An Uncommon Cause of a Refractory Gastric Ulcer
Keywords
Eosinophilic gastroenteritis, Abdominal pain, Gastric ulcer, Helicobacter pylori
Case Discussion
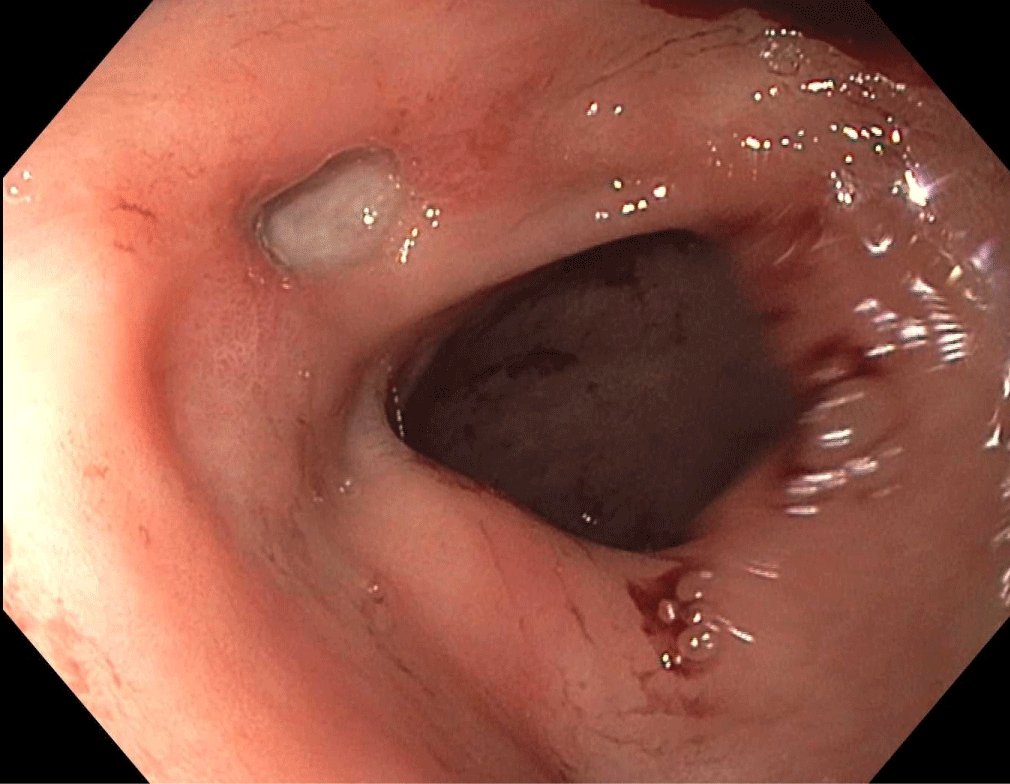
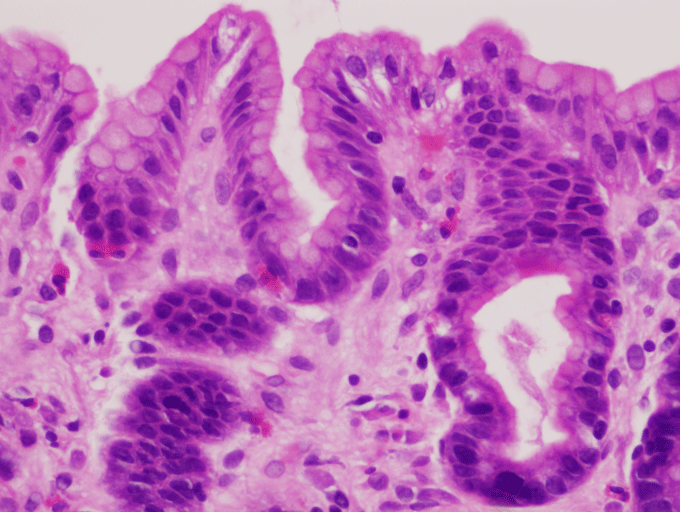
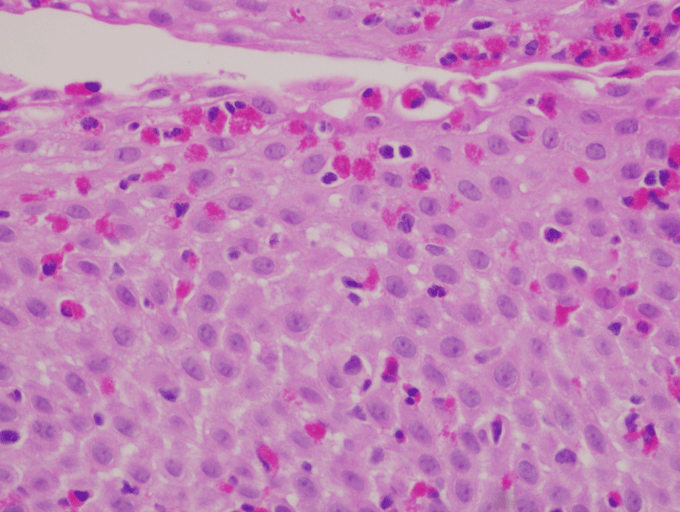
A 29-year-old female with a history of bipolar disorder presented to the emergency department (ED) with worsening epigastric pain. Two years ago, esophagogastroduodenoscopy (EGD) showed a 1.5-cm benign-appearing superficial ulcer in the pylorus. She was presumed to have an NSAID-induced peptic ulcer and was treated with proton pump inhibitor therapy. She had multiple hospitalizations for abdominal pain and several subsequent EGDs showing refractory gastric ulcer. During each EGD, the ulcer appeared deepen. Stool antigen and antral biopsy for H. pylori test (histology and rapid urease test) were repeatedly negative with normal gastrin level. Her physical examination was unremarkable. Complete blood count showed a hemoglobin of 11.4 g/dl (11.5-15.5) and white blood cell of 11.5 K/cm2 (4-12) with 5% eosinophils. The patient underwent repeat EGD that showed deeper ulcer (Figure 1). Targeted biopsies from the margin of the ulcer and esophagus showed significant eosinophilic infiltration consistent with primary eosinophilic gastroenteritis (EGE) (Figure 2 and Figure 3). She was started on prednisone 20 mg daily. Follow-up EGD after six weeks of prednisone showed completely healed ulcer and gastric biopsy showed improved eosinophil infiltration of 10 cells/HPF. The patient was seen follow up three and six months later showed complete resolution of symptoms with improvement in the quality of life.
Refractory gastric ulcer typically generates a broad list of differential diagnoses. Poor compliance with proton-pump inhibitors (PPIs), perpetual use of NSAIDs and H. Pylori should be considered as an initial differential diagnosis [1]. Other diagnostic possibilities including sarcoidosis, EGE, infection, and cancer should be investigated by performing biopsy from four quadrants of the ulcer. Peripheral eosinophilia and elevated serum immunoglobulin E (IgE) are common but not universal [2]. The pathogenic mechanism of EGE is not well recognized. Cytokines such as interleukin (IL)-3, IL-5 and granulocyte macrophage colony stimulating factor (GMCSF) causing the recruitment and activation of eosinophils [2,3]. Also, eotaxin has been shown to recruiting eosinophils into the lamina propria of the stomach and leading to inflammation and damage [2,4].
Klein classified EGE into three types depending on the layer in which inflammation takes place: Mucosal, muscular, and serosal type [4]. EGE usually present with nonspecific GI symptoms; the refractory gastric ulcer is a rare presentation of EGE [5]. Even though atopic disease and eosinophilia are clues to the diagnosis, the biopsy is crucial. The systemic steroid is very effective and results in complete resolution of symptoms; however, the patients who relapse after discontinuation of steroid may require long-term, maintenance therapy with a low-dose steroid.
Authors' Disclosures of Potential Conflicts of Interest
The author(s) indicated no potential conflicts of interest.
Financial Disclosure
None to report.
Authors' Contribution
All authors contributed equally to this manuscript.
References
- Lanas AI, Remacha B, Esteva F, et al. (1995) Risk factors associated with refractory peptic ulcers. Gastroenterology 109: 1124-1133.
- Ingle SB, Hinge Ingle CR (2013) Eosinophilic gastroenteritis: An unusual type of gastroenteritis. World J Gastroenterol 19: 5061-5066.
- Desreumaux P, Bloget F, Seguy D, et al. (1996) Interleukin 3, granulocyte-macrophage colony-stimulating factor, and interleukin 5 in eosinophilic gastroenteritis. Gastroenterology 110: 768-774.
- Talley NJ, Shorter R, Phillips S, et al. (1990) Eosinophilic gastroenteritis: A clinicopathological study of patients with disease of the mucosa, muscle layer, and subserosal tissues. Gut 31: 54-58.
- Kristopaitis T, Neghme C, Yong SL, et al. (1997) Giant antral ulcer: A rare presentation of eosinophilic gastroenteritis--case report and review of the literature. Am J Gastroenterol 92: 1205-1208.
Corresponding Author
Jiten P Kothadia, MD, Nazih Zuhdi Transplant Institute, INTEGRIS Baptist Medical Center, 3300 NW Expressway, Oklahoma City, OK 73112, USA, Tel: 609-865-6418, Fax: 405-951-9860.
Copyright
© 2018 Kothadia JP, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.