Type II Myocardial Infarction and Stress Cardiomyopathy Secondary to Inhaled Foreign Body (Garden Pea)
Abstract
A foreign body aspiration is an unusual event in the adult population, outside of known risk factors such as neurological disease. It typically presents as "cough (67%), dyspnoea (28%), chest pain, cyanosis, stridor or obstruction" and "wheezing (12.7%) and haemoptysis (23.3%)".
The authors present the case of inhaled foreign body (pea) in a 69-year-old lady, without underlying risk factors for aspiration. On admission, she was tachypnoeic and unable to speak in full sentences. Her Computerised tomography (CT) scan showed ground-glass changes and potentially superimposed infective changes.
Whilst awaiting transfer for bronchoscopy, she developed severe respiratory distress with cardiovascular compromise (new left bundle branch block (LBBB), tachycardia and hypertension). She was intubated in extremis and commenced on noradrenaline. Her angiogram showed mild non-obstructive disease, and she was diagnosed with a type two myocardial infarction and stress-induced cardiomyopathy. The pea was later removed on intensive care via flexible-bronchoscopy.
Learning points include the potential for patients with a foreign body to acutely deteriorate, hence the need for urgent bronchoscopic removal and the potential to develop myocardial ischaemia secondary to acute respiratory distress.
Keywords
Pulmonary aspiration treatment, Myocardial ischaemia, Bronchoscopy
Abbreviations
CT scan: Computerised tomography scan; LBBB: Left bundle branch block; PEA: Pulse less electrical activity; GCS: Glasgow coma score; TIVA: Total intravenous anaesthesia; ASA: American society of anesthesiologists
Introduction
Although foreign body aspiration is most frequently seen in the childhood age group, it can also be seen in the adult age group too. In adults, foreign bodies have a tendency to lie in the right bronchus as this is a shorter, straighter and hence more direct pathway, often in the distal bronchial tree, whereas in children the foreign body is more likely to be centrally located in the proximal bronchial tree. A systematic review conducted by Seghal, et al. [1] analysed a bronchoscopy database for those over the age of twelve, 25,998 cases were examined, and 65 cases of foreign body aspiration were found. 75% of the patients were male, with a mean age of 32.
They found that the most common radiological abnormalities were "Non-resolving pneumonia (30.6%), direct foreign body visualization (24.6%), and segmental collapse (18.4%)". The systematic review the conducted showed 0.24% of flexible bronchoscopies were performed to remove foreign bodies and success removal was 89.6%.
It is important that a diagnosis is sought, both for physiological resolution of symptoms, to prevent ongoing damage to lung parenchyma and to ensure that appropriate referrals are sought for ongoing prevention of recurrence, such as speech and language therapy reviews and swallow assessments, to determine if diet modifications would be appropriate to minimise risk.
Case Presentation
The authors present the case of a 69-year-old lady who presented in respiratory distress secondary to foreign body aspiration which became stuck in her right bronchus intermedius. Her comorbidities include breast cancer (recent surgery for this), hypertension and Grave's disease. Her medication includes anastrazole, carbimazole, enalopril and simvastatin.
She was eating fish and chips, when she choked and felt she inhaled a pea. She perpetually coughed post event and was unable to talk in full sentences, with increasing levels of dyspnoea. On the ward she was requiring 2L of oxygen to maintain saturations above 95%.
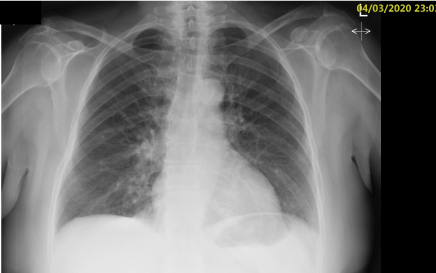
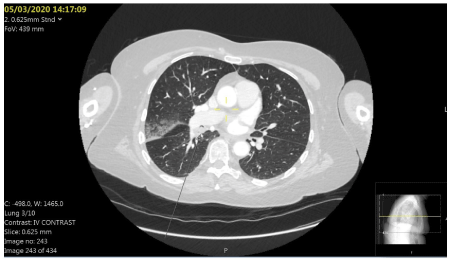
Admission chest x-ray showed possible airspace shadowing at the medial left lower lobe (Figure 1). Her CT scan (Figure 2) was reported as a soft tissue density filling defect within the right bronchus intermedius consistent with foreign body. Right upper lobe focal ground-glass change seen associated with the oblique fissure with a further focus of ground-glass changes seen at the anterior margin of the right lung apex. There is also septal thickening towards the lung bases which should be suspicious for a superadded infective aetiology.
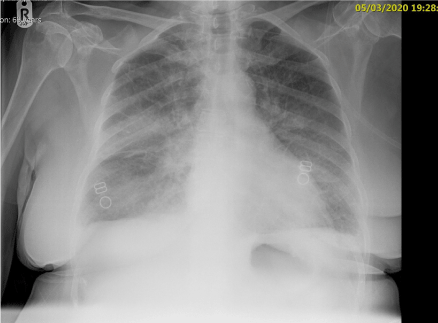
She was discussed with cardiothoracic surgery who advised transfer for a rigid bronchoscopy under general anaesthesia. Whilst awaiting transfer, she became tachypnoeic (from 24 to 36), tachycardic, hypertensive and intensive care were called. She developed a broad complex tachycardia, left bundle branch block (LBBB) and hyper-acute T-waves. Her repeat chest x-ray (Figure 3) showed increased shadowing in part of the upper lobe, possible inflammatory change/pulmonary oedema and bilateral effusions. She was intubated in extremis with fentanyl, ketamine and rocuronium and ventilated on intensive care.
The on-call cardiothoracic team advised she wouldn't have the bronchoscopy overnight, that the pea would not act as a ball valve and that supportive care should be continued overnight. She was in type 1 respiratory failure, was commenced on steroids, diuretics and piperacillin-tazobactam.
She was seen by cardiology who felt the new LBBB was due to a type 2 myocardial infarction, her initial troponin was 611, repeat was 817. She was commenced on aspirin and clopidogrel as she was too unstable to have an angiogram overnight. The following day the LBBB had resolved and Q waves developed. An echocardiogram was performed and showed normal sized left ventricle, moderate-severe systolic impairment, anterior and inferior hypokinetic/akinetic, with preserved apical function.
She underwent an angiogram which showed mild non-obstructive coronary artery disease, mild left ventricular systolic dysfunction and an end diastolic pressure of 16 mmHg - indicating stress cardiomyopathy secondary deemed most likely due to respiratory distress; subsequently her anti-platelets were then weaned.
She had a bronchoscopy, foreign body was visualised in the right lower lobe, this was grasped with biopsy forceps, however became stuck in the endotracheal tube on removal. She was extubated and reintubated with a new tube to remove the pea.
Subsequently to the pea being removed; noradrenaline was stopped, she was successfully extubated and oxygen was weaned. Her antibiotics were de-escalated to co-amoxiclav and she was discharged home from intensive care the following day.
Discussion
Foreign body aspiration presents in a bimodal distribution with peaks at the extremes of age, young children and the elderly, the latter often a consequence of neurological or neuromuscular disease. Data analysis from CE Safety found that "in four years 1571 people have died from choking... 398 in 2017... with the over 72% of these being over 65 years old - the numbers of which are increasing annually" [2].
Mise, et al. analysed 26,124 bronchoscopies for foreign bodies, these were identified in 0.33% of cases, of which 58% of all cases had underlying neurological or neuromuscular disease. Typically the foreign body trends towards the right bronchial tree (75.6%) of cases, and only 7% of cases had the foreign body visible on chest x-ray [3].
As such risk factors for foreign body aspiration include reduced Glasgow Coma Score (GCS) either secondary to neurological disease or sedative medications including alcohol, drugs such as anticholinergics or antipsychotics, extremes of age, either children accidentally inhaling toys/foreign objects or elderly as a result of dysphagia from neurological conditions such as previous stroke inducing dysphagia or conditions such as muscular dystrophy causing swallowing difficulties or cough reflex [4].
Symptoms of aspiration can range from life-threatening airway obstruction with collapse or a bidirectional stridor or in the instance of smaller objects/partial obstruction; include coughing, shortness of breath and wheezing. Later signs may include fever, in the case of subsequent infection or maybe asymptomatic and found incidentally. On examination wheeze may be audible, or unilateral absence of breath sounds noted.
Our patient was aware of the aspiration event and gave a clear clinical history on presentation to the Emergency department, however, it often presents in an insidious manner, with patients often not recalling the aspiration event, such as the food matter aspirated in the cases highlighted. Complications of such events can result in recurrent pneumonia and even persistent bronchiectasis after the foreign body has been removed, which can be as extreme as to require partial lobectomy surgery [5].
Differential diagnosis can include pneumonia or reactive airway disease such as asthma and chronic obstructive airway disease. Although considered a rare event in the adult population, it is important for early recognition and diagnostic bronchoscopy is performed in individuals of high risk as it can often have disastrous consequences. A case of foreign body aspiration induced cardiac arrest was documented by Kashif, et al. [6] who reports the case of a 48-year-old out-of-hospital pulse less electrical activity (PEA) arrest, who was investigated with a flexible bronchoscope and discovered to have aspirated meat, who went onto had full neurological recovery.
Management is dependent on whether the patient is conscious, as per life support algorithms [7]. However, first line investigation would include a plain film chest x-ray which may aid in locating the object if radiopaque (occurs in 2-19% of cases, less likely in the case of organic matter) [8]. Otherwise non-specific findings that may indicate aspiration include "atelectasis, pneumonia, air trapping, and pneumomediastinum" [4]. Second line investigations would include CT chest to improve detection rates, avoid subjecting a small child to unnecessary bronchoscopy, or aid location of said object during bronchoscopy.
Diagnosis and removal of foreign body initially involves the use of a flexible bronchoscope, or a ridged bronchoscope if the former fails. In adults, this can often take place under local anaesthetic, which is preferable given the patient group prone to aspirating are often frail comorbid ASA 3 or 4 patients.
Anaesthetic considerations for foreign body removal include the risks associated with shared airway procedures, ensuring adequate supply of hypnotic agent to prevent awareness and the potential for the situation to become life-threatening on induction. Pre-operative assessment should include analysis of previous anaesthetic charts for grade of intubation. Airway assessment such as mallampati scoring and assessment of clinical condition, in particular worrying signs such stridor, hoarse voice and drooling. It is important to view pre-operative imaging to identify the level of obstruction.
Induction is a concerning time, as there is the potential to dislodge and potentially cause total obstruction, by switching from spontaneous negative pressure ventilation to mandatory positive pressure ventilation. There are two options for induction, either gaseous or intravenous, both of which aim to keep the patients spontaneously ventilating throughout induction. It is important pre-medicate with anti-saliva medication to reduce secretions, and to use topical anaesthetic to the airway with lidocaine (at a dose of 4mg/kg) to minimise vocal cord irritation and potential coughing.
Maintenance of anaesthesia can either be via the use of total IV anaesthesia (TIVA) or vapours via connection to the bronchoscope side port. TIVA has the advantage that the anaesthetist is not relying on a shared airway, and often jet ventilation which needs to be intermittently stopped during the procedure. Intraoperative risks include dropping of the foreign body during removal which can cause life-threatening obstruction, trauma/bleeding from the scope and an inability to ventilate due to obstruction. High flow jet ventilation is associated with risks of barotrauma and gas trapping due to partial obstruction of exhalation; it is hence important to monitor airway pressures and end tidal carbon dioxide levels and increase the expiratory time to avoid developing respiratory acidosis.
Long-term prophylaxis includes appropriate reviews from speech and language teams regarding potential requirements for thickened fluids, ensuring that the elderly are monitored whilst eating, minimising poly-pharmacy, whilst avoiding anti-sialagogues, which can further impair swallowing and ensuring good dental hygiene/correctly fitting dentures [4].
In conclusion, it is important to remain vigilant for patients with a known foreign body aspiration for instances of acute deterioration in clinical condition. A literature review into this matter highlights that although in the majority of circumstances patients suffering from aspirations often have comorbidities that predispose them to this, it is not always the case, and it can have catastrophic consequences including cardiac arrest if it goes unnoticed.
References
- Sehgal I, Dhooria S, Ram B, et al. (2015) Foreign body inhalation in the adult population: Experience of 25,998 bronchoscopies and systematic review of the literature. Respir Care 60: 1438-1448.
- https://cesafety.co.uk/choking-deaths-report-2019/
- Mise K, Jurcev Savicevic A, Pavlov N, et al. (2008) Removal of tracheobronchial foreign bodies in adults using flexible bronchoscopy: Experience 1995–2006. Surg Endosc 23: 1360-1364.
- https://bestpractice.bmj.com/topics/en-gb/653
- Zubairi A, Haque A, Husain S, et al. (2006) Foreign body aspiration in adults. Singapore Med J 47 : 415.
- Kashif M, Talib Hashmi H, Khaja M (2016) Early recognition of foreign body aspiration as the cause of cardiac arrest. Case Rep Crit Care 2016: 1-4
- Resuscitation council UK (2020) Adult basic life support and automated external defibrillation.
- Paintal HS, Kuschner WG (2007) Aspiration syndromes: 10 clinical pearls every physician should know. Int J Clin Pract 61 :846-852
Corresponding Author
Sarah Brown, Guys and St Thomas, United Kingdom
Copyright
© 2022 Brown S. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.