Pill-Induced Esophagitis with Mucosal Dissection: A Case Report
Background
Pill-induced esophageal injury was first described in 1970. It occurs when a caustic medicinal pill dissolves in the esophagus and releases its noxious content, particularly if transit is delayed. Injury of this type, called pill esophagitis or pill induced esophageal injury is common but unfortunately is under-reported. More than a hundred different medicines have been reported to cause esophageal injury [1].
This injury is a common cause of esophageal complaints such as severe odynophagia, dysphagia, bleeding and even perforation. History and endoscopic examination are very important in diagnosis, and early endoscopic exam in particular may prevent these severe complications [2].
The quantity of pills taken has not been correlated with esophagitis. The likelihood of injury is related to the specific pills that are taken, the more caustic pills and the posture in which the patient habitually takes them, as well as whether or not they take a significant amount of water with them [3].
We report a case of a patient who presented pill esophagitis while under a treatment with naproxen.
Case Report
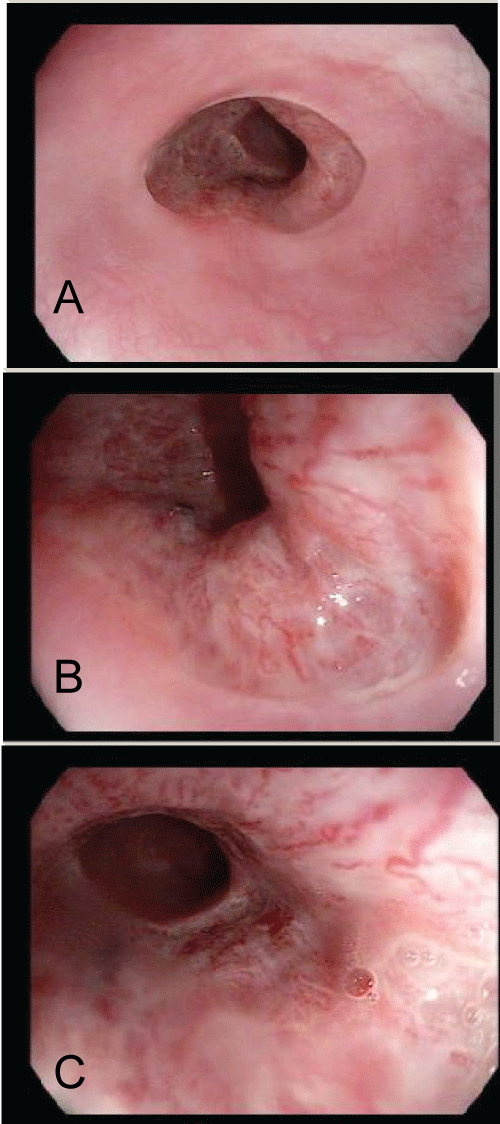
A 56-year-old female patient with dyslipidemia, type-2 diabetes and osteoarthritis was referred to our hospital with complaints of epigastric and retrosternal pain of high intensity, associated with intense heartburn, dysphagia and a sore throat sensation. She reported onset of symptoms 2 months before, after using naproxen twice a day for joint pain caused by osteoarthritis for about 40 days. She reported taking the pills usually with a small amount of water. A cardiologist had already evaluated her with no changes in electrocardiogram and stress test. No other abnormalities could be found in the history, thoracic radiography, hematology, biochemistry. Esophagogastroduodenoscopy was promptly performed and revealed a normal esophageal mucosa up to 30 cm from the incisors where there was a circumferential deepithelialized area with approximately 2 cm in length (Figure 1a, Figure 1b and Figure 1c). The other endoscopic findings were normal.
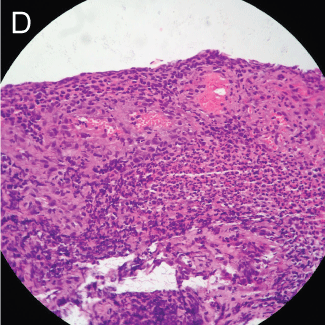
The histopathological study showed an ulcer fund compatible with chronic ulcerated esophagitis with no epithelial representation in the sample (Figure 1d).
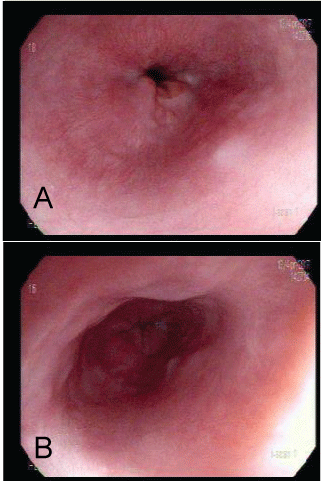
Patient was treated with pantoprazole 40 mg twice a day during 4 weeks with significant improvement of symptoms. A new endoscopic examination was performed after that and revealed a normal esophagus with a slight scar at 32 cm from the incisors (Figure 2).
Discussion
Our patient initially presented symptoms compatible with reflux esophagitis, such as heartburn sensation, but later developed high-intensity retrosternal pain and dysphagia, which subsequently correlated with the atypical endoscopic findings of circumferential ulcer with deepithelialization of the mid-esophagus confirmed in the histological examination.
The most frequently affected site in pill esophagitis was presumed to be in the mid-third of the esophagus. However, pill esophagitis can occur at any level where the esophagus is narrowed: The upper sphincter, the aortic arch, the left main bronchus, and the lower esophageal sphincter [4]. Evidence suggests that the highest incidence of pill esophagitis occurs in the distal, acid exposed region of the esophagus related to concomitant acid reflux, as demonstrated by injury from Nonsteroidal Anti-Inflammatory Drugs (NSAIDs) and other medications. In its distal location, pill esophagitis is often mistaken for reflux esophagitis [5].
The most common medications to cause pill esophagitis are antibiotics as tetracycline, doxycycline and clindamycin due to their direct irritant effect in the esophagus; NSAIDs that can cause severe esophagitis, esophageal strictures and bleeding [6]; bisphosphonates which can cause esophageal ulcers [7,8] and other medications such as potassium chloride, quinidine preparations, iron compounds, emepronium, alprenolol, and pinaverium [9]. Among all the medications used by our patient naproxen was the most likely drug to cause pill esophagitis. Pill-induced esophagitis occurs mainly in patients with risk factors for delayed esophageal clearance, causing prolonged contact of the medication with the esophageal mucosa [9,10] which can cause a local acid burn (doxycycline, tetracycline, ascorbic acid, ferrous sulfate, and emepronium) [11], local hyperosmolality when hyperosmotic solutions as potassium chloride generate tissue destruction and vascular injury [12] or, as in the case of our patient disruption of the cytoprotective barrier induced by NSAIDs.
The typical endoscopic appearance of pill-induced esophageal injury is a discrete ulcer with relatively normal surrounding mucosa [6]. Ulcers may range in size from 1 or 2 mm to several centimeters. In patients with alendronate-induced esophagitis, ulcerative lesions may involve 10 cm or more of the esophagus [7], although our patient did not report use of bisphosphonate drugs, she presented with a large circumferential ulcer in mid esophagus. Ulcers may be single or multiple and may be surrounded by mild local inflammatory changes. The typical ulcer involves only the submucosa, however deeper degrees of penetration can occur, and localized perforation has been reported [13]. Many cases of esophagitis caused by ibuprofen, indomethacin, aspirin, benorylate naproxen, and phenylbutazone have been reported in the last 10 years. Many of them have developed stricture and a few of them perforation or nonfatal hemorrhage. Before dysphagia occurred, most of the patients who were taking anti-inflammatory drugs - as happened with our patient - had symptoms of gastroesophageal reflux. This advocates that these drugs may aggravate reflux esophagitis and so increase the risk of stricture formation. NSAIDs should be prescribed with caution in the presence of symptomatic gastroesophageal reflux [9].
The main treatment of pill-induced esophagitis includes cessation of the offending drug and supportive therapy [2]. Although the use of antacids, histamine receptor antagonists, proton pump inhibitors, sucralfate, and even local anesthetic agents have been reported, it is unclear if they are effective in treating medication-induced esophagitis. However, it is recommended to use acid suppression as gastroesophageal reflux disease may be exacerbating or perpetuating the injury. Patients should be reminded that any pill, particularly the more caustic ones that have been frequently reported to cause pill-induced esophagitis, should be taken upright, with a full glass of water and not immediately prior to going to bed [3].
References
- Abid S, Mumtaz K, Jafri W, et al. (2005) Pill-induced esophageal injury: Endoscopic features and clinical outcomes. Endoscopy 37: 740-744.
- Büyükberber M, Demirci F, Savas MC, et al. (2006) Pill esophagitis caused by telithromycin: A case report. Turk J Gastroenterol 17: 113-115.
- Kikendall JW (2007) Pill-induced esophagitis. Gastroenterol Hepatol 3: 275-276.
- Kearney DJ, Donald GB (2002) Esophageal disorders caused by infection, systemic illness, medication, radiation and trauma, Pill esophagitis. In: Feldman M, Friedman LS, Sleisenger MH, Sleisenger & Fordtran's gastrointestinal and liver disease. (7th edn), Saunders, Philadelphia, 634-645.
- Vãlean S, Petrescu M, Cãtinean A, et al. (2005) Pill esophagitis: Two case reports. Romanian Journal of Gastroenterology 14: 159-163.
- Kikendall JW, Friedman AC, Oyewole MA, et al. (1983) Pill-induced esophageal injury. Case reports and review of the medical literature. Dig Dis Sci 28: 174-182.
- de Groen PC, Lubbe DF, Hirsch LJ, et al. (1996) Esophagitis associated with the use of alendronate. N Engl J Med 335: 1016-1021.
- Liberman UA, Weiss SR, Bröll J, et al. (1995) Effect of oral alendronate on bone mineral density and the incidence of fractures in postmenopausal osteoporosis. The alendronate phase iii osteoporosis treatment study group. N Engl J Med 333: 1437-1444.
- Zografos GN, Georgiadou D, Thomas D, et al. (2009) Drug-induced esophagitis. Dis Esophagus 22: 633-637.
- Olovson SG, Björkman JA, Ek L, et al. (1983) The ulcerogenic effect on the oesophagus of three beta-adrenoceptor antagonists, investigated in a new porcine oesophagus test model. Acta Pharmacol Toxicol (Copenh) 53: 385-391.
- Carlborg B, Densert O (1980) Esophageal lesions caused by orally administered drugs. An experimental study in the cat. Eur Surg Res 12: 270-282.
- Boley SJ, Allen AC, Schultz L, et al. (1965) Potassium-induced lesions of the small bowel I. Clinical aspects. JAMA 193: 997-1000.
- Henry JG, Shinner JJ, Martino JV, et al. (1983) Fatal esophageal and bronchial artery ulceration caused by solid potassium chloride. Pediatr Cardiol 4: 251-252.
Corresponding Author
Marcelia Brandelli Vieira dos Santos, Serviço de Gastroenterologia e Endoscopia Digestiva do, Hospital Ernesto Dornelles, Porto Alegre, Brazil.
Copyright
© 2017 dos Santos MBV, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.