Serum Homocysteine Levels in Patients with Retinal Vein Occlusion in a Spanish Population
Abstract
Purpose
To evaluate the clinical effectiveness and cost of switching to Mydrane™ for anaesthesia and mydriasis during cataract surgery.
Methods
The clinical outcomes and cost of using Mydrane™ during cataract surgery in a UK community hospital was benchmarked against published reference standards. 129 patients who underwent routine cataract surgery using Mydrane™ for combined anaesthesia-mydriasis were identified from an electronic database. Pupil dilation was measured using video image analysis. Factors affecting the variation in pupil size immediately prior to capsulorhexis were explored using multiple logistic regressions. The cost of changing mydriasis-anaesthetic practice was also assessed.
Results
The mean age of patients was 7-years-older compared to the gold standard. Throughout surgery, mydriasis was smaller by 0.5-0.7 mm and was unaffected by tamsulosin use or iris colour. Age and preoperative mydriasis with G tropicamide 1% significantly explained most of the variation in pupil diameter prior to capsulorhexis (p < 0.05). All patients requiring mechanical pupil dilation had pupils that dilated to less than 5 mm preoperatively. The visual results and complication profiles matched that of the reference standard. There was a marginal increase in cost of switching over to the use of Mydrane™.
Conclusions
Mydrane™ can provide acceptable anaesthesia and mydriasis in a non-selected group of patients, regardless of iris colour. The higher cost can be offset by removing adrenaline from the infusion fluid and using mechanical dilation if a pupil dilates to less than 5 mm preoperatively.
Introduction
The demand for cataract surgery is growing as the population ages and the thresholds for surgery decrease [1]. In-order to meet this increased demand with limited resources, there is increasing emphasis on modifying the pathway for cataract surgery to increase efficiency. The pathway consists of referral, preoperative assessment, admission for day case surgery, the surgery, the post-operative discharge and usually a single follow up visit. Dilation of the pupil is required twice in the pathway, first during preoperative assessment and again on the day that surgery is scheduled. A high-volume pathway for cataract surgery at Bishops Wood hospital in the UK, involved patients being supplied with G tropicamide 1% to use in both eyes 1 hour prior to their preoperative assessment by 3 of the authors (CKP, JT, TW). On the day of their surgery G tropicamide 1% and G phenylephrine 2.5% was applied 4 times at 5 minute intervals by band 6 nursing staff that used hand sanitiser before and after each of the 4 rounds of dilating drops. The standard anaesthetic technique used for surgery consisted of applying 3 drops of G Proxymetacaine 0.5% in the anaesthetic room followed by a subconjunctival injection of lignocaine 2% in the operating room. In 2015 an intracameral preparation, Mydrane™ (Laboratoires Thea, Clermont-Ferrand, France) was developed to achieve both anaesthesia and mydriasis and shown in a phase 3 randomised controlled trial to allow adequate mydriasis for cataract surgery [2]. Our cataract surgery pathway was modified in 2016 so that patients arriving for surgery did not receive mydriasis prior to surgery. Intracameral Mydrane™ was used instead to achieve combined anaesthesia and mydriasis in the operating room. Our aim was to audit the results of cataract surgery using this modified pathway compared against reference standard clinical trial [2] data, in a non-selected cohort of patients undergoing surgery over a 3 month period from 2nd of August 2016 and to cost compare the old and new pathways.
Method
Clinical management
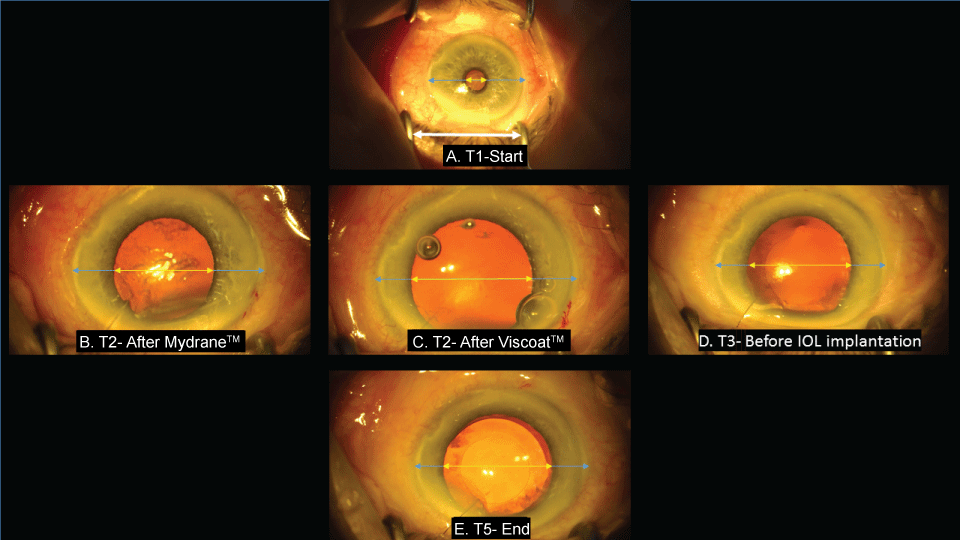
The hospital clinical governance committee granted permission for the audit which also adhered to the tenets of the Declaration of Helsinki. Consecutive patients in whom Mydrane™ was used for cataract surgery performed by one of the authors (CKP, an experienced surgeon) between 2nd August and 27th October 2016 at Bishops Wood Hospital were identified from an electronic patient record by one of the authors (JHP). The following preoperative data was extracted into statistics software (STATATM 14.2. (2016). Texas: Stata Corporation LP): age, gender, presence of diabetes, pseudoexfoliation, use of tamsulosin, best corrected preoperative LogMAR visual acuity and horizontal pupil diameter following dilation by G tropicamide 1% determined by slit lamp examination or from ocular biometry using the IOL Master™ 500 (Carl Zeiss Meditec AG, Jena, Germany). Scheduling of patients for surgery remained at four patients at the start of the operating session followed by 3 patients attending every hour. The modified surgical pathway consisted of bringing a patient into the anaesthetic room and administering 3 drops of G proxymetacaine 0.5% at 15 second intervals followed by application of G Povidone Iodine 5% Minims™. In the operating room, surgery was performed using the Zeiss OPMI Lumera™ (Carl Zeiss Meditec AG, Jena, Germany) microscope with integrated video capture facility. 200 µl Mydrane™ was injected into the anterior chamber through a 2.5 mm superotemporal corneal incision. Viscoat™ (Alcon Laboratories, Inc., Texas, USA) was then injected to deepen the anterior chamber and then applied onto the cornea to maintain clarity. Two side-port incisions were made in the lower temporal and upper nasal limbus. Phaco-chop with a Kelmann 30º tip and Ayliffe™ chopper was used to disassemble and aspirate the nucleus with vacuum setting on the Alcon Infiniti™ of 450 mmHg and infusion of BSS Plus™ to which was added 0.3 mls of 1:10000 adrenaline. The cortex was removed using bimanual aspiration. A Hoya iSert® 250 (Hoya Surgical Optics, Tokyo, Japan) lens implant was injected following inflation of the capsular bag with Provisc™ (Alcon Laboratories, Inc., Texas, USA) which was then aspirated. 1 mg intracameral cefuroxime was the antibiotic of choice with subconjunctival gentamicin-lignocaine 2.0% used in patient's allergic to penicillin. Video frame grabs were taken at the start (T1), following intracameral injection of Mydrane™, when the pupil had stopped dilating (T2), following use of Viscoat™ to deepen the anterior chamber (T3), prior to lens insertion (T4) and when surgery was complete (T5) (Figure 1) as per the reference publication. File names for each grabbed image included a time-stamp. The following were recorded: image capture failure, the duration of surgery defined as deducting the time stamp of T1 from T5, use of supplemental anaesthesia during surgery, any step to augment mydriasis for example mechanical dilation of the pupil, anterior capsule rim tears and posterior capsule rupture. Patients underwent optometry review 10-14 days following surgery. The following were recorded: best corrected LogMAR visual acuity, whether the patient's vision had improved and the requirement for further surgery such as need to aspirate residual lens material. Intraoperative pupil size was measured independently by one of the authors (JHP) using Image JTM open source software. Horizontal pupil diameter in mm was determined by measuring the horizontal corneal and pupil diameter in pixels and then calibrating this against measurement of the speculum in the T1 image (Figure 1). Iris colour was classified from the T1 image as blue, green, hazel or brown comparing against a template prepared by one of the authors (CKP). Stata™ was used for statistical evaluation. Change in vision resulting from surgery was compared using Students t-test. Multiple linear regression analysis was used to determine how age, iris colour, preoperative mydriasis, use of tamsulosin and the presence of diabetes or pseduexfoliation explained the variation in pupil size preceding capsulorhexis (T3). A p-value of less than 0.05 was deemed statistically significant.
It was assumed that upon admission it would take one minute for a band 6 nurse to administer one round of drops to the eye. Four rounds need to be given making a total time of 4 minutes.
Results
Clinical
Table 1 shows the data in the audit compared against the reference standard group of patients treated with Mydrane™ in the phase 3 trial undertaken by Labetoulle [2]. Table 2 summarizes missing data in the audit.
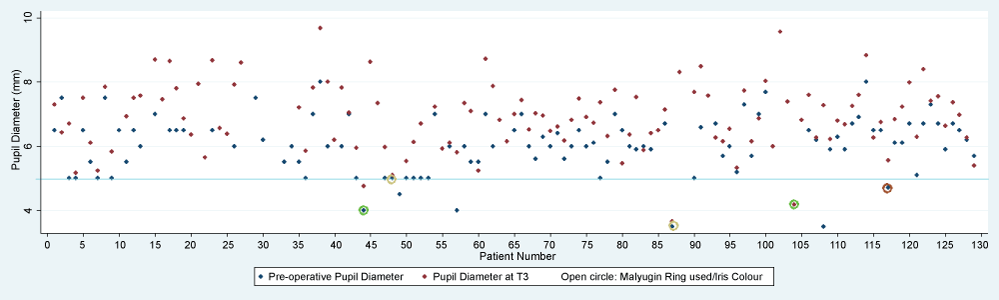
The sex ratio was similar for both groups. The patients in our audit were older by a mean age of 6.4 years. The mean duration of the surgery was 13.41 ± 2.70 minutes [N = 104] in our audit. Mydriasis remained stable throughout surgery in all cases. There was a statistically significant improvement in best corrected visual acuity following surgery from a mean LogMAR of 0.58 (6/24) to 0.08 (6/7.5) (p < 0.05). 97.7% patients [125/129] felt their vision was better at the post-operative visit. The mean horizontal pupil diameters ± SD [N] were T1: 2.37 ± 0.43 mm [n = 119], T2: 5.98 ± 0.97 mm [n = 109], T3: 6.90 ± 1.05 mm [n = 117], T4: 7.03 ± 1.07 mm [n = 108], T5: 6.87 ± 1.22 mm [n = 103]. The distribution of iris colour was; blue: 27.12%, green: 25.42%, hazel: 26.27%, brown: 21.19%. For sub-group analysis pupil dilation is defined as pupil diameter at T1 subtracted from that at T3. Mean pupil dilation ± SD in mm for each iris colour was: blue: 4.51 ± 0.82, green: 4.48 ± 082, hazel: 4.53 ± 0.99, brown: 4.58 ± 0.67. The mean pupil dilation ± SD for patients on Tamsulosin was 4.24 ± 0.86 compared with patients not on Tamsulosin: 4.60 ± 0.83. The mean pupil dilation ± SD of diabetic patients was 4.65 ± 0.69 compared to non-diabetic patients: 4.54 ± 0.87. There were 13% fewer patients with a pupil more than 6 mm at T3 in the audit, compared to the reference publication. No patients required supplemental anaesthesia. 3.9% (5/129) of patients required mechanical dilation of the pupil. If pupils that dilate to less than 5 mm with G tropicamide 1% preoperatively are considered, 57% (4/7) patients required mechanical dilation of the pupil (Figure 2). The other 3 patients dilated to well above 5 mm in response to Mydrane™. Only 1 case of a pupil dilating to 5 mm preoperatively required pupil expansion. Regression analysis indicated that 48.8% of the variation in pupil size before capsulorhexis was explained by the factors we included in our model. Age and preoperative mydriasis with tropicamide 1% were the only statistically significant variables (p < 0.05). Insignificant variables included iris colour, use of Tamsulosin and the presence of diabetes or pseduexfoliation (p > 0.05).
Cost effectiveness
Table 3 compares the direct and indirect costs of the new pathway versus the old for achieving mydriasis and anaesthesia. There is a 60% increase in cost for pupil and anaesthetic management per procedure with the new regimen which for 129 patients amounted to a total cost difference of £429.57.
Discussion
Intracameral mydriatics and anaesthetics are not new [3]. They have, however, been used as unlicensed products that are prepared by the operating nurse with the attendant pitfalls of additional time required and the possibility of drug concentration or contamination error which increases the risk of endothelial compromise or infection. This audit has shown that although the mean pupil diameter was approximately 0.5 mm smaller at each stage of surgery compared with the reference publication, it was possible to successfully adopt the use of Mydrane™, a commercial mydriatic-anaesthetic combination, by an experienced surgeon in a non-selected group of patients. Our audit confirmed that age and preoperative response to G tropicamide 1% are clinically the most useful variables that predict intra operative performance of Mydrane™. An explanation for reduced mydriasis in our audit is that patients were not excluded based on preoperative pupil diameter. In the reference publication, patients with a preoperative dilated pupil of below 7 mm were excluded. In our cohort, patients were not excluded based on preoperative dilated pupil diameter and the known inverse relationship between age and pupil size [4] is likely to have resulted in age selection bias explaining why the mean age of our sample was 6 years greater than in the reference publication. The presence of Pseduoexfoliation was not statistically significant but this may be a spurious given that only 1 patient in our audit had the disorder. The presence of diabetes was also found to be insignificant. This may reflect the fact that our audit did not record the duration of diabetes and the presence of diabetic retinopathy, which are associated with poor mydriasis [5]. The use of Tamsulosin was also insignificant in explaining variation in pupil size. However, pupil behaviour in patients treated with Tamsulosin is variable with approximately a 50% incidence of pupils that dilate normally [6]. Using Mydrane™ is likely to be effective prophylaxis against intra operative floppy iris syndrome given that intracameral phenylephrine has been shown to be effective in randomised controlled trials [7]. Uncertainty has been expressed about the response of dark irises to Mydrane™ [8]. This audit has found that a dark iris does not compromise the mydriatic response to Mydrane™. There was one case in this audit where a nuclear remnant was likely to have remained hidden under the iris requiring additional surgery. The pupil diameters (mm) in this case were: T1: 3.14, T2: unavailable, T3: 8.71, T4: 8.61, T5: 8.67 - one cannot therefore ascribe this complication to a small pupil. Caution needs to be exercised about extrapolating the safety of using Mydrane™ to different scenarios for example a) When trainee surgeons are operating, and b) When using nuclear disassembly techniques such as divide and conquer that require better visualization to the periphery of a cataract. Our audit found that when the preoperative pupil dilation to G tropicamide 1% was less than 5 mm, 4/7 (57%) patients required pupil expansion. Those patients that did not require expansion of the pupil (3/7) are assumed to have been sub-optimally dilated. If additional tropicamide 1% and phenylephrine 10% were used in these patients at the preoperative assessment, their pupils would likely dilate beyond 5 mm as they dilated to above this mark intra operatively (these pupils were preoperatively: 3.5, 4.0 and 4.7 millimeters and intraoperatively were: 7.28, 5.80 and 5.56 millimeters respectively). Pupil expansion could then be planned for all patients still dilating to less than 5 mm, avoiding the cost of using Mydrane™ in these cases. There is evidence that adding adrenaline to the infusion fluid may not be required when using intracameral mydriatics which could allow further improvement in cost effectiveness and workload in the operating room when using Mydrane™ [9]. The increase in cost of using Mydrane™ was £3.33 per patient. This marginal increase could easily be offset by improved operating room utilisation, one example being to possibly operate on an extra patient per list. On top of this, it is the surgeon's (CKP) impression that list flow has improved and that the pressures on nurses have reduced since Mydrane™ was first used. This is supported by evidence that patients spend less time in the hospital on the day of surgery [2]. Given the improved list flow a lower grade of nurse may be capable of assisting potentially providing another cost saving avenue. Another advantage is the potential for reducing the risk of cardiovascular complications given that systemic bioavailability of mydriatics is reduced by using Mydrane™ [2].
This audit has confirmed that it is safe for an experienced surgeon to incorporate the use of a new licensed combined intracameral mydriatic-anaesthetic combination of lignociane 1%, tropicamide 0.02% and phenylephrine 0.31% for patients undergoing routine cataract surgery including those with dark irises and those being treated with Tamsulosin. The changes our team plan to implement following the audit are to a) Instil additional mydriatic in any patient with a preoperative pupil diameter less than 5 mm at pre-assessment and consider the use of pupil expansion in those patients whose pupil remains below 5 mm and b) To stop using adrenaline in the infusion fluid.
Conflict of Interest
1. All authors declare there are no competing or financial interests. No funding or external support was received.
2. All authors of this paper have directly participated in planning, execution of the study and preparation of the manuscript.
3. All authors have read and approved the version submitted to the Journal.
4. The contents of the manuscript are original and have not been published earlier. C.K. Pate has received honoraria for lectures at meetings sponsored by Thea and Keith Davey has received payment from Thea for lectures and consultancy work. Thea was not involved in formulating the content of this article.
References
- Taylor HR (2000) Cataract: how much surgery do we have to do? Br J Ophthalmol 84: 1-2.
- Labetoulle M, Oliver Findl, François Malecaze, et al. (2015) Evaluation of the efficacy and safety of a standardised intracameral combination of mydriatics and anaesthetics for cataract surgery. British Journal of Ophthalmology.
- Behndig A, Korobelnik JF (2015) Mydriatic insert and intracameral injections compared with mydriatic eyedrops in cataract surgery: Controlled studies. J Cataract Refract Surg 41: 1503-1519.
- Wilhelm H (2011) Disorders of the pupil. Handb Clin Neurol 102: 427-466.
- Lei HL, Yang KJ, Sun CC, et al. (2011) Obtained mydriasis in long-term type 2 diabetic patients. J Ocul Pharmacol Ther 27: 599-602.
- Manvikar S, Allen D (2006) Cataract surgery management in patients taking tamsulosin staged approach. J Cataract Refract Surg 32: 1611-1614.
- Lorente R, de Rojas V, Vázquez de Parga P, et al. (2012) Intracameral phenylephrine 1.5% for prophylaxis against intraoperative floppy iris syndrome: prospective, randomized fellow eye study. Ophthalmology 119: 2053-2058.
- (2015) Mydrane-summary of product characteristics.
- Lundberg B, Behndig A (2007) Intracameral mydriatics in phacoemulsification surgery obviate the need for epinephrine irrigation. Acta Ophthalmol Scand 85: 546-550.
Corresponding Author
Chetan K Patel, FRCOphth, Department of Ophthalmology , Bishops Wood Hospital, Northwood, Middlesex; Oxford Eye Hospital, John Radcliffe Hospital, Oxford, UK.
Copyright
© 2017 Jai-Hin P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.