Small Bowel Diverticula: Usefulness of the Computed Tomography in a Non-Specific Clinical Presentation
Abstract
In the majority of cases small bowel diverticula are asymptomatic. As a result, the diagnosis is frequently incidentally made either by radiographic examination or upon laparotomy due to complications. Enteroclysis, Tc-99m scintigraphy, video capsule and double balloon enteroscopy are useful diagnosing small bowel disorders, but their utility in emergency situations is limited.
The clinical data from three consecutive patients surgically treated in our hospital for acute complications related to small bowel diverticula were retrospectively analyzed.
Small Bowel Diverticula are a rare pathology and the clinical presentation is usually non-specific, even with acute or chronic complications. Some diagnostic examinations such as X-ray and ultrasound scan could not be useful to verify the existence of the pathology even in acute presentation but, in our experience, the computed tomography of the abdomen is the most helpful examination in localizing the disease and guiding the appropriate approach even when it doesn't suspect a definite diagnosis. CT findings are able to bring to a correct pre-operative evaluation in presence of intestinal perforation, necessary to plan patient management.
Keywords
Jejunal-ileal diverticula, Clinical presentation, Computed tomography, Perforated diverticula
Introduction
Although diverticular disease of the duodenum and colon is frequent, the jejuno-ileal diverticulosis is an uncommon entity [1]. The prevalence of Small Bowel Diverticula (SBD) on autopsy ranges from 0.06% to 4.6% [2-5] and to 2.3% in radiographic findings [6]. The prevalence increases with age, peaking at the sixth and seventh decades. Eighty percent of diverticula occur in the jejunum, 15% in the ileum and 5% in both [6,7]. It is documented that the higher incidence of SBD in the jejunum is attributed to the larger diameters of the penetrating jejunal arteries [8].
In the majority of cases small bowel diverticula are asymptomatic [9]. As a result, the diagnosis is frequently incidentally made either by radiographic examination or upon laparotomy due to complications [6]. However, this entity should not be dismissed as an incidental finding, because it may be the cause of unclear chronic non-specific abdominal symptoms and acute complications, including hemorrhage, intestinal obstruction, diverticulitis and perforation. Owing to the rarity of these lesions and their complications, diagnosis is often difficult and delayed [9] and mortality of these complications reaches a rate as high as 24% [6]. In particular, the perforation of the small bowel diverticula can be fatal due to the delay in diagnosis [1] as the clinical presentation is often confused with other more common abdominal inflammatory processes. Plain abdominal radiographs are performed routinely but in most cases are not sufficient for diagnosis [7]. Enteroclysis, Tc-99 m scintigraphy, video capsule and double balloon enteroscopy are useful diagnosing small bowel disorders [10], but their utility in emergency situations is limited. The abdominal Computed Tomography (CT) may identify thickening or inflammation of the jejunum [11] but it also diagnoses isolated extraluminal air bubble in the mesentery that results from perforated diverticula or may visualize localized inflammatory masses such as a large abscess. Moreover, in the absence of contra-indications, diagnostic laparoscopy is very useful in evaluating patients with a complicated course. It ensures an accurate diagnosis and avoids the risk of unnecessary laparotomy if not indicated [6].
We report the clinical presentation of three patients with perforation related to small bowel diverticulosis, diagnosed and treated in our institution along with the accompanying diagnostic issues and a review of the literature. The aim of the study, even though with the due limit of three cases, is underline as CT is an accurate tool in predicting the site of gastro-intestinal perforation, especially in presence of clinical signs that could be considered subtle or only indirectly related to the site of perforation.
Cases Presentation
The clinical data from three consecutive patients surgically treated in San Gerardo Hospital (Monza, Italy) for acute complications related to small bowel diverticula were retrospectively analyzed (Table 1): they were two women and one man, with a mean age of 64.7 years (range 58-70 years). Patients with Meckel’s diverticulum or duodenal diverticulum were not included.
The first patient was a woman: she presented at the emergency room with abdominal pain at the upper quadrants for one month and some days of fever, urinary disorders and vomit, but with no clinical evidence of peritonitis. According to the initial symptoms the general practitioner prescribed a therapy with Ciprofloxacin for two weeks in the suspect of a urinary tract infection, with no benefit, and the persistence and exacerbation of symptoms had led the patient to our observation. Her medical history showed a surgical removal of an uterine leiomyomas and one right salpingo-ophrectomy.
The second patient was a man: he presented with fever, nausea, abdominal pain from two week, with a negative rebound tenderness sign (Blumberg). He reported a regular bowel function and a light diet for few days because of the nausea. In anamnesis we detected angina pectoris, arterial hypertension and a chronic obstructive pulmonary disorder.
The third patient was a woman: she presented at the fifth day of abdominal distention and pain, specifically at the left iliac fossa, with no vomit and no fever, but only constipation and the evidence of a decreased peristalsis. She only underwent a C-section in her life.
Every one of them presented to the emergency department with generalized abdominal pain and only the first patient had a clinic presentation that could suggest a particular disease such as a pyelonephritis.
The computerized tomography (Philips Brilliance iCT 256-slice scanner) was used as a diagnostic instrument for every one of them: the three patients had acute complications due to jejunal-ileal perforation of the diverticula.
Results
The main complaint of all these patients was abdominal pain, with fever and no evidence of peritonitis (Blumberg’s sign) and instrumental signs of bowel occlusion. In one case, this pain was interpreted as pyelonephritis at first time.
Every patient had a neutrophilic leukocytosis and an increased value of the C-reactive protein, but they did not have high blood values of Creatine kinase or Lactate (Table 1).
They all underwent X-ray (RX) examinations of the abdomen, but they did not show any evidence of free air and bowel occlusion and wasn’t helpful to complete the diagnosis. So every patient underwent an Ultrasound Scan (US), but there wasn't evidence of fluid collections or parietal thickenings of intestinal loops in any patient, only in patient 1 the ultrasound examination seemed to suggest a framework of pyelonephritis.
At that point they underwent CT examinations that, in all cases, identified the diverticular out pouching and the related inflammation. The abdominal CT was able to identify the presence of small bowel perforation in two cases: the two perforated diverticula were located in the jejunum on the mesenteric border, measuring between 20 and 31mm in diameter, and the diverticula were multiple in two patients.
In particular in patient 1 the CT scan showed a single jejunal diverticulum of 2 × 2.5 × 2.7 cm with proximal parietal thickening, lymph nodes reactivity and a very small fluid collection. In patient 2, the CT scan was carried out because of a clinical suspect of diverticulitis; the investigation identified a thickening of an jejunal loop in the context of numerous diverticula, where the biggest had a diameter of 31 mm. Heterogeneity of perivisceral fat and lymph nodes reactivity with an area of perforation stopped up with a sigmoid epiploic appendix and presence of purulent material were also found. In patient 3, the CT scan showed the presence of a small bowel diverticulum (diameter: 28 mm) with inflammation of perifocal fat and moderate fluid collection in the pelvis. Other diverticula were found at the proximal ileus.
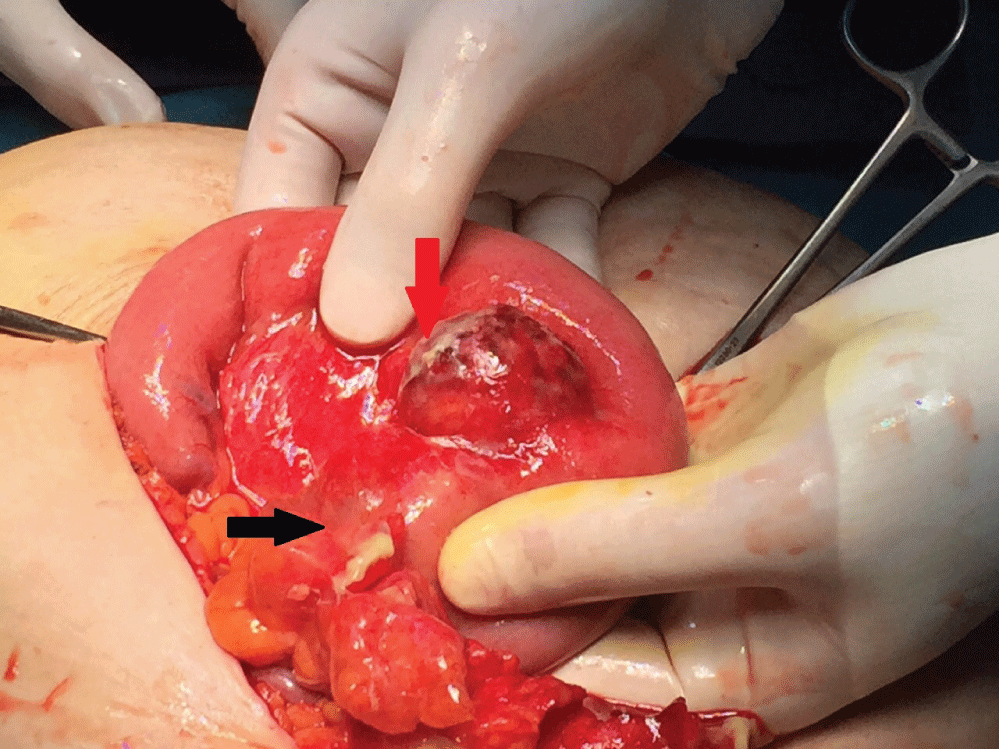
All patients underwent an exploratory laparoscopy; in patient 3 laparoscopic surgery was not possible due to the presence of adhesions from the previous C-section and the severe inflammatory process, so the surgical operation was converted to a median laparotomy: Figure 1 shows the perforated diverticulum plugged by the omentum.
One patient had a single diverticulum, while the others had multiple SBD of the proximal and middle portions of the ileum. Resection of the involved jejunal and ileus segment with primary anastomosis was performed in all three patients, with lysis of adhesions where needed, and for all patients a tissue sample of the perforated diverticula were pathologically analyzed. A cultural examination of the free abdominal fluid was made in two patients.
The final histological studies evidenced a diverticular disease in all patients, with acute necrotizing inflammation of the diverticular perimeter (patient 1), chronic granulomatous inflammation with abscesses (patient 2) or inflammation with abscesses and acute perforated diverticulitis (patient 3).
After the surgical intervention we placed an abdominal drain, which was removed two days later. There were no post-surgery complications, all subjects are still alive and have been discharged from hospital after a mean time of 6.7 days (range 6-7 days).
Discussion
The SBD disease is rare and it is usually asymptomatic, but it can present as an emergency: complications include intestinal obstruction, bleeding, inflammation and perforation, but also malabsorption, enterolith formation and abdominal discomfort [10]. Other possible, but still rarer, complications are the obstructions of the biliary or pancreatic duct and blind loop syndrome [12]. They occur in 10-30% of cases and they require surgical interventions in 8-30% of patients [13-15]. Some authors reported that it was not necessary to perform resection for ileal diverticula which were incidentally founded at laparotomy [16], but other authors favor surgical intervention, especially for large diverticula with dilated bowel loops that suggests a progressive form of the disease, and they reported good results for resections performed on patients with chronic pain or malabsorption [10,16].
The diagnosis of small bowel diverticulosis has therefore significant implications for the management of symptomatic patients, but this condition, well recognized on barium studies [17,18], have been anecdotal descriptions on abdominal CT [19]. The difficulty in detecting SBD on CT is probably related to a combination of factors including a thin criteria used to differentiate diverticula from gas or fluid-filled loops of small bowel as well as being an uncommon cause of symptoms in some cases the radiologist are not able to direct their attention to this pathology [20]. CT images in coronal or sagittal planes may be especially helpful in differentiating dilated small bowel loops from SBD. Some studies suggested that diverticula greater than 3 centimeters can be recognized to CT by the adjacent small bowel loops from their different contents and by the absence of discernible valvulae conniventes [21].
Beyond the diagnostic difficulty some CT findings can be considered characteristic of SBD; they appear as discrete round or ovoid, contrast-, fluid-, or air-containing structures outside the expected lumen of the small bowel, with a smooth wall and no recognizable small bowel folds [20].
In the small bowel diverticulitis common CT findings are a focal area of asymmetric small bowel wall thickening at the site of a focal out-pouching on the mesenteric side of the bowel; the absence of pneumoperitoneum does not exclude perforation [22]. Findings such as focal defect in the bowel wall, segmental bowel-wall thickening and concentrated bubbles of extraluminal gas in close proximity to the bowel wall have a high predictive value indicating the site of perforation [23].
In our experience we found there are not specific clinic data in patients with SBD: they have abdomen pain, fever and vomit from many days. Their blood exams are not specifically guiding to a single diagnosis, but they underline the presence of pathology.
Starting from their clinical presentation, without a clear indication to a surgical intervention, we treated our patients with antibiotics (Table 1), but the long-term presence of the symptoms and the ineffectiveness of the medical therapy after 24-48 hours orientated us to the need of a more specific diagnosis. RX and US tests did not highlight any evidence and the persistence of the symptoms with the incapability to reach a definite diagnosis directed to submit the patients to abdominal CT examinations. According only to their clinic presentation two exams were not indicated, but they were helpful in every case to reach a correct surgical management.
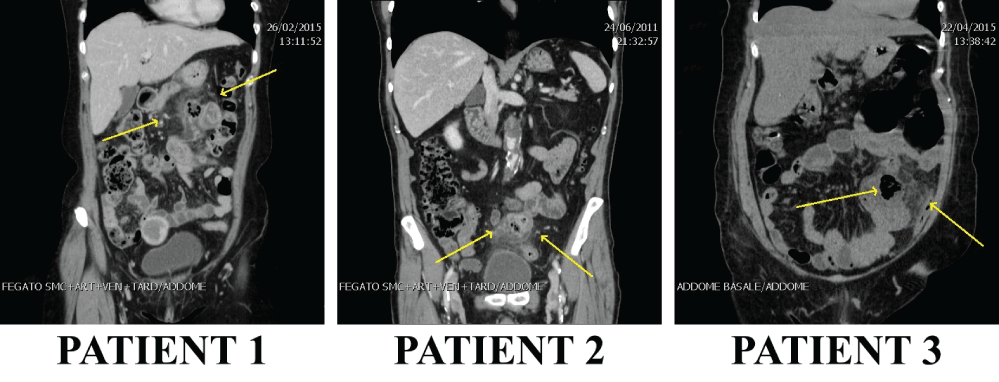
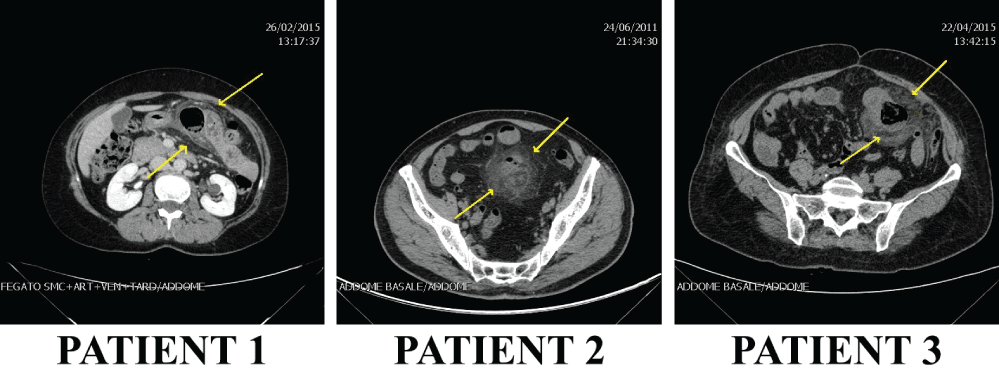
CT images (Figure 2 and Figure 3) highlighted the locations, number and dimensions of the diverticula: these examinations helped to prepare the right surgical interventions, according to the specific pathologic situation of every single patient. They were essential to proceed with the laparoscopies as they confirmed the presence of the diverticula, concluding the diagnostic process and guiding the surgeons through the interventions.
Conclusion
SBD have non specific and insidious course and its delayed diagnosis can lead to internal loop abscess or perforation, a favorable prognosis can be expected by an early diagnosis. CT of the abdomen play a crucial role in the diagnosis of small bowel diverticulitis and it is the most helpful exam to find the location of SBD and to guide to the most appropriate approach, even when there is not a diagnostic suspect.
Conflicts of Interest
None to declare.
Authors’ Contribution
F.U. and P.A.R. designed and wrote the report; I.S. and E.P. collected literature data; L.G. and F.R. reviewed the manuscript for its intellectual content. All authors read and approved the final version of the manuscript.
References
- Kassir R, Boueil-Bourlier A, Baccot S, et al. (2015) Jejuno-ileal diverticulitis: Etiopathogenicity, diagnosis and management. Int J Surg Case Rep 10: 151-153.
- Singal R, Gupta S, Airon A (2012) Giant and multiple jejunal diverticula presenting as peritonitis a significant challenging disorder. J Med Life 5: 308-310.
- Kassahun WT, Fangmann J, Harms J, et al. (2007) Complicated small-bowel diverticulosis: a case report and review of the literature. World J Gastroenterol 13: 2240-2242.
- Chien-Hua Lin, Huan-Fa Hsieh, Chih-Yung Yu, et al. (2005) Diverticulosis of the jejunum with intestinal obstruction: A case report. World J Gastroenterol 11: 5416-5417.
- Makris K, Tsiotos GG, Stafyla V, et al. (2009) Small intestinal nonmeckelian diverticulosis. J Clin Gastroenterol 43: 201-207.
- Hibbeln JF, Gorodetsky AA, Wilbur AC (1995) Perforated jejunal diverticulum: CT diagnosis. Abdom Imaging 20: 29-30.
- Tsiotos GG, Farnell MB, Ilstrup DM (1994) Nonmeckelian jejunal or ileal diverticulosis: an analysis of 112 cases. Surgery 116: 726-731.
- Lempinen M, Salmela K, Kemppainen E (2004) Jejunal diverticulosis: a potentially dangerous entity. Scand J Gastroenterol 39: 905-909.
- Dimitris Mantas, Stylianos Kykalos, Dimitris Patsouras, et al. (2011) Small intestine diverticula: Is there anything new? World J Gastrointest Surg 3: 49-53.
- Sakpal SV, Fried K, Chamberlain RS (2010) Jejunal Diverticulitis: A Rare Case of Severe Peritonitis. Case Rep Gastroenterol 4: 492-497.
- Schnueriger B, Vorburger SA, Banz VM, et al. (2008) Diagnosis and management of the symptomatic duodenal diverticulum: a case series and a short review of the literature. J Gastrointest Surg 12: 1571-1576.
- Affes Nejmeddine, Abid Bassem, Hammami Mohamed, et al. (2009) Complicated jejunal diverticulosis: Acase report with literature review. N Am J Med Sci 1: 196-199.
- Falidas E, Vlachos K, Mathioulakis S, et al. (2011) Multiple giant diverticula of the jejunum causing intestinal obstruction: report of a case and review of the literature. World J Emerg Surg 6: 8.
- Alok Tiwari, Vijay Gupta, Priya Hazrah, et al. (2013) A rare case of multiple jejunal diverticulosis presenting as intestinal obstruction. Clin Pract 3: e21.
- Longo WE, Vernava AM 3rd (1992) Clinical implications of jejunoileal diverticular disease. Dis Colon Rectum 35: 381-388.
- Wilcox RD, Shatney CH (1988) Surgical implications of jejunal diverticula. South Med J 81: 1386-1391.
- Maglinte DD, Chernish SM, DeWeese R, et al. (1986) Acquired jejunoileal diverticular disease: subject review. Radiology 158: 577-580.
- Herlinger H, Maglinte D, Birnbaum BA (1999) Clinical imaging of the small intestine. Springer-Verlag 331-376.
- Horton KM, Corl FM, Fishman EK (1999) CT of non-neoplastic diseases of the small bowel : spectrum of disease. J Comput Assist Tomogr 23: 417-428.
- Fintelmann F, Levine MS, Rubesin SE (2008) Jejunal diverticulosis: findings on CT in 28 patients. AJR Am J Roentgenol 190: 1286-1290.
- Chou CK, Mak CW, Hou CC, et al. (1998) CT of large small-bowel diverticulum. Abdom Imaging 23: 132-134.
- Macari M, Faust M, Liang H, et al. (2007) CT of jejunal diverticulitis: imaging findings, differential diagnosis, and clinical management. Clin Radiol 62: 73-77.
- JP Singh, MJ Steward, TC Booth (2010) Evolution of imaging for abdominal perforation. Ann R Coll Surg Engl 92: 182-188.
Corresponding Author
Fabio Uggeri, Department of Medicine and Surgery, University of Milano-Bicocca, via Cadore 48, 20900 Monza (MB), Italy, Tel: +39-347-4311-545, +39-0392-333-651.
Copyright
© 2017 Uggeri F, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.