Resistant Posterior Semicircular Canal BPPV with Changing Oculomotor Pattern Solved with Mastoid Vibration Application
Abstract
The use of mastoid vibration in addition to repositioning maneuvers for the treatment of benign paroxysmal positional vertigo of the posterior semicircular canal (PSC-BPPV) was described for the first time by Epley. There is evidence in the literature that the additional use of mastoid vibration could provide a substantial advantage also in the treatment of the apogeotropic variant of BPPV of the horizontal semicircular canal (HSC-BPPV). The present is a case report about a patient with a left PSC-BPPV resistant to the conventional treatment with Epley repositioning maneuver. This patient showed an uncommon response to the repositioning maneuver: a recurrent canal switch into the HSC and a temporary apogeotropic variant of PSC-BPPV. A possible explanation of our findings is reported along with a discussion about the usefulness of mastoid vibration in such case.
Keywords
Benign paroxysmal positional vertigo, Otolithic membrane, Positional nystagmus, Semicircular canals, Mastoid vibration
Introduction
Benign paroxysmal positional vertigo (BPPV) is caused by free otoconia dislodged from the utricle macula and entering into the semicircular canal. In most of the cases the otoconial debris gravitates into the posterior semicircular canal (PSC). In the typical form, when otolith debris are localized in the ampullary arm of the canal, the Dix-Hallpike positional maneuver causes the otoconial shift away from the ampulla with an ampullofugal endolymphatic flow and a consequent excitatory cupular deflection, according to the second Ewald law. The clinical sign is a paroxysmal left-torsional, up-beating, nystagmus for the left PSC, and right-torsional, up-beating, nystagmus for the right PSC [1].
Some authors described a "reversed" nystagmus in some cases of PSC-BPPV: a right-torsional, down-beating nystagmus for the left PSC, a left-torsional, down-beating nystagmus for the right one. These findings have been interpreted with a localization of the debris in the non-ampullary arm of the PSC. In this case, the Dix-Hallpike position maneuver causes an ampullopetal (i.e. toward the ampulla) endolymphatic flow and a consequent inhibitory cupular deflection. This particular form of PSC-BPPV has been named as apogeotropic variant or pseudo-anterior canalolithiasis [2,3].
Here we report the case of a left PSC-BPPV resistant to the conventional treatment with Epley repositioning maneuver. This patient showed an uncommon response to the repositioning maneuver: a recurrent canal switch into the horizontal semicircular canal (HSC) BPPV and a temporary apogeotropic variant of PSC-BPPV. We speculate on the mechanism of this clinical findings and discuss about the usefulness of mastoid vibration in vertigo resolution.
Case Presentation
A 67-year-old female came to our observation at the Otolaryngology Department (tertiary referral center) of the University of Perugia (Italy), complaining of brief positional vertigo triggered by head movements.
During the left Dix-Hallpike positioning test, we observed a paroxysmal left-torsional, up-beating nystagmus, suggestive of left PSC-BPPV. Epley repositioning maneuver was carried out but, at the following Dix-Hallpike control test, a horizontal, left-beating nystagmus appeared. The following McClure maneuver [4] showed a bipositional geotropic nystagmus, more intense on the left head position, suggesting a canal switch into a left HSC-BPPV. The latter was solved completely by Gufoni liberatory maneuver [5].
Two months later, the patient came back to our attention for a left PSC-BPPV recurrence, but in this case, repeated Epley repositioning maneuvers showed no effectiveness.
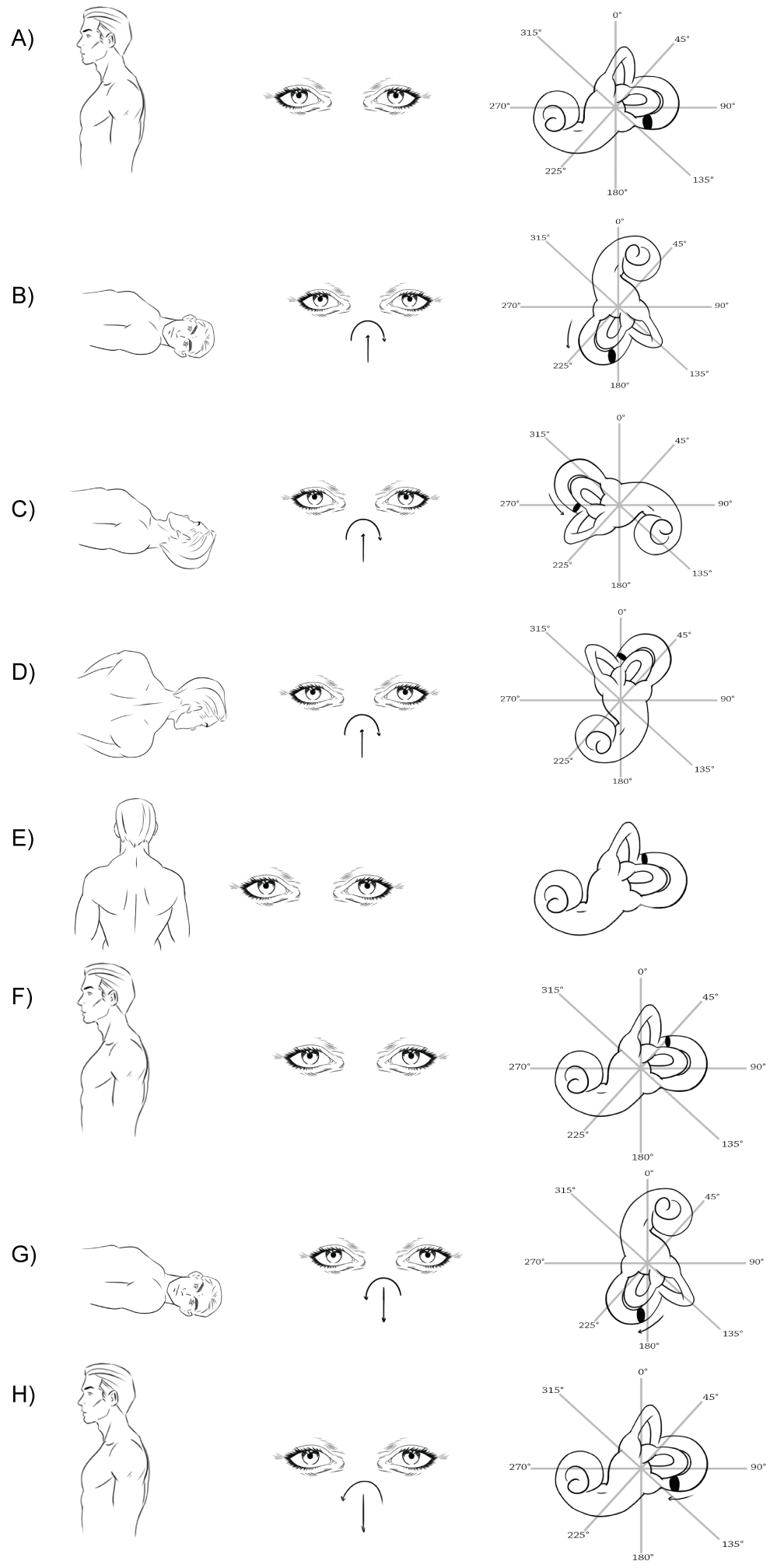
In particular, the left Dix-Hallpike positioning test initially evoked a typical left-torsional, up-beating nystagmus (Figure 1A and Figure 1B). After Epley repositioning maneuver (Figure 1C, Figure 1D and Figure 1E), a reversed right-torsional, down-beating nystagmus appeared on the left Dix-Hallpike control test (Figure 1F and Figure 1G), followed by a right-torsional, down-beating nystagmus when the patient returned to the sitting position (Figure 1H). Finally a typical left-torsional, up-beating nystagmus appeared again on a new left Dix-Hallpike position. We waited at least one minute between the different maneuvers.
Therefore, we applied a mastoid vibration [1,6,7] (Frequency: 100 Hz; Amplitude: 0,8 mm) for 60 seconds prior to left Dix-Hallpike test. A typical nystagmus for left PSC-BPPV was noticed again. After the Epley maneuver, the following left Dix Hallpike positioning test showed, this time, a geotropic horizontal, left-beating nystagmus responsive (i.e. vertigo resolution) to Gufoni maneuver for the left HSC-BPPV after confirmation by means of McClure positioning maneuver. No recurrence was observed at subsequent controls.
Discussion
The oculomotor changing pattern observed in our case may have the same physiologic explanation of the so-called pseudo-anterior canalolithiasis described by Imai et al (i.e. shift of the otoconial debris between the two parts of the PSC), but with an opposite timing. In fact, while in Imai's report, the case explanation was related to the shift of otoconial debris from the non ampullary to the ampullary part of the PSC in response of an inverted Epley maneuver [3], in our case the movement of the debris may be related to the shift from the ampullary arm of the PSC to the non ampullary one after an incompletely effective Epley repositioning maneuver.
In particular, an extensive possible physiological mechanism for our BPPV case could be the following: the otoconial debris are originally located in the proximal arm of the PSC (Figure 1A), as demonstrated by the typical nystagmus evoked on the first Dix-Hallpike test (Figure 1B). During Epley repositioning maneuver (Figure 1C, Figure 1D and Figure 1E), the debris encountered an obstacle on its path, such as a canalar stricture or a plugging caused by a large otoconial mass, which blocks its progression toward the utricle into the non ampullary arm of the PSC (Figure 1F). Afterwards, the repetition of Dix-Hallpike test causes, this time, an ampullopetal shift of the debris (Figure 1G) with a return of the otoliths into their original position during the return to the sitting position (Figure 1H).
Although no statistically significant difference emerges in literature between the internal height of the posterior semicircular canal considering three points of measurement (proximal, mid and distal part) [8], we hypothesize that this patient could exhibit an anatomical anomaly. In our opinion, in the adjacency of the common crus, the internal lumen of the canal would be narrower, thus blocking the progression of the mass through the canal and determining the resistance to the repositioning maneuver. Alternatively, we could consider an obstruction of the distal end of the posterior semicircular canal under the effect of a large otoconial mass or jam caused by the confluence of the debris. The otoconial mass would stop in the distal part of the canal and then would fall under the action of gravity, provoking an ampullopetal endolymphatic flow with a "reversed" nystagmus on the second Dix-Hallpike positioning test. At this point, the debris stops again in the ampullary arm. This would be the reason why the returning from the declivous to the orthostatic position evokes a peculiar reversed nystagmus (right torsional, down beating) and the following Dix-Hallpike test produces the typical nystagmus rather than a negative clinical finding.
We may also speculate on the possibility to observe multiple oculomotor patterns in different positions in case of multicanal involvement in BPPV. In our case, however, this possibility can be excluded since the different oculomotor patterns were observed individually in a single positioning maneuver and not simultaneously in different positions. For this reason the various types of nystagmus observed in our case are better explained by an intracanal (i.e. from the ampullary to the non ampullary part of the PSC), or intercanal (i.e. from the PSC to the HSC) shift of the otolitic debris.
The possibility of otoliths flow into the HSC during Epley repositioning maneuver for a PSC-BPPV is well known [9]. However, the reasons of this event are still not clear. Some authors suggest a role of head position during Epley maneuver and recommend the necessity of maintaining the head strictly at 30 ℃ below the horizontal plane to avoid canal conversion [10]; others state that Dix Hallpike control test itself or other repositioning maneuvers performed too soon (from 1 to 15 minutes later) could lead to this complication [11]. Other authors propose that at the end of Epley maneuver a large mass of otoconia may be located in the utricle and near the opening of the semicircular canals [12]. In particular, the opening of the HSC is adjacent to the common crus and for this reason, there is a high risk of debris re-entry, especially when the head hangs for some time.
Another interesting aspect is that this case is a further proof about the existence of the apogeotropic variant of PSC BPPV (e.g. pseudo-anterior canalolithiasis), together with its mechanism and peculiar behavior (temporary and reversible nystagmus).
Finally, the mastoid vibration proved to be useful to solve the canal jam, reduce the otoconial mass volume and enable it to reach the utricle as effect of the therapeutic maneuver. The use of mastoid vibration for the treatment of PSC-BPPV was described for the first time by Epley in addition to repositioning maneuvers. It has also been proved in the literature that the additional use of mastoid oscillation provides a substantial advantage in treating the apogeotropic variant of benign paroxysmal positional vertigo of HSC-BPPV [1,6,7]. On the basis of our experience, this procedure could be tempted also in the treatment of the PSC-BPPV presenting in its apogeotropic variant.
References
- Epley JM (1992) The canalith repositioning procedure: for treatment of benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg 107: 399-404.
- Paolo Vannucchi, Rudi Pecci, Beatrice Giannoni (2012) Posterior semicircular canal benign paroxysmal positional vertigo presenting with torsional downbeating nystagmus: an apogeotropic variant. Int J Otolaryngol 2012: 413603.
- Imai T, Masumura C, Takeda N, et al. (2013) Pseudo-anterior canalolithiasis. Acta Otolaryngol 133: 594-599.
- McClure JA (1985) Horizontal canal BPV. J Otolaryngol 14: 30-35.
- Gufoni M, Mastrosimone L (1998) Trattamento con manovra di riposizionamento per la canalolitiasi orizzontale. Acta Otorhinolaringol Ital 18: 363-367.
- Mario Faralli, Fabrizio Longari, Giampietro Ricci, et al. (2008) Mastoid Oscillation in the Treatment of the Apogeotropic Variant of Benign Paroxysmal Positional Vertigo of the Lateral Semicircular Canal. Mediterr J Otol 2008: 152-156.
- Li JC (1995) Mastoid oscillation: a critical factor for success in canalith repositioning procedure. Otolaryngol Head Neck Surg 112: 670-675.
- Lee JY, Shin KJ, Kim JN, et al. (2013) A Morphometric Study of the Semicircular Canals Using Micro-CT Images in Three-Dimensional Reconstruction. Anat Rec (Hoboken) 296: 834-839.
- Lin GC, Basura GJ, Wong HT, et al. (2012) Canal Switch After Canalith Repositioning Procedure for Benign Paroxysmal Positional Vertigo. Laryngoscope 122: 2076-2078.
- Herdman S (2007) Vestibular Rehabilitation. F. A. Davis, Philadelphia, United States of America.
- Foster CA, Zaccaro K, Strong D (2012) Canal Conversion and Reentry: A Risk of Dix-Hallpike During Canalith Repositioning Procedures. Otol Neurotol 33: 199-203.
- Anagnostou E, Stamboulis E, Kararizou E (2014) Canal conversion after repositioning procedure: comparison of Semont and Epley maneuver. J Neurol 261: 866-869.
Corresponding Author
Luca D'Ascanio, MD, Department of Otolaryngology- Head & Neck Surgery, "Carlo Poma" Civil Hospital, Strada Lago Paiolo 10- 46100 Mantova, Italy, Tel: 0039-3283186967, Fax: 0039-0376201624.
Copyright
© 2017 Faralli M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.