Quality of Life and Psychological Disorders of Patients with Chronic Pulmonary Obstructive Disease (COPD) Admitted for Exacerbation
Abstract
We aimed to verify how many patients with COPD admitted due to exacerbation had psychological disorders such as anxiety-depression and had their quality of life affected according to specific questionnaires; as well as to know the relation of these parameters with the degree of dyspnea and affectation of their COPD descriptive study of patients admitted for COPD at a pulmonology service between January and June of 2014 was carried out. Quality of life (St. George questionnaire) and symptoms of anxiety and depression (HADS questionnaire), degree of dyspnea (MRC and Borg scores) and severity of COPD (GOLD) were assessed. In our study, 41 patients were included, 75.6% were men. We found that there was a significant correlation between patients with grade IV COPD and the presence of dyspnea > 3 on the Borg score. Likewise, the relationship between a result > 8 in the HADS questionnaire and the patients with grade IV COPD was significant. However, only a third of our patients had received psychological treatment. Most of our patients had a significant deterioration in their quality of life, probably secondary to the presence of a moderate-severe degree of dyspnea.
We consider the collaboration of the nurses of the hospitalization units to carry out screening of the psychological aspects of the patients admitted with chronic lung processes such as COPD, since their correct treatment would reduce their symptoms, such as dyspnea, improve their quality of life and, probably, reduce the number of their exacerbations.
Keywords
Chronic obstructive pulmonary disease (COPD), Quality of life, Anxiety and depression, Comorbidity, Nurse
Introduction
Chronic obstructive pulmonary disease (COPD) is characterized by a chronic and progressive course that is associated with a great impact on the quality of life and the presence of psychological problems, which implies changes in the personal and family lifestyle that generate stress. This will influence the medical and rehabilitative intervention offered to them [1-4]. There are authors who consider COPD as a systemic syndrome with multiple comorbidities, which would include certain mental problems, such as depression and anxiety [5,6]. Likewise, Matte, et al. [7] showed that, after a review of the literature, the percentage of depression in COPD (27.1%) clearly exceeded that of the control population (10%).
Dyspnoea is probably the symptom that most affects the quality of life of patients with COPD, since it generates, gradually, a decrease in physical activity. It has been shown that the greater the degree of dyspnea, the greater is the fear felt by the patient during physical exercise [8]. This influences the vital activities, provoking dependence and social isolation, which would lead to the development of symptoms of anxiety and depression [3,9-11]. This psychological symptomatology could increase in patients with COPD who require admission, especially if they have not received previous psychological-psychiatric treatment [5,6]. This can significantly mark the course of the disease. It has been shown that these symptoms can persist despite the improvement of lung function [11,12].
Therefore, the objectives of our study were to verify how many patients with COPD who were admitted due to exacerbation, had anxiety-depression according to the HADS questionnaire and if they received treatment for it; their quality of life according to the St. George questionnaire and to relate the data obtained in these questionnaires with the severity of the disease measured by the GOLD scoring system and its degree of dyspnea.
Patients and Methods
A cross-sectional, descriptive and retrospective study was performed in patients diagnosed with COPD according to GOLD (a scoring system created as a management strategy for COPD [1] aged 18 years and older, who were admitted to the Pneumology Service of La Paz University Hospital, between January and March 2014, due to exacerbation of his underlying disease.
Those who could not answer the questionnaires, who did not want to collaborate, in which the results of all the surveys were not collected or those whose cause of admission was not the exacerbation of their COPD were excluded. The nursing group, within the first 24 h of admission, was in charge of passing and supervising the St George respiratory [10] and HADS [13,14] questionnaires, as well as the mMRC and Borg dyspnea scores [15]. Their demographic data, the smoking habit and the last spirometric variables in stable period were collected to categorize the disease, as well as the treatment prior to admission.
Statistical method
Qualitative data were described as absolute frequency and percentage and quantitative ones as mean-standard deviation. The association between qualitative data was studied using Fisher's exact test. The Mann-Whitney test was used for the correlation between the quantitative data. Data were analyzed using the SAS 9.3 program (SAS Institute, Cary, NC, USA) and values of p < 0.05 were considered significant.
Ethical considerations
The authors state that no patient data appears in this article. The ethical norms of the Center have been followed, requesting authorization to the patients to participate in the answer of the questionnaires. The authors have no conflicts of interest with the study.
Results
A total of 41 (45.5%) patients in different severity scores were included in the 90 patients admitted for exacerbated COPD, of whom 31 were men (75.6%), with a mean age of 72.0 ± 11.23 (39-88) years. Table 1 shows the general characteristics of the patients. Although statistically significant relationship was not found between the character of smoker (yes, no, ex) and the degree of COPD, 69% of our patients with COPD IV were ex-smokers.
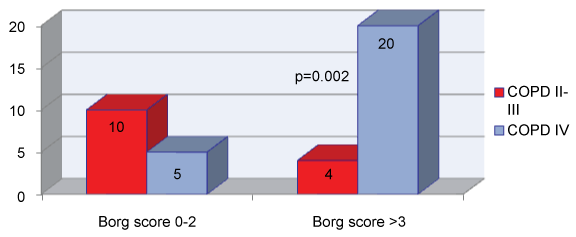
62.9% of the patients had dyspnea according to the mMRC scale between 1-2 and 56.1% between 3-6 according to the Borg score (Table 1). A significant correlation between the degree of COPD IV and the degree of dyspnea > 3 on the BORG scale (p = 0.002) was found (Figure 1). The scores obtained for the psychological variables (Table 1) indicated that more than a quarter of the sample presented a score higher than 11 (11 patients showed anxiety (25.82%) and 10 patients depression (24.34%), but only six (14.6%) patients were receiving pharmacological treatment. In this sense, we found a relationship between COPD IV with a depression score > 8 (p = 0.02).
When assessing the quality of life with the St. George Respiratory questionnaire, we saw that 92.7% presented a global alteration of the quality of life. According to each scale of the questionnaire, we observed that subscales were affected as follows: 95.1% the impact subscale (39 ± 2.5), 87.8% the symptom subscale (35 ± 3.3), and 80.5% the activity subscale (33 ± 4.2), although we did not find correlation between total scores or the ones from the subscales with the severity of COPD (in COPD grade IV, The most affected subscale was that of impact (p = 0.62).
Discussion
Patients with COPD are two to three times more likely to develop emotional problems than the general population due to the symptoms of the disease and their inability to control them effectively, poor quality of life, unhealthy living habits and a reduced survival [4]. Agreeing with previous publications, patients with COPD admitted due to exacerbation have their quality of life affected, due to increased dyspnoea and cough, worsening both as the disease progresses, and due to their successive admissions, so their measure is a good indicator of evolution [5,8,15]. In our study we found a significant impairment of quality of life as measured by the St George questionnaire, probably because most had a severe degree of COPD according to GOLD and a clinic of moderate dyspnea, which would determine a difficult physical mobilization and a progressive decrease of their social activities, measured in our work by a poor score in the impact scale of St. George questionnaire [8,11,16,17]. Although not measured in this article, there are studies that leave proof that a decreased quality of life would increase the number of exacerbations in patients with COPD [19,18,19].
Although there are articles that analyze the association between COPD and its psychological aspects and its effect on morbidity, there are few guidelines that provide solutions [19]. It has been shown that around 40% of patients with COPD develop depression and 36% have anxiety, increasing with the admission from exacerbation, as well as having a negative effect on the prognosis of COPD [4,19]. In our study, almost 33% of the patients admitted had clear psychological symptoms according to the HADS score, but very few of them were receiving treatment. We believe that it is due to the scarce research that specialists carry out on the emotional aspects of the disease in the follow-up of patients with COPD and the apprehension that some physicians have to recommend some psychiatric medicines. Several studies have concluded that depression and anxiety negatively affected the prognosis of COPD, increasing mortality, longer index stay, favoring exacerbations and re-admissions, and even affecting the total score and the impact subscale score of the St George Respiratory questionnaire [19,20].
We also found a significant correlation between grade IV of COPD and the presence of psychological symptomatology. The presence of a moderate-severe degree of dyspnea in these patients could not only be associated with their poor quality of life, but also with the depressive-anxious symptomatology they manifested. This fact is considered very important, since it has been shown that the anxiety-depression clinic would be linked to greater morbidity, negatively impact their prognosis and worsen their symptoms [4,19]. This has led to the indication of the need to carry out a screening of these psychological alterations to guide an adequate treatment that generates better quality of life and reduces morbidity and mortality [17,21].
The nursing associated with the hospitalization units of the Pneumology services provide a considerable help in the care of patients with COPD. The usual incorporation of questionnaires that allow a screening of the psychological aspects and the quality of life of these patients would be fundamental to evaluate other comorbidities that could negatively influence their morbidity and mortality. This screening work can be carried out with the collaboration of nurses of the hospitalization units in patients admitted with chronic processes such as COPD, since their correct treatment would improve their symptoms, their quality of life and probably, to reduce the number of exacerbations. The role of nursing would be key in explaining, retrieving and reviewing the questionnaires used for these purposes.
One of the most important limitations that we find in this study is that it would have been very interesting to know and link to the previous hospitalizations with the HADS questionnaire scores and the follow-up of the patients treated with clear psychological alterations in relation to the number of subsequent exacerbations, which we would like to correct in the future. Another of the limitations is the sample size that was small for all the patients that get into the hospital due to this complication. These limitations have been found in other works, since the methodology used varies, especially in the selection of the population, not only in their number but also in the variables analyzed.
Acknowledgements
Any of the authors have Conflict of Interest or have received any funding about this work.
All authors have contributed in the work planning, written and review of the manuscript.
References
- Miravitlles M, Calle M, Soler-Cataluna JJ (2012) Clinical phenotypes of COPD: Identification, definition and implications for guidelines. Arch Bronconeumol 48: 86-98.
- De Voogd JN, Wempe JB, Koeter G, et al. (2009) Depressive symptoms as predictors of mortality in patients with COPD. Chest 135: 619-625.
- Maurer J, Rebbapragada V, Borson S, et al. (2008) Anxiety and depression in COPD: Current understanding, unanswered questions, and research needs. Chest 134: 43S-56S.
- Heslop K, Newton J, Baker C, et al. (2013) Effectiveness of cognitive behavioural therapy(CBT) interventions for anxiety in patients with chronic obstructive pulmonary disease (COPD) under taken by respiratory nurses: The COPD CBTCARE study: (ISRCTN55206395). BMC Pulm Med 13: 62-68.
- Filipowski M, Bozek A, Kozlowska R, et al. (2014) The influence of hospitalizations due to exacerbations or spontaneous pneumothoraxes on the quality of life, mental function and symptomsof depression and anxiety in patients with COPD or asthma. J Asthma 51: 294-298.
- Baraniak A, Sheffield D (2011) The efficacy of psychologically based interventionsto improve anxiety, depression and quality of life in COPD: A systematic review and meta-analysis. Patient Educ Couns 83: 29-36.
- Matte DL, Pizzichini MM, Hoepers AT, et al. (2016) Prevalence of depression in COPD: A systematic review and meta analysis of controlled studies. Respir Med 117: 154-161.
- Janssens T, De Peuter S, Stans L, et al. (2011) Dyspnea perception in COPD: Association between anxiety, dyspnea-related fear, and dyspnea in a pulmonary rehabilitation program. Chest 140: 618-625.
- Rose C, Wallace L, Dickson R, et al. (2002) The most effective psychologically-based treatments to reduce anxiety and panic in patients with chronic obstructive pulmonary disease (COPD): A systematic review. Patient Educ Couns 47: 311-318.
- Yohannes AM, Willgoss TG, Baldwin RC, et al. (2010) Depression and anxiety in chronic heart failure and chronic obstructive pulmonary disease: prevalence, relevance, clinical implications and management principles. Int J Geriatr Psychiatry 25: 1209-1221.
- Altenburg WA, Bossenbroek L, de Greef MH, et al. (2013) Functional and psychological variables both affect daily physical activity in COPD: A structural equations model. Respir Med 107: 1740-1747.
- von Leupoldt A, Taube K, Lehmann K, et al. (2011) The impact of anxiety and depression on out comes of pulmonary rehabilitation in patients with COPD. Chest 140: 730-736.
- Herrero MJ, Blanch J, Peri JM, et al. (2003) A validation study of the hospital anxiety and depression scale (HADS) in a Spanish population. Gen Hosp Psychiatry 25: 277-283.
- Bestall J, Paul E, Garrod R, et al. (1999) Usefulness of the Medical Research Council (MRC) dyspnoea scale as a measure of disability in patients with chronic obstructive pulmonary disease. Thorax 54: 581-586.
- Miravitlles M, Ferrer M, Zalacain R, et al. (2004) Effect of exacerbations on quality of life in patients with chronic obstructive pulmonary disease: A 2 year follow up study. Thorax 59: 387-395.
- Ferrer M, Alonso J, Prieto L, et al. (1996) Validity and reliability of the St Georges respiratory questionaire after adaptation to a different language and culture: The Spanish example. Eur Respir J 9: 1160-1166.
- Niewoehner DE (2006) The impact of severe exacerbations on quality of life and the Clinical Course of Chronic Obstructive Pulmonary Disease. Am J Med 119: 38-45.
- Gudmundsson G, Gislason T, Janson C, et al. (2005) Risk factors for rehospitalization in COPD: Role of health status, anxiety and depression. Eur Respir J 26: 414-419.
- Atlantis E, Fahey P, Cochrane B, et al. (2013) Bidirectional associations between clinically relevant depression or anxiety and COPD: A systematic review and meta-analysis. Chest 144: 766-777.
- Ng TP, Niti M, Tan WC, et al. (2007) Depressive symptoms and chronic obstructive pulmonary disease. Effect on mortality, hospital readmission, symptom burden,functional status, and quality of life. Arch Intern Med 167: 60-67.
- Tsavlis DD, Theodorou M, Anna Tzoumaka A, et al. (2012) The impact of treatment of chronic obstructive pulmonary disease (COPD) on functional status and quality of life of patients. European Respiratory Journal 40.
Corresponding Author
Dra C Prados, Pulmonology Service, La Paz University Hospital, Paseo Castellana, 261, 28046, Madrid, Spain, Fax: 917277585.
Copyright
© 2018 Prados C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.