (PPC) Pharmacy Pain Resident upon request to develop a "pain care plan". In all cases, interventions by the resident are supervised by the PGY2 Pharmacy Pain Management Residency Director consistent with current policy and acceptable standards of practice. The pharmacy pain resident's mandate was to apply evidenced-based principles from chronic pain guidelines to specialized care [23-25]. Specific interventions included: pain assessment, pain pathology (i.e. musculoskeletal or neuropathic), appropriateness of medication therapy, screening for aberrant behaviors (i.e. early fills, over/under dosing, lost/stolen prescriptions, abnormal or unexpected urine drug screens, and non-adherence with treatment plan), patient education, and phone follow-up to address medication related questions and assess severity of reported side effects. Drug-drug interactions are reviewed, the possibility of pharmacogenetic influences are evaluated, and alternative or additional modalities are discussed.
The purpose of this review was to determine the preliminary impact of a Pharmacy Pain Resident in collaboration with a Clinical Pharmacy Pain Specialist on a subspecialty HIV practice.
Study Design and Methodology
A retrospective medical chart review of all veterans treated by the Infectious Diseases specialists at the Stratton VA's outpatient HIV clinic was undertaken from August 2013 to May 2014. The Pharmacy Pain Resident dedicated two half day sessions of HIV outpatient clinical care per week over the study period. The main outcome of interest for our review was the percent change in opioid use with the involvement of the pain service as outlined above. Additional outcomes of interest included utilization of adjuvant medications appropriate for mechanism of pain complaint, comorbid mental health diagnoses, comorbid substance abuse, appointment attendance as an indicator of treatment adherence, and monitoring parameters (pain agreement, UDS). The project format was submitted to the Stratton VA Medical Center Institutional Review Board (IRB) and it was determined not to be research and exempt from IRB review, as validated by exclusion under 45 CFR 46.101(b).
Utilizing the VA's electronic computerized patient record system (CPRS), patient information was systematically reviewed and evaluated for inclusion utilizing information from clinic notes (physician, pharmacist, and nursing), medication refill history, and lab results. Baseline characteristics were recorded such as age, gender, history of substance abuse, mental health history, pain agreements, urine drug screen (UDS) frequency, and clinic appointment adherence.
For our main outcome of interest, opioid use was evaluated at baseline by collecting drug name, duration, amount, and source and comparing it to levels at the end of the study. Patients were excluded from the analysis if: (1) patients were not seen in clinic during the study period or (2) opioid prescriptions were managed by non-HIV providers.
Results
A total of 96 veterans were assessed for inclusion, however, 6 veterans were excluded because they were not seen during the study period and an additional 4 veterans were excluded because their opioid prescriptions were managed by non-HIV providers. For the 86 veterans that were included, 80 (93%) were male and 6 (7%) were female. The mean age was 59 (29-82) years old. Thirty (34.8%) patients were seen by the Pharmacy Pain Resident at the request of HIV providers at least once, and 22 (25.6%) were managed with opioids at some point.
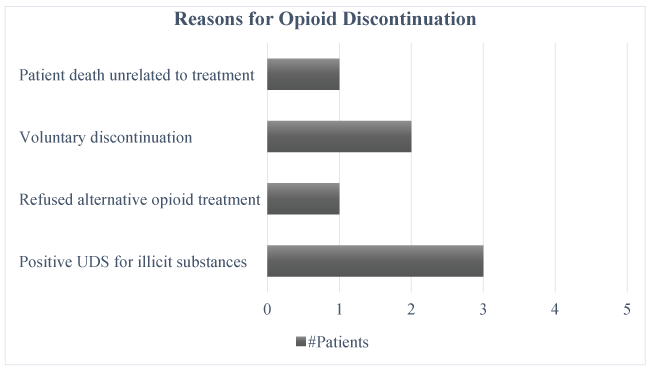
An important outcome of interest was to assess the percent change in opioid utilization after pain specialist involvement. We found 20 (23.3%) patients were on opioids at baseline, and during the course of the study, 13 (65%) patients either had their opioids discontinued (7 patients, 35%) or reduced (6 patients, 30%). In patients whose opioids were reduced, the mean percent reduction in opioids was 32% which was measured as absolute reductions and not morphine equivalent daily dose (MEDD) since none of these patients were rotated to alternative opioids. Reasons for opioid discontinuation are listed in Figure 1. The remaining two patients offered opioid therapy had a recent and serious history of substance abuse but with significant pain pathology. At the medical provider's request, a specialized pain management plan for each patient was instituted including weekly follow-ups, urine drug screens, required appointment adherence, education about non-pharmacologic treatment options, adjunct pain medications, and a week's supply of opioids in a dosage form more difficult to abuse compared to their previous regimen. Unfortunately, neither patient could demonstrate adherence for more than a week and were subsequently discontinued from opioid therapy altogether and offered adjuvant and non-pharmacologic modalities. An additional eight patients were seen by the Pharmacy Pain Resident and four were evaluated but not considered candidates for opioid therapy due to untreated neuropathies, two were treated for inflammatory conditions, and two were general pharmacy questions unrelated to pain (drug interactions, crushable dosage forms).
For the additional outcomes of interest, adjuvant medications, 10 (45.5%) patients on opioids were also taking anti-inflammatories compared to 20 (23.3%) patients in our overall study population. Similarly, 9 (40.9%) patients on opioids were also treated with an adjuvant agent such as an anticonvulsant (gabapentinoids) or antidepressants with noradrenergic reuptake inhibitory properties [serotonin norepinephrine reuptake inhibitors (SNRI), tricyclic antidepressants (TCA)] for neuropathy compared to 17 (19.8%) in the overall study group. Comorbid mental health diagnoses were noted among 9 (41%) patients on opioid therapy, with depression (31.8%) and post-traumatic stress disorder (18.2%) being the most common. A history of substance abuse was also seen in 18 (68.2%) patients on opioids but whether this was recent or distant was not determined. Interestingly, adherence with scheduled appointments turned out to be an excellent predictor of treatment adherence. Patients on opioids were scheduled in clinic more frequently and 73% more likely to keep appointments possibly because it was a requirement to receive their prescriptions. However, compared to similar patients on opioids, patients that would eventually be discontinued from opioid therapy were 2.5 times more likely to "no-show", cancel, or present for unscheduled clinic visits. For monitoring parameters, at the end of the study only 5 (22.7%) patients on opioids had signed an opioid agreement. However, UDS were frequently ordered for opioid patients with 16 (72.3%) patients providing UDS in the prior 6 months, and 20 (90.9%) patients within the previous 12 months.
Discussion
Infectious disease providers often function as primary care physicians for HIV-infected patients either by health-system directive or patient preference. While this likely provides considerable advantage with respect to care continuity in effectively treating their HIV, it also places enormous pressure on these specialty physicians to treat a number of conditions outside their area of expertise. Pain management is an area where patients can easily monopolize a significant amount of the medical providers' time attempting to address persistent complaints or requests for opioid medications [26,27]. Continuous complaints about not receiving a patient-preferred opioid, communications with emergency department personnel, addressing complaints to the patient advocate or requests for early opioid renewals, interpreting false negative/positive urine screens, and other time consuming interruptions undoubtedly have a negative impact on other patient care obligations [28]. Therefore, treating pain effectively often requires an artful interdisciplinary team approach with skilled clinicians that are excited and passionate about pain management and the compulsory challenges that are inherent to the specialty.
Open collaboration between infectious disease providers and our pain management service was a tremendous success prompting a retrospective quality assurance review to quantify this benefit. Incorporating this pain service resulted in a significant reduction in opioid utilization with only one-third of patients prescribed opioids remaining unchanged from baseline. The pain specialists mandate was not a reduction in opioid use but instead focused on providing evidence and guideline-based recommendations into practice with routine assessments for pain type, aberrant behavior, progress towards treatment goals, and appropriateness of therapy. Opioids were tapered, without patient consent in the absence of identifiable pathology or if aberrant behaviors were present. In all cases, pain management with adjunct non-opioid medication was offered and education provided. Utilizing a pharmacy pain specialist in this capacity proved advantageous due to the complexity of drug interactions, not the least of which included complicated HIV medication regimens.
This collaboration also yielded unanticipated benefits in decreasing provider burden and preserving patient-provider relationship. Patients were seen by the Pharmacy Pain Resident in separate but connected visits to the provider allowing for discussion between providers and warm patient handoff. Developing a pain management program within an existing clinic not only improved patient adherence with medical follow-up but decreased the time liability providers would otherwise devote to address concerns related specifically to pain management. Also, because the pain specialist was responsible for monitoring and follow-up, patients with repeated aberrant behavior, testing positive for illicit drugs, or other violations of their opioid agreement resulting in discontinuation of opioid therapy could openly discuss their concerns or displeasure at the pain resident, which allowed the HIV provider to continue offering treatment for HIV. In addition to the measurable results previously stated, the HIV providers were immensely satisfied at having consistent and dedicated pain management access in the specialty clinic. Examples mentioned by our clinical providers included the following: "Sometimes I'm uncomfortable prescribing pain medications because it's difficult to delineate if pain is real or not and I don't want to deny giving pain medications to someone with real pain, but at least with pain management there I feel as if I have the expertise to guide me; I couldn't do this without them; Having the pain management service in our clinic provides the best point of care for our patients, we're able to directly discuss potential issues and provide solutions with the support we need for this sometimes difficult area of medicine."
Numerous studies have shown correlations between mental health diagnoses and chronic pain patients and our review was no different. Forty one percent of patients on opioids also had a mental health diagnosis. Depression was the commonest among mental health diagnoses and appeared to be present in nearly one-third of all patients prescribed opioids. Post traumatic stress disorder was also frequent and was present in nearly one-fifth of all patients on opioids but this may not be generalizable because the incidence of PTSD is much more common among the veteran population compared to the general public. A history of substance abuse was noted in nearly two-thirds of patients on opioids but how recently the drug abuse occurred was not assessed. The difference in utilization of adjunct medications between baseline and the end of our study was not evaluated, however, by the end of the study patients on opioids were twice as likely to be on adjunct medications for pain particularly anti-inflammatories or anti-convulsants/antidepressants indicating attempts to address each patient's pain pathology.
Putting our clinic under the microscope for the study period also highlighted areas for improvement. First, it was noted that only one-fifth of patients on opioids had signed an opioid agreement. We suggest that this be a requirement for each patient so that he/she understands both the risks and benefits of opioid therapy and also expectations. Second, risk stratification tools were not utilized. This method prospectively could in fact help identify higher risk individuals earlier in treatment and thus mitigate against certain hazards such as unrecognized mental problems or active addiction.
Our study has several limitations including the lack of a control group, and small sample size of patients resulting in inadequate power to make comparisons or evaluate for significance between groups. Additional limitations included a higher average age and predominantly male patients, hence limiting external validity to a more diverse population.
Conclusion
Rather than blanket restrictions in opioid use that threaten individualized care, health systems should consider focusing on cost-effective delivery of specialty services to high need areas like HIV clinics. The most impressive feature of this experience is the profound effect that involving a pain resident with training in pharmacotherapeutics demonstrated despite involvement for the equivalent of one day per week. Innovative health systems could potentially offer specialty pain management services economically in four to five different specialty areas each week and perhaps expect similar outcomes and improvements in opioid utilization and provider morale. While small, our study demonstrates that opioid utilization can be addressed while effectively treating a patient's pain complaints on an individualized basis and for the appropriate pain mechanism.
References
- Gaither JR, Goulet JL, Becker WC, et al. (2014) Guideline-Concordant Management of Opioid Therapy Among Human Immunodeficiency Virus (HIV)-Infected and Uninfected Veterans. J Pain 15: 1130-1140.
- Merlin JS, Cen L, Praestgaard A, et al. (2012) Pain and Physical and Psychological Symptoms in Ambulatory HIV Patients in the Current Treatment Era. J Pain Symptom Manage 43: 638-645.
- Merlin JS, Westfall AO, Raper JL, et al. (2012) Pain, Mood, and Substance Abuse in HIV: Implications for Clinic Visit Utilization, Antiretroviral Therapy Adherence, and Virologic Failure. J Acquir Immune Defic Syndr 61: 164-170.
- Krashin DL, Merrill JO, Trescot AM (2012) Opioids in the Management of HIV-Related Pain. Pain Physician 15: ES157-ES168.
- Namisango E, Harding R, Atuhaire L, et al. (2012) Pain Among Ambulatory HIV/AIDS Patients: Multicenter Study of Prevalence, Intensity, Associated Factors, and Effect. J Pain 13: 704-713.
- Frich LM, Borgbjerg FM (2000) Pain and Pain Treatment in AIDS Patients: A Longitudinal Study. J Pain Symptom Manage 19: 339-347.
- Merlin JS, Tucker RO, Saag MS, et al. (2013) The Role of Palliative Care in the Current HIV Treatment Era in Developed Countries. Top Antivir Med 21: 20-26.
- Selwyn PA, Arnold R (1998) From fate to tragedy: the changing meanings of life, death, and AIDS. Ann Intern Med 129: 899-902.
- Antiretroviral Therapy Cohort Collaboration (2010) Causes of death in HIV-1–infected patients treated with antiretroviral therapy, 1996-2006: collaborative analysis of 13 HIV cohort studies. Clin Infect Dis 50: 1387-1396.
- Galvan FH, Burnam MA, Bing EG (2003) Co-occurring psychiatric symptoms and drug dependence or heavy drinking among HIV-positive people. J Psychoactive Drugs 35: 153-160.
- Pence BW, Miller WC, Whetten K, et al. (2006) Prevalence of DSM-IV–defined mood, anxiety, and substance use disorders in an HIV clinic in the Southeastern United States. J Acquir Immune Defic Syndr 42: 298-306.
- Gaynes BN, Pence BW, Eron JJ Jr, et al. (2008) Prevalence and comorbidity of psychiatric diagnoses based on reference standard in an HIV+ patient population. Psychosom Med 70: 505-511.
- Swica Y, Breitbart W (2002) Treating Pain in Patients with AIDS and a History of Substance Use. West J Med 176: 33-39.
- Breitbart W, Kaim M, Rosenfeld B (1999) Clinicians' Perceptions of Barriers to Pain Management in AIDS. J Pain Symptom Manage 18: 203-212.
- Stephenson J (1996) Experts Say AIDS Pain Dramatically Undertreated. JAMA 276: 1369-1370.
- Breitbart W, Rosenfeld BD, Passik SD, et al. (1996) The Undertreatment of Pain in Ambulatory AIDS Patients. Pain 65: 243-249.
- Breitbart W, Passik S, McDonald MV, et al. (1998) Patient-Related Barriers To Pain Management In Ambulatory AIDS Patients. Pain 76: 9-16.
- Atkinson TJ, Schatman ME, Fudin J (2014) The damage done by the war on opioids: the pendulum has swung too far. J Pain Res 7: 265-268.
- Balantyne JC (2012) "Safe and effective when used as directed": the case of chronic use of opioid analgesics. J Med Toxicol 8: 417-423.
- American Academy of Pain Medicine (2013) Use of Opioids for the Treatment of Chronic Pain.
- Volkow ND, Frieden TR, Hyde PS, et al. (2014) Medication-Assisted Therapies-Tackling the Opioid-Overdose Epidemic. New Eng J Med 370: 2063-2066.
- FDA (2014) FDA Response to Citizens Petition: Physicians for Responsible Opioid Prescribing (PROP). Docket ID FDA-2012-P-0818.
- Chou R, Fanciullo G, Fine P, et al. (2009) Clinical Guidelines for the Use of Chronic Opioid Therapy in Chronic Noncancer Pain. J Pain 10: 113-130.
- VA/DoD (2010) Clinical Practice Guideline For Management of Opioid Therapy For Chronic Pain.
- Manchikanti L, Abdi S, Atluri S, et al. (2012) American Society of Interventional Pain Physicians (ASIPP) Guidelines for Responsible Opioid Prescribing in Chronic Non-Cancer Pain: Part 2-Guidance. Pain Physician 15: S67-S116.
- Wasan AD, Wootton J, Jamison RN (2005) Dealing with difficult patients in your pain practice. Reg Anesth Pain Med 30: 184-192.
- Bruns D, Disorbio JM, Hanks R (2007) Chronic Pain and Violent Ideation: Testing a Model of Patient Violence. Pain Med 8: 207-215.
- Matthias MS, Parpart AL, Nyland KA, et al. (2010) The Patient-Provider Relationship in Chronic Pain Care: Providers' Perspectives. Pain Med 11: 1688-1697.
Corresponding Author
Timothy J Atkinson, Pharm D, BCPS, Clinical Pharmacy Specialist, Pain Management, VA Tennessee Valley Healthcare System, Murfreesboro, Tennessee, USA.
Copyright
© 2017 Mahatme S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.