Enucleation of Pancreatic Insulinomas with the use of Intraoperative Ultrasonography
Abstract
Tumor-induced hypoglycaemia is very rare, usually caused by a pancreatic beta cell tumor (insulinoma). Symptoms caused by inappropriate insulin secretion usually occur during fasting periods, they can be neurogenic or neuroglycopenic. The diagnosis usually takes up to 2-years, this is biochemical with imaging support. The only curative treatment for an insulinoma is surgical resection (enucleation or partial pancreatectomy).
Objective: To show our experience in the diagnosis and treatment of insulinomas, mentioning diagnostic methods and location with Intraoperative Ultrasonography.
Method: A retrospective analysis of five patients treated at the Clinical Hospital of the University of Chile between 2006 and 2015 was performed.
Results: The average age was 49.2 years (SD 28). The average time between the onset of symptoms and diagnosis was 3.1 years. An imaging study was performed in all patients, with CT of the abdomen and pelvis, identifying a single tumor in all cases with an average size of 1.24 cm (SD 0.26 cm).
Conclusion: Insulinoma should be suspected for symptomatic hypoglycemia, especially in non-diabetic patients. The use of ultrasonography allows to precisely orient the dissection avoiding pancreatic complications and the presence of remnants that could recur. Intraoperative US allows successful enucleation, avoiding morbid resections.
Keywords
Insulinoma, Ultrasonography, Enucleation
Introduction
Tumor-induced hypoglycaemia is very rare, being caused in most cases by a pancreatic beta-cell tumor (insulinoma). Insulinoma are the most frequent functioning pancreatic neuroendocrine tumors (25%). However, their overall incidence is 4/million inhabitants/year [1]. They usually appear during the fifth decade of life, predominantly in females (60%). Most are single and benign (87%), but may be multiple in 7% of cases, and malignant in 6% of patients. It is very important to remember that they can occur in the context of hereditary pathologies such as MEN [2].
Symptoms caused by inappropriate insulin secretion occur most frequently during periods of fasting, and can appear at any time of the day. These can be neurogenic, such as hunger, diaphoresis, paresthesia, palpitations, sweating, anxiety and tumor [1,3] or neuroglycopenic, such as confusion, altered mental status, behavioral changes, seizures, confusion and coma [4]. A Clinical sign that should raise suspicion of insulinoma is weight gain as a result of frequent feeding to avoid symptoms of hypoglycaemia [1].
The aim of this study is to show our experience in diagnosis and treatment of insulinomas, mentioning diagnostic methods and localization with Intraoperative Ultrasonography (US IOp).
Material and Methods
A retrospective analysis of five patients treated at the Clinical Hospital, Universidad de Chile between 2006 and 2015 was performed (Table 1).
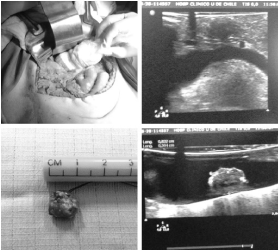
Surgical protocol: Bilateral subcostal laparotomy. Wide Kocher maneuver, exposure of the entire pancreas. Intraoperative ultrasonography to identify the lesion, location and relationship with the duct of Wirsung. Careful blunt dissection and hemostasis with ligatures. Enucleation. Real time ultrasonographic control. Ex situ control of the lesion to compare size and characteristics. US IOp review of pancreas for remaining lesions.
Results
Five patients were included, 4 females and 1 male, with a mean age of 49.2-years (SD 28-years).
The average time between the onset of symptoms and diagnosis was 3.1-years (SD 4.9 years). Among the symptoms, the most frequent was hypoglycaemia, occurring in 4/5 patients, two patients, 3/F and 5/H presented neuroglupenic symptoms, manifesting with an episode of lipotimia and confusional syndrome respectively (Table 2).
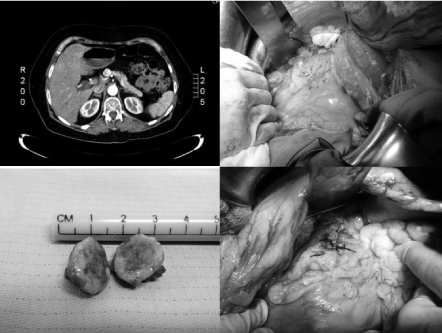
An imaging study was performed in all patients with CT of the abdomen and pelvis, a single tumor was identified, with an average of 1.24 ± 0.23 cm, 2 were located in the head of the pancreas, 2 in the neck and 1 in the uncinate process.
In all cases, laparotomy was performed with bilateral subcostal approach, performing enucleation with fine dissection under intraoperative ultrasonographic imaging (location and real-time control of Wirsung's duct). A single tumor was evidenced in all cases, with an average size of 1.3 cm (E.D. 0.35 cm). Partial pancreatectomy was not performed in any case. The average surgical time was 210 minutes (D.E. 53 minutes). Dextrose 10% infusion and serial hemoglucotest control were maintained during the operation. In all cases the rapid biopsy was reported as insulinoma (Figure 1).
Regarding complications, one patient (1/F) presented with a small intra-abdominal collection during the postoperative period, which did not require intervention (Table 3).
Discussion
Because of its rarity, the diagnosis of insulinoma usually takes up to 2-years from the onset of symptoms. In our case the average time from symptom onset to diagnosis was 3-years. In patients presenting Whipple's triad (symptoms of hypoglycaemia with decreased glycemia that reverts with glucose intake), a biochemical diagnosis of insulinoma can be made by confirming that there is hyperinsulinism associated with the episode according to the following criteria: fasting glycemia < 55 mg/dL, plasma insulin ≥ 3 mU/mL, plasma C-peptide ≥ 6 ng/mL, plasma proinsulin ≥ 5 pmol/L, b-hydroxybutyrate ≤ 2.7 mmol/L, glycemia change ≥ 25 mg/dL after 30 minutes of EV glucagon administration, negative blood sulfonylureas study and absence of circulating anti-insulin antibodies. If we only have a history of episodes with compatible symptomatology, without an associated diagnostic laboratory [1], a prolonged fasting study (72h fasting) can be performed according to the protocol used in our series of patients to make the diagnosis (Figure 2).
Once the biochemical diagnosis has been made, the presence of the tumor must be confirmed by imaging; ultrasonography, tomography or magnetic resonance imaging can be used as localization methods. However, a negative imaging study does not rule out the presence of the tumor. In these cases, endosonography or laparoscopic ultrasound may be an option to confirm its presence and determine its location [5]. In our series, CT of the abdomen and pelvis was performed and was diagnostic in all patients.
The only curative treatment for an insulinoma is surgical resection, performing enucleation of the tumor or partial pancreatectomy. In most centers, it is performed by laparotomy, but in some centers, it is also performed laparoscopically, reporting similar morbidity [1].
In cases where the patient refuses surgery or is not a good candidate for it, medical treatment with frequent carbohydrate intake associated with the use of diaxozide (200-600 mg/day POV) or somatostatin analogues can be left [1].
Insulinoma are rare tumors, which should be suspected in symptomatic hypoglycaemia, especially fasting hypoglycaemia in non-diabetic patients, but their Clinical presentation follows a certain classic pattern. For this same reason, it is important that the index of suspicion for this pathology is high when faced with a non-diabetic patient presenting with hypoglycaemia, especially if it is fasting.
The diagnosis is biochemical, complementad by findings of pancreatic radiological tumor, usually unique.
The only curative treatment for insulinoma is complete resection [6]. In this retrospective study, we used the laparotomy approach with ultrasonography support, which allows us to better guide the dissection without causing pancreatic complications and in order not to leave remnants that could recur. In addition, in patients with head, neck or uncinate process location, intraoperative US allows successful enucleation, avoiding extensive resections such as pancreaticoduodenectomy or Whipple's operation.
Authors Declaration
There are no conflicts of interest in this review on the part of any of the authors. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
References
- Iglesias P, Diez JJ (2014) Management of endocrine disease: A clinical update on tumor-induced hypoglycemia. Eur J Endocrinol Eur 170: R147-157.
- Service FJ, Mc Mahon MM, O'Brien PC, et al. (1991) Functioning insulinoma-incidence, recurrence, and long-term survival of patients: A 60-year study. Mayo Clin Proc 66: 711-719.
- Service FJ, Dale AJ, Elveback LR, et al. (1976) Insulinoma: Clinical and diagnostic features of 60 consecutiva cases. Mayo Clin Proc 51: 417-429.
- Dizon AM, Kowalyk S, Hoogwerf BJ (1999) Neuroglycopenic and other symptoms in patients with Insulinomas. Am J Med 106: 307-310.
- Noone TC, Hosey J, Firat Z, et al. (2005) Imaging and localization of islet-cell tumours of the pancreas on CT and MRI. Best Pract Res Clin Endocrinol Metab 19: 195-211.
- Lou I, Inabnet W (2020) Advances in the diagnosis and management of insulinoma. Advances in treatment and management in Surgical Endocrinology 199-206.
Corresponding Author
Patricio Cabané T, Head and Neck Surgery, Clinica Indisa, Av Santa Maria 1810, Providencia, Santiago de Chile, 7520440, Chile, Tel: +56993351805
Copyright
© 2022 Patricio CT. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.