Bedside Lung Ultrasonography in the Assessment of the Postoperative Atelectasis
Postoperative atelectasis may complicate the progress of patients after major abdominal surgery. Lung ultrasonography plays a key role in the diagnosis of lung consolidations (atelectasis, pneumonia, etc.) as it not only enables diagnosis at the patient's bedside, but also treatment response assessment in real time [1]. We present the case of a patient who, at early stages of the postoperative period of major abdominal surgery, presented moderate hypoxemia secondary to the presence of bilateral alveolar consolidations which were diagnosed using bedside lung ultrasonography. These were resolved after treatment administration which was also assessed using bedside lung ultrasonography.
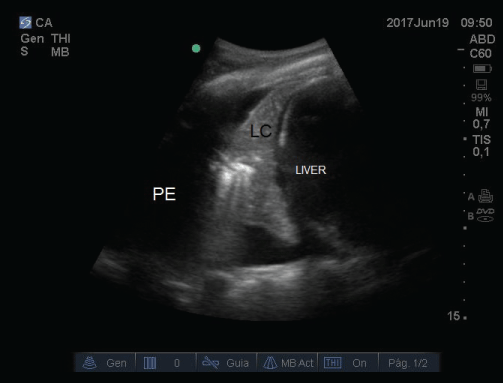
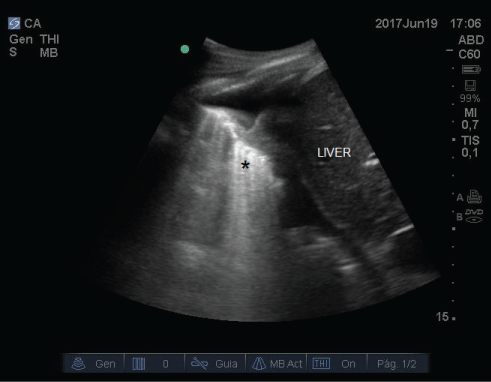
A 61-year-old patient, who was a smoker and had a history of hypertension, was admitted to the postoperative Intensive Care Unit after undergoing a laparotomy to amend a perforated duodenal ulcer. Blood component therapy was not necessary during surgery and fluid therapy was goal directed. In the early stages of the post-operative period, moderate hypoxemic respiratory failure was observed with FiO2 0.35 (pO2 53 mmHg) without hypercapnia. The patient was afebrile. Pulmonary auscultation showed bilateral hypoventilation with no additional sounds. Bedside lung ultrasonography was performed with a SonoSite M-Turbo® scanner using a high-frequency linear probe (6-13 MHz) for the anterior lung regions and a low-frequency convex probe (3-5 MHz) for the lung bases. Bilateral pleural effusion was appreciated and bilateral basal lung consolidations appeared as hypoechogenic masses with static air bronchograms [2] (Image 1). In view of the diagnosis of bilateral atelectasis, the treatment applied was non-invasive ventilation with PEEP values between 7-8 cm H2O (cycles of 2 hours with 1 hour rest, with face mask for 24 hours). Also bedside lung ultrasonography was used to monitor treatment response observing how, after non-invasive ventilation; the sonography pattern of consolidation was replaced by B lines in the following hours, which indicated aeration of the alveolar consolidation [3,4] (Image 2). The patient progressed favorably and was discharged to a ward 72 hours after receiving treatment (non-invasive ventilation and respiratory physiotherapy).
The present case report aims to emphasize the importance of bedside ultrasonography in critically ill patients and how it enables not only diagnosis but also follow-up of the treatment response.
References
- Volpicelli G, Elbarbary M, Blaivas M, et al. (2012) International evidence-based recommendations for point-of-care lung ultrasound. Intensive Care Med 38: 577-591.
- Lichtenstein D, Mezière GA (2008) Relevance of lung ultrasound in the diagnosis of acute respiratory failure: the BLUE protocol. Chest 134: 117-125.
- Tusman G, Acosta CM, Constatini M (2016) Ultrasonography for the assessment of lung recruitment maneuvers. Crit Ultrasound J 8: 8.
- Bouhamed B, Brisson H, Le Guen M, et al. (2011) Bedside ultrasound assessment of positive end-expiratory pressure-induced lung recruitment. Am J Respir Crit Care Med 183: 341-347.
Corresponding Author
Domínguez D, Surgical Intensive Care Unit, Department of Anesthesiology and Critical Care, Hospital Universitario Nuestra Señora de Candelaria, Spain.
Copyright
© 2017 Domínguez D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.