Pediatric Elbow Arthrofibrosis: Management and Surgical Considerations
Abstract
A 17-year-old female presented with severe joint contracture secondary to arthrofibrosis of the elbow after mild trauma. Conclusion: Intensive physical therapy, arthroscopic synovectomy and repeated manipulation under anesthesia can return functional range of motion to pediatric patients presenting with refractory arthrofibrosis.
Introduction
Joint contracture of the elbow is not an uncommon finding. Traumatic insults to the elbow as well as surgical manipulation followed by immobilization can lead to arthrofibrosis [1]. However, several cases of mild elbow insult resulting in severe elbow contracture have been reported in the literature [2,3]. This phenomenon, when the level of trauma does not match the subsequent elbow stiffness and there are repeated early recurrences after soft-tissue contracture release, has been coined "refractory arthrofibrosis" [2]. To the best of the authors' knowledge, this case report presents the first instance of refractory arthrofibrosis after mild elbow trauma in the pediatric population.
Case
A 17-year-old female presented to our institution with right arm pain between the wrist and elbow following a fall while cheerleading. She fell forward with her shoulder and elbow flexed in front of her body. Her initial physical exam revealed severe pain over her right lateral epicondyle on palpation with no active block to pronation/supination, however, her ROM was limited to 45-110° extension/flexion. Neurovascular/sensation status was intact and checked in the axillary, common radial, ulnar and median nerve distributions. A palpable radial artery was noted. The patient's fingers were well perfused with normal capillary refill and no swelling or signs of compartment syndrome were observed.
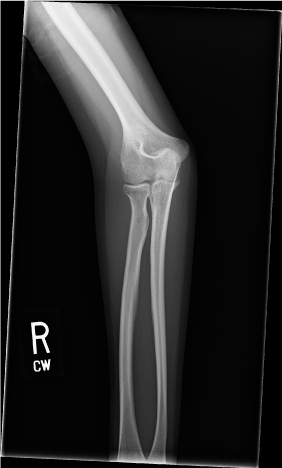
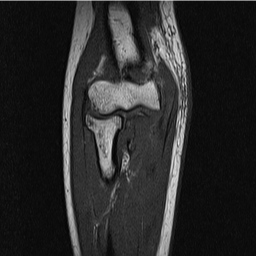
Radiographs performed 3 days after the fall were unremarkable (Figure 1), and the patient was subsequently scheduled for ultrasound. The anterior elbow was evaluated in the long and short axis. Overall, only a small humero-ulnar joint effusion was observed. Given the flexion block and effusion a decision was made for further MRI evaluation, and the patient was placed into a long arm splint with sling for comfort. MRI revealed a non-displaced fracture of the right radial head with straining of the common extensor and pronator teres tendons (Figure 2). The patient was put into a long arm sling, advised to use NSAIDs for pain and was referred to physical therapy for ROM exercises.
Follow up at 6 weeks revealed decreased pain with elbow flexion, extension and protonation, however, significant contracture interfered with her daily activities. Despite formal physical therapy, ROM in her right elbow was limited to 35-128° extension/flexion. The observed stiffness was thought secondary to arthrofibrosis. The patient's medical history was examined thoroughly and was unremarkable for any known inflammatory or metabolic conditions. Furthermore, medical records obtained from the patient's pediatrician revealed no underlying psychiatric or mood disorders that may complicate treatment and compliance in the adolescent population. She was then referred to our department for surgical consultation. Further physical exam revealed limited range of motion and decreased grip strength (right hand: 19 lbs compared to left hand: 40 lbs) and a DASH score of 56.8% in her right upper extremity. The patient and family felt that progress with physical therapy had plateaued, and they decided to proceed with elbow arthroscopy with synovectomy and manipulation under anesthesia.
At four weeks post-op the AROM of her right elbow was 20-53° extension/flexion despite achieving full ROM intraoperatively. Her DASH increased to 62.9% and her right grip strength decreased to 7 lbs. Due to the lack of progression with post-op physical therapy a subsequent manipulation of the elbow under anesthesia was performed. The patient's ROM increased to 20-120° extension/flexion and has remained stable for approximately 1 year. The pain has stopped, and she has regained the ability to brush her hair and eat using her right hand.
Surgical Treatment
The patient received supraclavicular nerve blocks preoperatively and was placed supine on the operating table in a lateral decubitus position. All bony prominences were padded, and the right upper extremity was prepped and draped in sterile fashion. A tourniquet was applied, the affected joint was insufflated with 40 mL of lactated Ringer solution, and an anteromedial portal was made 1.5 cm proximal to the medial epicondyle. Sharp dissection was carried through the skin followed by blunt dissection. The elbow was then entered with a 1.9 mm scope. Upon inspection, the patient had extensive synovitis in the anterior compartment. Next, a standard anterolateral portal was created. Of note, a singular, small chondral loose body was removed from the anterior compartment of the elbow. Next, the synovitis and anterior capsule were carefully removed using a debrider. A cartilage defect on the superior portion of the capitellum with a stable articular rim was observed. After synovectomy of the anterior capsule was completed, a transtricipital portal was made 1 cm proximal to the tip of the olecranon. Blunt dissection was carried down into the olecranon fossa, and a scope was introduced into the radiocapitellar joint. Extensive synovitis and scar tissue were observed in the posterior hemijoint of the elbow. Once a paratricipital portal was made at the level of the radial capitellar joint, a debrider was introduced into the posterior compartment to perform a limited synovectomy. Attention was paid to preserve the annular ligament and triceps. All synovitis was removed from the joint, and no loose bodies or osteochondral defects of the posterior capitellum or radial head were observed. At this point, the elbow was flexed intraoperatively. Full ROM was achieved, and the portals were closed with 3-0 Monocryl. A soft dressing and anterior flexion block splint was applied. The patient was instructed to begin immediate ROM exercises along with physical therapy.
Subsequent manipulations of the elbow were performed under supraclavicular nerve block. Full ROM of the elbow was achieved intraoperatively. Fluoroscopy was used to confirm no fracture occurred during manipulation. The patient was instructed to resume physical therapy 3 days after surgery, specifically, low load prolonged stretch, contract relax stretching, and active and passive assistive ROM exercises with overpressure.
Discussion
In summary, the patient originally presented to our institution with a ROM of 45-110° extension/flexion. After 6 weeks of conservative treatment and physical therapy, her ROM plateaued at 35-128 ° extension/flexion. An elbow arthroscopy with synovectomy was then performed. Despite achieving full ROM intraoperatively, the patient's ROM at 4 weeks post-op decreased to 20-53° extension/flexion. A subsequent manipulation under anesthesia increased the patient's ROM to 20-120° extension/flexion where it has remained stable for over 1 year.
After a mild insult like a non-displaced fracture an unexplainable elbow contracture is rare in the pediatric patient, and as such, this is the first case report that presents such an event. Nonetheless, refractory arthrofibrosis should only be suspected in a similar situation if all other potential etiologies of stiffness are ruled out including intrinsic causes (i.e. joint incongruity, synovitis, malunion, loose bodies, and post-traumatic osteophyte formation) and extrinsic causes (i.e. heterotopic ossification, adhesions, contractures of the joint capsule, and ligament contractures) [4].
In addition to standard X-ray imaging, MRI may be needed to identify chondral damage and loose bodies. For example, Hear, et al. presented a case of elbow stiffness in a 10-year-old boy following a non-displaced supracondylar fracture; the stiffness was corrected once a previously unseen articular cartilage fragment was removed from the radiocapitellar joint [3]. In the case presented, MRI was performed and no loose bodies were observed. However, a small chondral fragment was found and removed from the anterior compartment during arthroscopy. Unfortunately, removal of the loose body did not relieve the patient's contracture which further supported the hypothesis of refractory arthrofibrosis.
Even if identification of refractory arthrofibrosis is made, as the name suggests, response to treatment does not offer complete resolution. While the patient described here regained functional status and was able to return to activities of daily living, ROM returned to borderline functional range with a continued flexion block despite aggressive physical therapy and multiple procedures. Nesterenko, et al. reported on four adults suffering from refractory arthrofibrosis and found that, despite similar surgical treatment and manipulation under anesthesia, any gains in ROM were lost within 2 months [2]. Nesterenko, et al. reported post-treatment average ROM of 38-83° extension/flexion accompanied by pain, while the patient presented here has an ROM arc of 20-120° extension/flexion that has remained stable for over one year.
Fibrotic scar tissue formation is not an uncommon response to severe trauma and surgery, and arthrofibrosis is a known complication after total knee arthroplasty. It can also be seen after prolonged immobilization of a joint [5]. However, the patient in this case report did not suffer a significant trauma nor was she exposed to prolonged immobilization. As genetics and bioinformatics advance, the etiology of arthrofibrosis is becoming less murky. Excessive scar tissue production has been linked to a pro-inflammatory response with increased amounts of IL-2, IL-6 and tumor necrosis factor alpha resulting in increased levels of alpha-smooth muscle actin containing myofibroblasts in the setting of arthrofibrosis [6-8]. However, recent studies utilizing microarray expression and RT-qPCR have begun to identify upregulated mRNA transcription of genes affecting pathways linked to inflammation, ECM synthesis, and remodeling in the early stages of in-vivo joint contracture models [9]. Further elucidation of these molecular targets may provide a genetic basis as to why certain patients may be predisposed to refractory arthrofibrosis [9]. Until then, pediatric patients with suspected refractory arthrofibrosis should be followed diligently, enrolled in a robust physical therapy program, and synovectomy and manipulation should be performed judiciously by the treating surgeon.
References
- Barlow JD, Hartzler RU, Abdel MP, et al. (2013) Surgical capsular release reduces flexion contracture in a rabbit model of arthrofibrosis. J Orthop Res 31: 1529-1532.
- Nesterenko S, Sanchez-Sotelo J, Morrey BF (2009) Refractory Elbow Arthrofibrosis: A Report of Four Cases. J Bone Joint Surg Am 91.
- Heard WMR, O'Brien MJ, Savoie FH (2015) Elbow Trauma and Arthrofibrosis. In: Brockmeier SF, MRI-Arthroscopy Correlations: A Case-Based Atlas of the Knee, Shoulder, Elbow and Hip. Springer New York, New York, USA, 327-333.
- Nandi S, Maschke S, Evans PJ, et al. (2009) The stiff elbow. Hand (NY) 4: 368-379.
- Dafang Zhang, Ara Nazarian, Edward K Rodriguez (2018) Post-Traumatic Elbow Stiffness: Pathogenesis and Current Treatments. Shoulder & Elbow.
- Abdel MP, Morrey ME, Barlow JD, et al. (2012) Myofibroblast cells are preferentially expressed early in a rabbit model of joint contracture. J Orthop Res 30: 713-719.
- Cohen MS, Schimmel DR, Masuda K, et al. (2007) Structural and biochemical evaluation of the elbow capsule after trauma. J Shoulder Elbow Surg 16: 484-490.
- Unterhauser FN, Bosch U, Zeichen J, et al. (2004) α-Smooth muscle actin containing contractile fibroblastic cells in human knee arthrofibrosis tissue. Arch Orthop Trauma Surg 124: 585.
- Morrey ME, Abdel MP, Riester SM, et al. (2017) Molecular landscape of arthrofibrosis: Microarray and bioinformatic analysis of the temporal expression of 380 genes during contracture genesis. Gene 610: 15-23.
Corresponding Author
Mark Seeley, Department of Orthopaedic Surgery, Geisinger Medical Center, Danville, Pennsylvania, USA.
Copyright
© 2019 Max C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.