A Case Report and Literature Review of the de Garengeot
Abstract
Inguinal and femoral hernias are a common condition evaluated and managed by the general surgeon. The femoral hernia is less common of the two and carries a high risk of strangulation, mandating an urgent repair. An exceptionally rare finding is the vermiform appendix within the femoral hernia sac, known as a de Garengeot hernia. Herein we present a case and review of the etiology, incidence, and management of a de Garengeot hernia.
Keywords
de garengeot hernia, Vermiform appendix, Femoral hernia
Introduction
Abdominal wall hernias are a relatively common condition affecting close to 5% of the population. An estimated 75% of these hernias occur in the groin [1]. Femoral hernias are much less common, accounting for approximately 3% of groin hernias [2]. Although femoral hernias occur more frequently in women than men, inguinal hernias remain the most common type in women overall [3]. Femoral hernias tend to occur later in life and are known to have a higher rate of strangulation and incarceration (up to 20%) when compared to other types of hernia, thus requiring urgent repair [4].
The hernia sac is a potential space that may entrap pre-peritoneal and intra-abdominal contents. Both femoral and indirect inguinal hernias are more common on the right side, since the sigmoid colon often impedes access to the left femoral canal. Rarely, the appendix may be found within a hernia sac. When the appendix is found within the sac of an inguinal hernia it is known as Amyand's hernia. An even more uncommon finding is the appendix within the sac of a femoral hernia [5,6]. We present a case of this rare finding, known as a de Garengeot hernia, which occurs in less than 1% of femoral hernias. In this case report, we discuss the incidence and prevalence of this condition, as well as a review of the literature regarding diagnosis and management.
Case Report
An eighty-nine-year-old female presented to our emergency department with complaints of a painful right inguinal mass. She had a seven year history of a reducible right inguinal hernia which had become irreducible, distended, and acutely painful for forty-eight hours prior to admission. Her other medical history also included a pelvic procedure for bladder suspension, radiation treatment for a skin neoplasm, and Alzheimer's dementia.
On physical exam, the hernia was located medially below the inguinal ligament near the pubic tubercle, and was irreducible with moderate tenderness. The overlying skin did not have cellulitis, erythema, or induration. Despite regular bowel movements, her abdomen had become distended. In addition, she was found to have developed sudden new onset atrial fibrillation, but remained afebrile and normotensive. Her laboratory findings were within normal limits without evidence of lactic acidosis or leukocytosis.
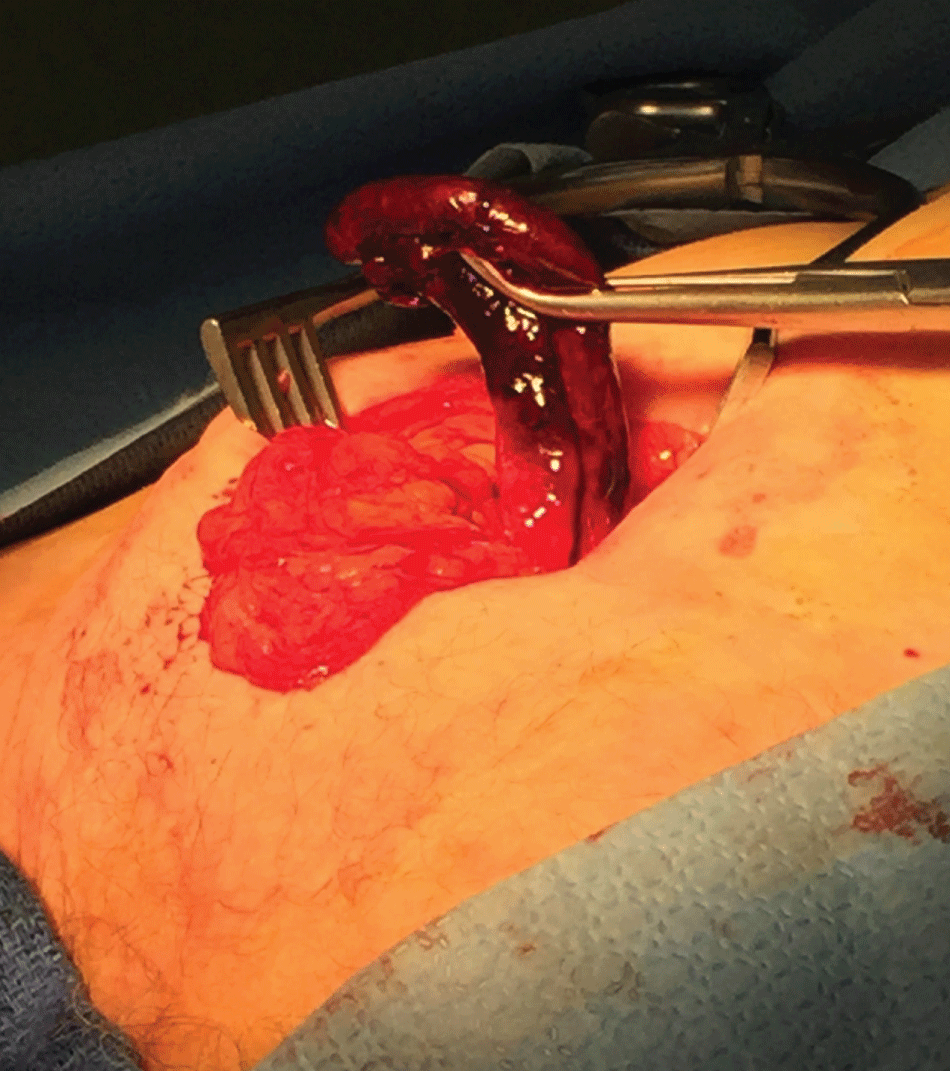
The patient was taken emergently to the operating room for repair of a suspected incarcerated femoral hernia. Given the development of a new cardiac arrhythmia, we also had concern for a strangulated hernia with impending visceral compromise. An oblique incision was made at the level of the inguinal ligament and the inguinal canal was exposed and opened. A femoral hernia was identified in the femoral canal. After dividing the inguinal ligament, we opened the sac and found a necrotic appendix containing black fluid with the necrosis extending distal to the base of the cecum (Figure 1). We performed an appendectomy through the hernia sac and buried the stump with a z-stitch. We amputated the sac and repaired the hernia using a Cooper's ligament primary tissue repair. The appendix was sent for confirmatory pathologic examination.
During the operation, the patient spontaneously returned to a normal sinus rhythm. Post-operatively, the patient tolerated a diet and was discharged within 24 hours on oral antibiotics. The patient was seen in follow up two weeks after her discharge. She continued to do well and was returning to her activities of daily living without limitation. She was seen once again, about one month following her operation, was convalescing without issue, and was discharged to her primary physician.
Discussion
Described first in 1731 by the French surgeon Rene Jacques Croissant de Garengeot, a de Garengeot hernia is a femoral hernia containing the appendix within its sac. It should be noted that the eponym for this rare hernia was not bestowed until the year 2005 [7,8]. Interestingly, the original report of this hernia subtype predates the description of the first appendectomy, which was performed in London by Claudius Amyand, also a French surgeon, in the year 1735 [9]. Amyand's name also became eponymous with the rare finding of a vermiform appendix within the sac of an inguinal hernia.
There is evidence that the incidence of femoral hernia increases as the population ages. In a retrospective and prospective study, Arenalet, et al. assessed all patients over the age of seventy with abdominal wall hernia in whom their group operated on. In patients over seventy years, femoral hernias occurred in 52% of women and 7% of men. The incidence of femoral hernia of patients in the age group of 80-89 years old was 36% of all abdominal hernias in the study population, compared to 16% of patients in the age group 70-79. Emergency operations also were found to be increasingly necessary in more advanced age. Whereas 22% of patients in their seventies underwent an emergency operation, 53% of patients in their eighties, and 89% of those in their nineties underwent an emergent procedure [10].
The diagnosis of a de Garengeot hernia is often made intra-operatively while exploring a femoral hernia [8]. As in our case, physical exam often leads to operative exploration given the high risk of incarceration associated with a femoral hernia. Imaging may be pursued, though is usually not helpful in establishing a diagnosis [11,12]. Computed tomography (CT) may show intestinal pneumatosis, which is evidence of an incarcerated hernia with visceral involvement. However, CT often does not reveal the obstructive findings typical of small bowel involvement [8,13].
At exploration, an appendix within the femoral hernia sac often appears inflamed, gangrenous, or necrotic. The sac may contain murky or purulent fluid. These findings seem to indicate acute appendicitis, but may also result from an appendix incarcerated within a tight femoral ring [13]. Distinguishing between these etiologies may not affect the management of the appendix, however, as most reports in the literature advocate for appendectomy at the outset [6]. Due to the limited number of cases reported in the literature, an approach to de Garengeot hernia repair has not been uniformly established. Some authors advocate for the use of prosthetic mesh and a pre-peritoneal approach for repair of the femoral defect, while others have performed the traditional Cooper's ligament repair with good result [7,8,14,15]. The decision to use mesh is typically based on the surgeon's appreciation for gross contamination within the wound. Laparoscopic approaches, such as trans abdominal preperitoneal (TAPP) hernia repair, have also been successful [16,17]. Laparoscopy may be most useful when the clinical diagnosis is difficult or indeterminate.
References
- Ruhl CE, Everhart JE (2007) Risk factors for inguinal hernia among adults in the US population. Am J Epidemiol 165: 1154-1161.
- Dahlstrand U, Wollert S, Nordin P, et al. (2009) Emergency femoral hernia repair: A study based on the nation register. Ann Surg 249: 672-676.
- Koch A, Edwards A, Haapaniemi S, et al. (2005) Prospective evaluation of 6895 groin hernia repairs in women. Br J Surg 92: 1553-1558.
- Kark AE, Kurzer M (2008) Groin hernias in women. Hernia 12: 267-270.
- Tanner N (1963) Strangulated femoral hernia appendix with perforated sigmoid diverticulitis. Proc R Soc Med 56: 1105-1106.
- Voitk AJ, McFarlane JK, Estrada RL (1974) Ruptured appendicitis in femoral hernias: report of two cases and review of the literature. Ann Surg 179: 24-26.
- Akopian G, Alexander M (2005) De Garengeot hernia: Appendicitis within a femoral hernia. Am Sug 71: 526-527.
- Shum J, Kris C (2012) Management of appendicitis in a femoral hernia. Int J Surg Case Rep 3: 10-11.
- Mohamed A, Bhatty T, Rashad A, et al. (2009) Amyand: A forgotten surgeon and hernia: case presentation and literature review. Internet J Urol 7.
- Arenal JJ, Rodrigeuz-Vielba P, Gallo E, et al. (2002) Hernias of the abdominal wall in patients over the age of 70 years. Eur J Surg 168: 460-463.
- Nguyen ET, Komenaka IK (2004) Strangulated femoral hernia containing a perforated appendix. Can J Surg 47: 68-69.
- D'Alia C, Lo Schiavo MG, Tonante A, et al. (2003) Amyand's hernia: Case report and review of the literature. Hernia 7: 89-91.
- Ebisawa K, Yamazaki S, Kimura Y, et al. (2009) Acute appendicitis in an Incarcerated femoral hernia: A case of de Garengeot hernia. Case Rep Gastroenterol 3: 313-317.
- Rose RH, Cosgrove JH (1988) Perforated appendix in the Incarcerated femoral hernia: A place for Pre Peritoneal Repair. NY State J Med 32: 380-381.
- Priego P, Lobo E, Moreno I, et al. (2005) Acute appendicitis in an incarcerated crural hernia: Analysis of our experience. Rev Esp Enferm Dig 97: 707-715.
- Comman A, Gaetschmann P, Hanner T, et al. (2007) DeGarengeot hernia: Transabdominal preperitoneal hernia repair and appendectomy. JSLS 11: 496-501.
- Al-Subaie S, Mustafa H, Al-Sharqawi N, et al. (2015) A case of de Garengeot hernia: The feasibility of laparoscopic transabdominal preperitoneal hernia repair. Int J of Sur Case Rep 16: 73-76.
Corresponding Author
B Phillips, Vice Chairman of Surgery-Surgical Research, Associate Professor of Surgery, Department of Surgery; Associate Professor of Clinical and Translational Science, Department of Clinical and Translational Science; Creighton University School of Medicine, Creighton University Medical Center, 601 North 30th Street, Suite 3701, Omaha, NE 68131-2137, USA, Tel: 402-717-4842, Fax: 402-717-6062.
Copyright
© 2017 Serio S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.