Post-Operative Chloride Phosphate and Calcium Phosphate Ratios in Hyperparathyroidism Patients
Abstract
Background: To determine significance of longitudinal laboratory testing and their ratios after parathyroidectomy in patients with primary hyperparathyroidism (pHPT).
Methods: Patients referred for evaluation of pHPT. Patient data was collected prospectively preoperatively as well as one month and one year post op. Changes in data were analyzed. T tests were used to determine significance.
Results: Post op there were significant decreases in parathyroid hormone (PTH) and calcium when comparing to preoperative data, however no significant difference between one month and one year post op, p = .170 (PTH) and p = .315 (calcium) were noted. The average Ca: PO4 decreased post op from 3.73 to 2.65, p = .000. There was a significant increase to 2.74 at one year. Cl: PO4 decreased preop to postop, p = .000 and there was no difference when comparing one month and year postop values.
Conclusions: Our study highlights the value of using common lab values and their ratios to aid in post-operative follow up of a spectrum of patients with pHPT.
Key words
Primary hyperparathyroidism, Hyperchloremia, Borderline, Normocalcemia, Chloride Phosphate ratio, Calcium phosphate ratio
Introduction
Primary Hyperparathyroidism (pHPT) is a disease characterized by elevated parathyroid hormone (PTH) levels attributed to an increase in parathyroid cell number due to adenoma or hyperplasia, resulting in dysregulation of the body's calcium levels. Under normal circumstances the body's calcium receptors (CaSR) would sense the increase in calcium and begin to excrete calcium at the level of the glomerulusand decrease PTH release. When PTH release is dysfunctional, the pathophysiologic response is to activate osteoclasts via FGF23 signaling which increases bone remodeling and subsequently releasing calcium and phosphate, increasing calcium absorption in the digestive tract, and increasing calcium retention at the level of the nephron [1]. This leads to the characteristic symptoms commonly attributed to primary pHPT: kidney stones, fatigue, depression, weakness, confusion, general muscle aches, and eventually even osteoporosis.
Due to widespread calcium testing in recent decades, patients may present before the disease has progressed to the point of overt kidney stones or the most severe forms of bone breakdown seen with brown tumors, previously pathognomonic for the condition. Consequently, a new subgroup of patients has emerged with some of the classic symptoms, but with borderline elevated calcium and/or PTH values. This has been reported to have varying incidence from 20% up to 38.9% seen in our previous study [2]. Since these patients are more commonly seen in contemporary practice, they are included in this study. This population is important to identify because they typically benefit from parathyroidectomy and yet can present challenges in diagnosis by calcium and PTH levels. The long-term effects of untreated pHPT on bone strength and the negative cardiovascular implications such as vasculopathy, increased blood pressure, and increased vascular occlusive events [3] are also significant reasons to pursue work up of borderline pHPT patients.
In previous studies by Reeve, et al. [4], the chloride phosphate ratio (Cl: PO4) had been shown to be highly sensitive and specific (0.94 and 0.96 respectively) at a ratio value of 33 and above for the diagnosis of pHPT. It is believed that the significant phosphate loss at the level of the proximal collecting tubule and chloride re- absorption from PTH activation are the driving factors for significance of this relationship. Because of this connection between primary hyperparathyroidism and the Cl: PO4, the Cl: PO4 has now been tested on the normocalcemic pHPT variety. Mismar, et al. [5] reported a sensitivity of 0.724 and specificity of 0.763. In our previous study we examined patients with classic hyperparathyroidism, normocalcemic hyperparathyroidism, those with elevated calcium and normal PTH values (normohormonal pHPT), and controls.
We looked at Receiver Operator Curves to examine the Cl: PO4 performance and the area under the curve (AUC) was found to be 0.712, with a low sensitivity of 58.4% with a ratio cutoff of 332. We however did see rather promising results when looking at the calcium phosphate ratio (Ca: PO4), which has also been shown to predict primary hyperparathyroidism. Madeo, et al. [6] recently reported a sensitivity of 85.7% and specificity of 85.3% with a Ca: PO4 ratio cutoff of 2.55. We found an AUC of 0.813 and when using a cutoff of 2.55, the Ca: PO4 in our study served as a robust predictor, with a sensitivity of 95.6% [2].
The major aim of this present study is to determine if Cl: PO4 and Ca: PO4 ratios normalize in the short term (1 month) and long term (1-year) postoperatively. Although we have shown the two ratios can be sensitive in aiding with the borderline pHPT diagnosis preoperatively, demonstrating that these ratios normalize post op would further support their significance in clinical practice, patient management post operatively, timing of post op lab testing, and be a possible marker to surveil for biochemical recurrence.
Methods
All research was conducted at a tertiary care hospital. University of Arkansas for Medical Sciences (UAMS) institutional review board approval was obtained. (IRB #205694) A retrospective chart review of all patients over the age of 18 undergoing parathyroidectomy by a single surgeon at the UAMS from August 2013 to February 2018 with a prospective collection of post-operative laboratories were reviewed. We routinely collected total (normal range 8.5-10.5 mg/dL) and ionized calcium (1.28-1.33 mmol/dL), intact PTH (12-88 pg/mL), magnesium (1.5-2.5 mEq/L), phosphorus (2.5-4.5 mg/dL), creatinine (0.6-1.2 mg/dL), and 25 OH vitamin D (30-80 ng/mL) [7]. Localization of presumed adenoma was typically established using a combination of office ultrasound and 4D CT. Patients were then taken to the operating room for focused parathyroidectomy. Intraoperative PTH monitoring was utilized for confirmation of surgical cure, and if a 50% decrease of PTH into the normal range was not seen following removal of the gland of interest, the neck was explored. Patients were seen routinely around 1-month post op, and then again at the one-year post-operative anniversary for laboratory examination.
Patients with a known history of malignancy of any kind or hyperparathyroidism due to secondary or tertiary causes were excluded. Data collected and reviewed included patient demographics, preoperative diagnosis and imaging, pathology, and preoperative and post-operative labs as outlined above. Descriptive statistics were generated for the entire population prior to subset analysis. Statistical analysis was run on the entire population including variant subgroups using paired t-test to compare lab values pre and post operatively. Variants examined, aside from classic hyperparathyroidism (Ca > 10.5 mg/dL, PTH > 88 pg/mL), were defined as normohormonal (exhibiting elevated Ca, but PTH < 88 pg/mL), normo calcemic (elevated PTH, but Ca < 10.5 mg/dL), and finally those with what we referred to as borderline pHPT having combined high normal Ca and PTH values.
Results
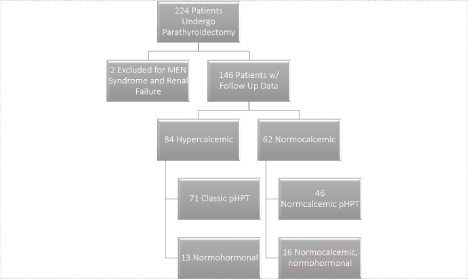
224 eligible patients underwent parathyroidectomy in the study period, 146 patients had complete preoperative and post op follow up data for analysis. The mean age was 64.9-years (SD = 12.85-years). 79.7% of patients were female (N = 118), and the remaining 20.3% were male. Figure 1 shows a breakdown, classified preoperatively based on calcium and PTH. 84 of the 146 patients (57.5%) had hypercalcemia (Ca > 10.5 mg/dL) preoperatively. Thirteen of those patients did not have a matched elevated PTH, defined as PTH greater than 88 pg/mL, making them part of the normo hormonal variant. The remaining 62 patients (42.5% of the population) were normo calcemic, 46 of those had elevated PTH classifying them as normo calcemic pHPT, and 16 of those had borderline elevated PTH levels.
Table 1 and Table 2 display the statistics generated preoperatively, at one month, and one year and the results of two tailed paired t tests for PTH, phosphorus, serum calcium, Ca:PO4, chloride, and Cl:PO4. As expected, the postoperative PTH significantly decreased from an average value of 144.03 pg/mL to 63.23 pg/mL which was a significant (p = 0.00). There was no significant difference between 1-month and 1-year post op PTH levels which averaged 63.23 pg/mL (p = 0.170).While there was an expected significant difference in preoperative (mean = 10.64 mg/dL) and postoperative calcium levels (mean = 9.33), p = 0.00, there was no significant difference in the 1-month and 1-year calcium levels (mean = 9.40 mg/dL), p = 0.315.
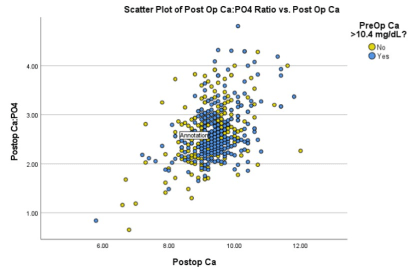
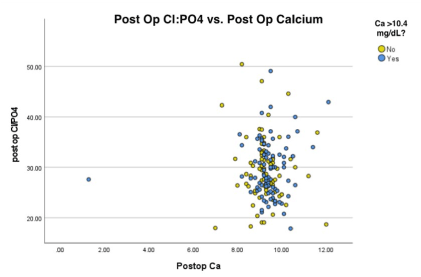
The mean preoperative phosphorus level for patients was 2.98 mg/dL, while the means at 1 month and 1 year postoperative were 3.67 mg/dL and 3.51 mg/dL, respectively. The postoperative one month and one-year values were both increased from the preoperative levels, p = .00. The difference in 1-month and 1-year phosphorous levels was also significant, p = 0.00, indicating an ongoing change of phosphorus over the first postoperative year. The average preoperative Ca: PO4 was 3.73 and the average 1-month post op was 2.65. At 1-year, there was an average Ca: PO4 of 2.78. There was a significant difference between preop and 1 month and 1 year post op, both p = 0.00, as well between the two post op ratios, p = 0.022. Figure 2 is a scatter plot of Ca: PO4 vs. postop Ca and values can be found between 2.00 and 3.00.
There was no significant difference in preop and post op chloride, p = 0.305. There was a significant difference in pre op and 1-year levels, p = 0.00 which reflects the slow decrease in chloride overtime. The average preoperative Cl: PO4 was 35.5, greater than 33 cut off. There was a significant decrease in the Cl: PO4 to 29.4 at 1 month follow-up, p = 0.00. The average Cl: PO4 remained below the cutoff of 33 at one year and there was no significant difference between one month and one-year ratios. The normalization of the ratio appears to be attributed, in part, to the increase in phosphorus levels postop, considering there was only a minor difference in the mean preoperative and postop chloride levels.
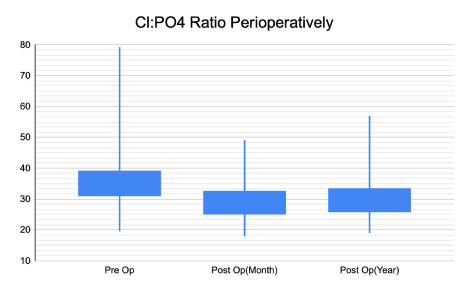
Figure 3 displays three adjacent whisker plots, and it can be observed that the rectangle, which represents the 50% of data between the first and third quartiles, is significantly lower, and importantly below the cutoff of 33 in the post op plots.
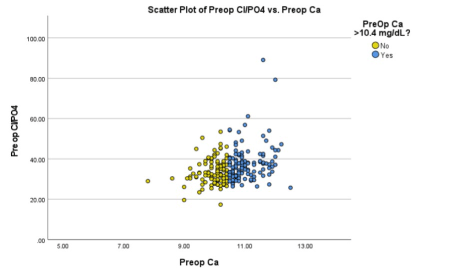
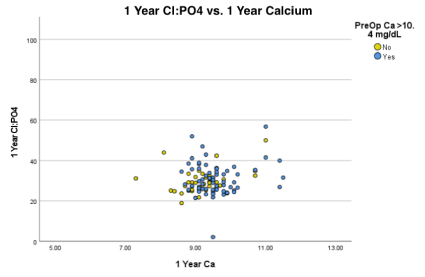
Figure 4 displays the preoperative Cl: PO4 versus calcium levels. Figure 5 displays 1-month post op Cl: PO4 values compared to calcium. The significant decrease in calcium and Cl: PO4 in those with classic pHPT can be observed between the two plots. It can also be observed that most patients were below the cutoff of 33 postop, and this was not unique between those with classical pHPT and variants. Figure 6 shows the same plots as in Figure 4 and Figure 5, but at the 1-year post op follow up. Although a few patients were lost to follow up, it can be observed that there does not appear to be a rightward shift of calcium, which might be appreciated if there were recurrences in patients. There also does not appear to be an upward shift representing an increase of Cl: PO4 at one year.
Discussion
Our previous 2 and current results show the value of using commonly available lab values to aid in the diagnosis and surveillance of patients with variants of primary hyperparathyroidism. There has been debate over how, and by whom (surgeon vs. other provider), to proceed with follow up and surveillance post parathyroidectomy. It is common for most surgeons to monitor patients in the immediate (up to 1 month) postoperative period because of the risk symptomatic hypocalcaemia which has been reported in up to 47% of patients but is infrequently permanent and generally treated with calcium +/- concurrent Vitamin D supplementation for a short interval [8]. Serious complications, such as hungry bone syndrome, can occur after parathyroidectomy. In this condition the patient can have rapid and profound hypocalcaemia, hyperphosphatemia, and hypomagnesaemia from a longstanding history of elevated pHPT and is thought to occur due to the rapid influx of calcium into the bone once excess PTH is no longer signaling osteoclasts to release it [9]. These issues are commonly left to the referring endocrinologists to manage.
With a reported recurrence rate as high as 14.8% at 10-years [10] and the insidious return of symptoms, there is clearly rationale for long term vigilance of post-operative pHPT. This task could be delegated to the primary care provider, but he or she will need education on this rationale. Current recommendations by the American Association of Endocrine Surgeons (AAES) and the American Association of Clinical Endocrinologists (AACE) calls for evaluation at 6months to ensure the patient is indeed still normocalcemic with normal PTH because persistent elevation in either calcium or PTH could signal an operative failure [11,12].
At our institution, patients were seen by the surgeon at 1-month post op, and then again around the one-year surgery anniversary. Our results highlighted how there was a significant decrease in PTH and serum calcium levels in the immediate postoperative period from pre op. Neither PTH nor calcium levels rebounded at one year. This leads to the question, how beneficial is continued surveillance after 1-month postoperative follow up for routine patients? In the immediate postoperative period, hypocalcaemia and rebound hyperphosphatemia can occur, but it appears that by the 1-year visit, the serum calcium and phosphorus were corrected within their normal ranges. It was interesting to note that phosphorus appeared to correct at 1-month, and then gradually decreased by one year.
In our previous study [2], the Cl: PO4 had a sensitivity of only 58.4%. Based on our results, we can see there was clearly a significant decrease in the Cl: PO4 postop, from a mean of 35.5 to a mean of 29.4. It is important to note that patients at 1-month post op Cl: PO4 ratios, 78.9% had normalized ratios. 10 of the normocalcemic variant patients (20.83%) and 13 (21.3%) with classic pHPT remained above the cutoff of 33. These ratios corrected over time and were not used as an indicator for intervention, they were observed.
While the Ca: PO4 had an excellent pre procedure sensitivity in our previous study (95.4%), and it significantly decreased post op, the average Ca: PO4 was 2.65 which remained above the 2.55 cutoff cited by previous literature. This highlights the nature of the ratio itself that, while it might be beneficial in preoperative evaluation, it is sensitive but not specific. We would also like to note the slight increase in the Ca: PO4 at one year. It was observed that while the calcium levels and Ca: PO4 remained decreased, the phosphorus did increase, which is reflected in the slightly increased Ca: PO4 at one year.
We do acknowledge that compared to our first study, which included over 200 patients undergoing parathyroidectomy for pHPT, we did have a smaller sample size due to attrition. In the first years of study data (2014-2015), patients were only tested for serum calcium, PTH, and ionized calcium levels, making calculations of ratios with chloride impossible. We also acknowledge that these ratios will not take the place of intact PTH testing, rather that they may aid in surveillance of cases with ambiguous lab values in the post op period, especially for patients who did not exhibit classically elevated Ca and PTH on initial presentation.
Conclusion
We believe our findings demonstrate the worth of simple lab values and calculations like the Cl: PO4 and Ca: PO4 ratios when managing patients with pHPT, including its variants. The preoperative evaluation for pHPT with Ca: PO4 was a strong predictor with a high sensitivity. The Cl: PO4, which performed inferior to Ca: PO4 pre operatively, demonstrated value in follow up and surveillance of patients. Finally, we showed that the population with normocalcemic hyperparathyroidism behaved similarly to classic patients in the postoperative period, indicating that this testing may be universally applicable to all variant forms of pHPT.
Funding
None
Conflicts of Interest
None
References
- Maruani G, Hertig A, Paillard M, et al. (2003) Normocalcemic primary hyperparathyroidism: Evidence for a generalized target- tissue resistance to parathyroid hormone. J Clin Endocrinol Metab 88: 4641-4648.
- Wright C, King D, Small M, et al. (2020) The Utility of the Cl: PO4 ratio in patients with variant versions of primary hyperparathyroidism. Otolaryngol Head Neck Surg 164: 308-314.
- Hagstrom E, Michaelsson K, Melhus H, et al. (2014) Plasma-parathyroid hormone is associated with subclinical and clinical atherosclerotic disease in 2 community-based cohorts. Arterioscler Thromb Vasc Biol 34: 1567-1573.
- Reeves CD, Palmer F, Bacchus H, et al. (1975) Differential diagnosis of hypercalcemia by the chloride/phosphate ratio. Am J Surg 130: 166-171.
- Mismar AA, Materazzi G, Biricotti M, et al. (2013) Performance of chloride phosphate test in patients with primary hyperparathyroidism. Is it related to calcium level? Saudi Med J 34: 801- 805.
- Madeo B, Vincentis SD, Repaci A, et al. (2020) The calcium-to-phosphorous (Ca/P) ratio in the diagnosis of primary hyperparathyroidism and hyperparathyroidism: A multicentric study. Endocrine 68: 679-687.
- Nelson KL, Hinson AM, Lawson BR, et al. (2016) Postoperative calcium management in same-day discharge thyroid and parathyroid surgery. Otolaryngol Head Neck Surg 154: 854-860.
- Mittendorf EA, Merlino JI, McHenry CR (2004) Post-parathyroidectomy hypocalcemia: Incidence, risk factors, and management. Am Surg 70:114-119.
- Witteveen JE, Van Thiel S, Romijn JA, et al. (2013) Hungry bone syndrome: Still a challenge in the post-operative management of primary hyperparathyroidism: A systematic review of the literature. Eur J Endocrinol 168: R45-R53.
- Lou I, Balentine C, Clarkson S, et al. (2017) How long should we follow patients after apparently curative parathyroidectomy? Surgery 161: 54-61.
- Wilhelm SM, Wang TS, Ruan DT, et al. (2016) The American Association of endocrine surgeons guidelines for definitive management of primary hyperparathyroidism. JAMA Surg 151: 959-968.
- Stack BC Jr, Bimston DN, Bodenner DL, et al. (2015) American Association of clinical endocrinologists and American college of endocrinology disease state clinical review: Postoperative hypoparathyroidism-definitions and management. Endocr Pract 21: 674-685.
Corresponding Author
Brendan C. Stack, Jr, MD, FACS, FACE, Department of Otolaryngology-HNS, Southern Illinois University School of Medicine, Springfield, IL 62702, USA.
Copyright
© 2022 Wright C. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.