Mesenteric Hematoma in the Context of Recurrent Intussusception: Cause or Effect
Abstract
Intussusception is a common pediatric abdominal emergency associated with pathologic lead points in up to twenty-five percent of cases. After reduction using an air enema, the recurrence of intussusception is uncommon, but suspicion of a lead point is increased if recurrence occurs. We report on a case of recurrent intussusception where mesenteric lymphoid hyperplasia and a mesenteric hematoma were found intraoperatively and discuss their respective etiologic significance in this context.
Introduction
Intussusception is the most common abdominal emergency in young children, occurring in 56 per 100,000 children annually in the United States [1]. The cause of intussusception is most commonly idiopathic and can be associated with lymphoid (Peyer's Patch) hyperplasia acting as a lead point. Pathologic lead points refer to lesions in or around the intestine that cause the affected proximal segment to become trapped in the uninvolved distal segment by peristalsis, causing intussusception. Pathologic lead points have been reported in 12.5-25% of cases and include Meckel's diverticulum, intestinal wall hematomas, mesenteric cysts, and tumors [2].
The treatment of choice for intussusception is non-operative reduction using pneumatic pressure by enema (air enema) [2]. Recurrent intussusception after air enema reduction is infrequent with recurrence risks of 2.2% to 3.9% and 2.7% to 6.6% after the first 24 hours and 48 hours post-reduction, respectively [3]. In one study, the probability of recurrence post-reduction was 100% after the fourth episode of intussusception [4]. With recurrences post-reduction, the presence of a pre-existing pathologic lead point should be considered and operative management is generally required [5].
While pathological lead points can result in recurrent intussusception, the authors are not aware of reports in the English literature of similar lesions occurring as the result of recurrent intussusception. We present the first documented case of idiopathic recurrent intussusception resulting in a mesenteric hematoma.
Case
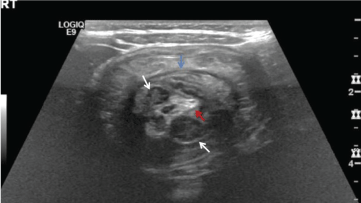
A two-year-old girl with no significant medical history presented to the Emergency Department with a two-day history of diarrhea, a one-day history of recurrent abdominal pain, and two episodes of green gelatinous stools mixed with bright red blood. The patient did not have any fevers, congestion, rhinorrhea, rash or other systemic symptoms. Her physical exam was unremarkable. Complete blood count and liver function tests were normal. An ultrasound demonstrated ileocolic intussusception and mesenteric lymphoid hyperplasia (Figure 1). The patient underwent successful reduction with air enema. Over the next 48 hours, she had 3 recurrences, each reduced successfully with air enema. On her 5th recurrence, pediatric surgery was consulted and the decision was made to bring the patient to the operating room for diagnostic laparotomy.
Per report from the surgeon, upon physical inspection the appendix and cecum appeared thick and inflamed. The ileocecal valve was demonstrated to be in the appropriate location and therefore there was no intussusception noted at that time. Approximately 10-15 cm proximal to the ileocecal valve a lesion was encountered in the mesentery impinging on the ileum. The lesion was described as a hematoma vs. vascular anomaly, approximately 1 cm in diameter, with surrounding prominent lymph nodes. The bowel was noted to be normal proximal to the lesion, but thickened and discolored distally. The mesenteric lesion and bowel immediately adjacent to it was resected and an end-to-end anastomosis was performed. The resected bowel segment with lesion was sent to pathology for examination and diagnosis.
Post-operatively, the patient's mother was asked about any recent trauma which was denied. No external injuries were documented in the medical record. On post-operative day #2, the Child Abuse Team was notified due to the concern of the mesenteric hematoma without a known etiology. Computed Tomography (CT) of the abdomen and pelvis with intravenous and oral contrast, a skeletal survey, and coagulation studies were recommended by the Child Abuse Team. Ultimately, the imaging studies did not reveal any additional injuries and the coagulation studies were normal.
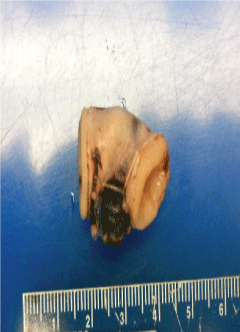
Pathological examination of the specimen revealed an unoriented segment of bowel, 2.2 cm long and up to 1.5 cm in diameter, open at both ends. There was a circumscribed, dark red nodule, 0.8 cm diameter, in the scant mesentery included with and adjacent to the bowel. The serosa showed focal small hemorrhages, the wall was without lesions including hemorrhage, and the mucosa was tan with few punctate hemorrhages and a small submucosal hemorrhage. Lymph nodes were not received with the bowel segment. Histologic examination revealed a recent hematoma in the mesentery, without hemosiderin on iron stain, as well as small submucosal hemorrhage. There was no lesion, including vascular malformation, inflammation, or neoplasm. The bowel was viable (Figure 2).
Discussion
A mesenteric hematoma is a focal collection of blood in the mesentery most frequently caused by blunt force abdominal trauma; though infrequent, the most common accidental mechanism is a motor vehicle crash [6,7]. Non-traumatic causes include aneurysmal vessel dilation, vasculitis/connective tissue disease, spontaneous hemorrhage while on anti-coagulation therapy, acute pancreatitis, Crohn's disease, duodenal stenosis, and incarcerated inguinal hernia [7].
When traumatically generated, the mechanism of injury of mesenteric hematomas in such cases are due to compression of the bowel and deceleration forces [8]. Injury to the mesentery can have downstream effects on the bowel. Traumatic intussusception has been previously described, though it is rare with only 22 cases being reported in the English literature [9]. Intramural bowel hematomas were reported in four of these 22 cases, but a hematoma arising in the mesentery was not described [9].
In young children, intraabdominal injuries are the second leading cause of death due to physical abuse, with the most commonly injured structures being the small bowel (especially duodenum and proximal jejunum), the left lobe of the liver, and the pancreas-however, any abdominal tissue or organ can be injured in the context of child physical abuse [10,11]. When the mesenteric hematoma was identified in our patient without a well-described history of blunt force trauma to account for the injury, child physical abuse was considered.
Ultrasound is the modality of choice to diagnose intussusception. However, it has poor sensitivity for identifying pathologic lesions [5]. In addition, ultrasound has a low sensitivity for detection of mesenteric injuries with CT being the preferred imaging modality for such injuries [12]. If intussusception has multiple recurrences, a patient usually undergoes surgical intervention and CT imaging is not routinely obtained. In this patient, one of the lymph nodes detected ultrasonographically could have been the mesenteric hematoma found intraoperatively, calling into question whether the intussusception was caused by the mesenteric hematoma or could have been the result of the mesenteric hematoma.
Given the clinical context, the etiology of the mesenteric hematoma and intussusception in this patient was difficult to determine prior to final pathological diagnosis. The average age for presentation of both intussusception and non-accidental abdominal trauma is 2 years, and both entities may demonstrate significant overlap in clinical symptoms, making them difficult to distinguish at initial presentation [12]. An additional clinical overlap in this case was the coexistent mesenteric hematoma with surrounding lymph node hyperplasia. Lymph node hyperplasia is a well-described cause for idiopathic intussusception, however it has never been described in the presence of concurrent mesenteric hematoma [13]. Any cause of local inflammation, including trauma, may result in lymphadenopathy, which makes this a nonspecific finding [13]. Lymphoid hyperplasia precipitating intussusception is most commonly associated with a preceding viral illness, which was not reported in this patient [14]. In addition, lymphoid hyperplasia is not commonly associated with multiple recurrences of intussusception post-reduction with air enema [15].
When recurrent intussusception occurs in association with lymphoid hyperplasia, there should be consideration for presence of a pathologic lead point [15]. To our knowledge, this is the first case demonstrating a mesenteric hematoma resulting from recurrent intussusception in a search for said leadpoint. In this patient, the consideration for nonaccidental abdominal trauma resulting in the mesenteric hematoma was appropriate given her clinical findings. However, the interpretation by the pathologist in conjunction with clinical correlation and review of the available literature were both paramount in making the appropriate diagnosis in this case.
Patient Consent
Consent to publish the case report was not obtained. This report does not contain any personal information that could lead to identification of the patient.
Funding
No funding or grant support.
Authorship
All authors attest that they meet the current ICMJE criteria for authorship.
Conflict of Interest
None of the authors have any financial disclosures (RS).
References
- Fisher J, Sparks E, Turner C, et al. (2015) Operative indications in recurrent ileocolic intussusception. J Pediatr Surg 50: 126-130.
- Carroll A, Kavanagh R, Ni Leidhin C, et al. (2017) Comparative effectiveness of imaging modalities for the diagnosis and treatment of intussusception. Acad Radiol 24: 521-529.
- Gray M, Li SH, Hoffmann RG, et al. (2014) Recurrence rates after intussusception enema reduction: A meta-analysis. Pediatrics 134: 110-119.
- Hsu WL, Lee HC, Yeung CY, et al. (2012) Recurrent intussusception: When should surgical intervention be performed? Pediatr Neonatol 53: 300-303.
- Lin XK, Xia QZ, Huang XZ, et al. (2017) Clinical characteristics of intussusception secondary to pathologic lead points in children: A single-center experience with 65 cases. Pediatr Surg Int 33: 793-797.
- Reece R, Christian C (2009) Child abuse medical diagnosis & management. (3rd edn), American Academy of Pediatrics, Elk Grove Village, Illinois, US.
- Shikata D, Nakagomi H, Takano A, et al. (2016) Report of a case with a spontaneous mesenteric hematoma that ruptured into the small intestine. Int J Surg Case Rep 24: 124-127.
- Wang R, Chong C, Hsu H, et al. (2006) Mesenteric injury caused by minor blunt abdominal trauma. Emerg Med J 23: e27.
- Paul K Kleinman (2015) Diagnostic Imaging of Child Abuse. (3rd edn), cambridge University Press, Cambridge, UK, 575-576.
- Lindberg DM, Shapiro RA, Blood EA, et al. (2013) Utility of hepatic transaminases in children with concern for abuse. Pediatrics 13: 268-275.
- Carole Jenny (2011) Child Abuse and Neglect: Diagnosis, Treatment and Evidence. St. Louis, Elsevier Saunders.
- Bège T, Brunet C, Berdah S (2016) Hollow viscus injury due to blunt trauma: A review. J Visc Surg 153: 61-68.
- Lucey B, Stuhlfaut J, Soto J (2005) Mesenteric lymph nodes seen at imaging: Causes and significance. Radiographics 25: 351-365.
- Bhisitkul DM, Todd KM, Listernick R (1992) Adenovirus infection and childhood intussusception. Am J Dis Child 146: 1331-1333.
- Shteyer E, Koplewitz BZ, Gross E, et al. (2003) Medical treatment of recurrent intussusception associated with intestinal lymphoid hyperplasia. Pediatrics 111: 682-685.
Corresponding Author
Richard Sidlow, Department of Pediatrics, Staten Island University Hospital-Northwell Health, 475 Seaview Avenue, Staten Island, New York 10305, USA, Tel: 516-581-9084; 718-226-6969, Fax: 718-226-1128.
Copyright
© 2018 Steiner MM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.