What are the Main Pathogenetic Features of Vascular Cognitive Impairment?
Abstract
The term vascular cognitive impairment designates a heterogenous group of disorders ranging from mild cognitive impairment to full-blown dementia-vascular dementia-resulting from cerebrovascular lesions involving various brain areas. Current clinical criteria show moderate sensitivity (50-56%) and variable specifi city (range 64-98%). The prevalence in autopsy series ranges from 0.03 to 58% (mean 8-15% in Western series, 22-35% in Japan). Major morphological types-multiinfarct and subcortical vascular encephalopathy, strategic infarct dementia, lacunar state, granular atrophy (rare), and ischemic encephalopathy-are caused by atherosclerosis of major cerebral arteries and small vessel disease, resulting from systemic, cardiac and local vascular disease or cerebral amyloid angiopathy. Pathogenesis of vascular dementia is multifactorial, and pathophysiology affects brain areas and neurological networks involved in cognition, memory, behavior, and executive functions. Vascular brain injury in elderly persons often coexists with Alzheimer-type lesions and other pathologies resulting in mixed dementia. The heterogeneity of clinical manifestations, cerebrovascular pathology and their pathogenic factors result in limitations of the accuracy of diagnostic criteria for vascular dementia. Recent standardized and reproducible neuropathological criteria for the assessment of cerebrovascular lesions associated with cognitive impairment need to be validated by prospective clinico-pathologic studies.
Keywords
Vascular cognitive impairment, Vascular dementia, Cerebrovascular disease, Small vessel dementia, Neuropathology
Abbreviations
AD: Alzheimer Disease; BBB: Blood-Brain Barrier; CVLs: Cerebrovascular Lesions; MCI: Mild Cognitive Impairment; SID: Strategic Infarct Dementia; SvaD: Subcortical Vascular Dementia; SVD: Small Vessel Disease; VaD: Vascular Dementia; VCI: Vascular Cognitive Impairment; WMH: White Matter Hyperintensities
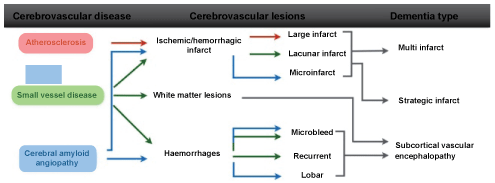
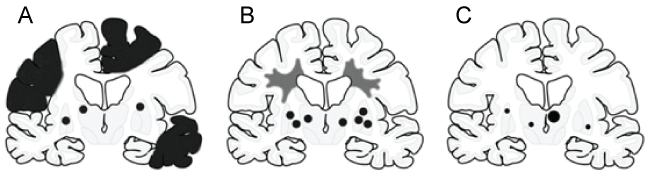
Vascular cognitive impairment (VCI) describes a heterogenous group of cognitive disorders ranging from mild cognitive impairment (MCI) to full-blown dementia-vascular dementia (VaD)-resulting from cerebrovascular lesions (CVLs), involving different neuronal networks. They are mainly caused by the following blood vessel diseases: atherosclerosis (AS) of major cerebral arteries, small vessel disease (SVD) resulting from systemic, cardiac and local vascular disease, cerebral amyloid angiopathy (CAA), and cerebral hypoxia. The major patterns of brain lesions distinguish: 1. multi-infarct encephalopathy, and 2. subcortical vascular encephalopathy, and 3. strategic infarct dementia [1-3] (Figure1 and Figure 2).
Morphological substrates of VaD are related to large and small vessel disease (Table 1).
1. Large vessel dementia: Multi-infarct encephalopathy (about 15% of VCI) featured by multiple large and small infarcts in supply areas or borderzones of major cerebral arteries due to severe AS of extra- and intracranial vessels causing local thrombo-embolism, hypoperfusion and cardiogenic emboli, caused by breaking of thrombi from ulcerated lesions in extracranial arteries or heart valves. Inflammatory and rare hereditary angiopathies, e.g. CADASIL, frequently cause smaller infarcts [4]
2. Small vessel disease (SVD)/microangiopathic dementia with microinfarcts, lacunes and microbleeds, predominantly involving subcortical structures (white matter, basal ganglia, intern capsule) due to microvascular changes, e.g., fibrosis, stenosis, hypertensive angiopathy, etc. These changes are present in more than 60% of VCI patients.
Small vessel lesions include [1-4]:
a) Lacunar state with multiple cortico-subcortical lacunes or microinfarcts, found in 32-45% of elderly as the most frequent type of CVLs.
b) Strategic infarct dementia (SID) with small infarcts in functionally essential brain areas (thalamus, frontocingular cortex, hippocampus) due to SVD or embolism. They destruct neuronal networks that are important for cognition and behavior.
c) Watershed or borderzone (cortical and/or subcortical) infarcts in cerebral convexities or borderzones between major cerebral arteries or in territories between small deep and superficial vessels.
d) Subcortical vascular dementia (SVaD) or arteriosclerotic (leuko) encephalopathy type with confluent white matter lesions (demyelination, axonal loss due to lacunar infarcts or related with enlarged perivascular areas), usually sparing subcortical U-fibers [1,5]. White matter hyperintensities (WMH) seen in magnetic resonance imaging (MRI) in elderly individuals with and without cognitive impairment, are generally associated with SVD and edema. The lesions are caused by disturbances of the blood-brain barrier (BBB), hypotension and ischemia, but recent studies indicate also relationship to cortical neurodegenerative tau-pathology in Alzheimer disease (AD) [6].
e) Cerebral microbleeds, associated with increased ischemic stroke risk, are markers of consequences of both hypertensive SVD and CAA [1,2,4].
3. Further pathological substrates of VCI include:
a) Post-ischemic encephalopathy with:
• Cortical laminar necrosis mainly in arterial border zones resulting from hypoxia due to cardiac or respiratory arrest;
• Multiple post-ischemic lesions with cortical/subcortical (micro)infarcts;
• Hippocampal sclerosis of hypoxic-ischemic etiology, but also associated with neurodegeneration or advanced age.
b) Hemorrhagic dementia due to primary (hypertensive) intracerebral hemorrhages is rare.
c) Combined (multifocal) cerebrovascular lesions involving various brain regions, related to different vascular changes.
Clinical Features
Cognitive changes in VCI/VaD are more variable than in AD and are dependent on the particular neuronal substrates related to the vascular pathology, while other functions such as memory, language, executive functions and non-cognitive features, depression and apathy are much more affected; delusions and hallucinations are less frequent [7,8].
Previous diagnostic criteria for VCI/VaD requested the presence of memory loss independent of dementia. Currently, several sets of criteria for the clinical diagnosis of VCI/VaD are used [2,7]: the NINDS-AIREN criteria, the ADDTC criteria, the DSM-V criteria (APA), distinguishing possible, probable and proven VaD (with pathologically proven multiple cerebrovascular lesions/CVLs), the NINDS-CSN criteria, the EFNS guidelines, the consensus statement of the American Stroke Association, and the VASCOG criteria.
Several studies reported moderate sensitivity of clinical criteria (average 50-56%) and variable specificity (range 64-98%) with variable interrater reliability [7,8]. The heterogeneity of clinical manifestations, cerebrovascular pathology and their pathogenic factors result in limitations of the accuracy of diagnostic criteria for VCI/VaD. The limitations of current clinical diagnostic criteria sets for VCI/VaD that poorly reflect the underlying pathology, have been critically discussed recently [2,4,9].
In clinical studies, the prevalence of VaD ranges from 4.5 to 39%, in Western memory clinic- and population-based series 8-15%, in pathological series even 0.03-85.2% with means around 11-15%, and in Japan 23.6-35% [2]. The prevalence studies must be interpreted cautiously since aged subjects with and without dementia show a high frequency of mixed pathologies [5,10].
In elderly patients the prevalence of "pure" VaD morphologically characterized by multiple CVLs without essential concomitant AD-type (Braak neuritic stage < 2.0) and other pathologies ranges from 5 to 78% with mild reduction in the oldest-old, while that of mixed dementia increases with age [1]. Recent studies have emphasized the co-morbidities associated with VaD and AD-like pathology, resulting in mixed dementia. Although there is an established relationship between vascular and degenerative (AD) pathology, the links between the two lesions have to be identified. In general, however, vascular brain damage is believed to be an important component of AD pathophysiology [5,10]. However, the impact of cooccurring pathologies on progression of cognitive impairment may depend on the severity of AD pathology [8,10,11].
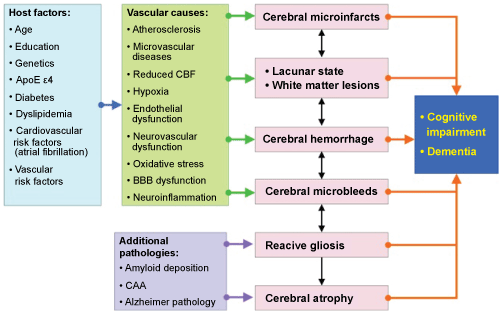
The pathogenesis of CVLs inducing cognitive impairment is multifactorial, resulting from systemic or local vascular and cardiac disease (Table 2). They affect neuronal networks involved in memory, cognition, behaviour and executive functions (thalamo-cortical, striato-subfrontal, limbic systems). Due to frequent comorbidity in old age, cerebrovascular pathology often coexists with Alzheimer-type lesions and other pathologies. 25 to over 80% of elderly both demented and non-demented individuals show mixed pathologies [4,10]. The systemic interplay of pathogenic factors related to VCI is summarized in (Figure 3).
Standardized neuropathological criteria for the assessment of CVLs associated with cognitive impairment are urgently needed. However, despite several recent suggestions for staging and grading vascular lesions in specific brain areas, due to the high variability of these lesions, no generally accepted and validated criteria are currently available for VCI/VaD [1-4]. A recent collaborative study of nine UK neuropathological centers to formulate evidence-based Vascular Cognitive Impairment Neuropathology Guidelines (VCING) for post-mortem assessment of CVD of relevance for BCI/VaD has shown that various combinations of three pathologies (occipital leptomeningeal CAA, atherosclerosis in occipital white matter, and at least one infarct) can be used to report a low, intermediate or high likelihood that CVD contributed to cognitive impairment [12]. Like previous proposals for classification and rating of vascular and related cerebral lesions causing cognitive impairment, the VCING needs validation by prospective clinico-pathologic studies. Further clinico-pathological studies and harmonization of neuropathological procedures are needed to validate the diagnostic criteria for VaD in order to elucidate the impact of CVLs and coexistent pathologies on cognitive impairment as a basis for successful preventive and therapeuthic options.
References
- Jellinger KA (2013) Pathology and pathogenesis of vascular cognitive impairment-a critical update. Front Aging Neurosci 5: 17.
- Jellinger KA (2014) Pathogenesis and treatment of vascular cognitive impairment. Neurodegener Dis Manag 4: 471-490.
- Jellinger K (2016) Current pathogenetic concepts of vascular cognitive impairment. J Neurol Neurol Sci Disord 2: 010-016.
- Kalaria RN, Akinyemi R, Ihara M (2016) Stroke injury, cognitive impairment and vascular dementia. Biochim Biophys Acta 1862: 915-925.
- McAleese KE, Alafuzoff I, Charidimou A, et al. (2016) Post-mortem assessment in vascular dementia: advances and aspirations. BMC Med 14: 129.
- McAleese KE, Walker L, Graham S, et al. (2017) White matter lesions in Alzheimer's disease are associated with cortical neurodegenerative pathology but not with small vessel disease (abstr.). Neuropathol Appl Neurobiol 43: 15.
- O'Brien JT, Thomas A (2015) Vascular dementia. Lancet 386: 1698-1706.
- Jellinger KA (2013) How should vascular dementia be managed? Neurodegen Dis Manage 3: 109-113.
- Skrobot OA, O'Brien J, Black S, et al. (2016) The Vascular Impairment of Cognition Classification Consensus Study. Alzheimers Dement 13: 624-633.
- Jellinger KA (2016) Cerebral multimorbidity in aging. J Neurol Neuromed 1: 1-5.
- Attems J, Jellinger KA (2014) The overlap between vascular disease and Alzheimer's disease-lessons from pathology. BMC Med 12: 206.
- Skrobot OA, Attems J, Esiri M, et al. (2016) Vascular cognitive impairment neuropathology guidelines (VCING): the contribution of cerebrovascular pathology to cognitive impairment. Brain 139: 2957-2969.
Corresponding Author
Kurt A Jellinger, Institute of Clinical Neurobiology, Vienna, Austria, Tel: +43-1-5266534.
Copyright
© 2017 Jellinger KA. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.