What's Your Diagnosis? A 7-Year-Old Boy with a White Hair Patch on the Head for Three Months
Abstract
Background
Tinea capitis is one of the most common dermatophyte infections in children, particularly among African American children. It can manifest with a variety of clinical presentations ranging from the subtle seborrheic dermatitis subtype to the more severe kerion pattern, with boggy and tender lesions. The most common presentation, however, is the scaly, pruritic multiple patches of alopecia with the involved hair shafts are broken off at the surface giving the appearance of black dots. A less common presentation of tinea capitis is the grey patch type and it is usually caused by M. canis.
Methods
The patient presented with a white hair patch on the scalp that was fully noticed about 3 months ago at the site of an initial diagnosis of tinea capitis that took place 6 months ago. The patient was then treated successfully with Griseofulvin for 6 weeks and showed improvement, however, the growing hair at the site has become whitish in color.
Results
The scalp fungal culture that was obtained at the current visit was negative. At 12-months following the original tinea capitis infection, the discolored white hair patch continued to improve as it was being replaced with a mixture of both more whitish colored hair mixed with the naturally colored hair.
Conclusion
Tinea capitis can rarely lead to poliosis with depigmented white hair patch as a consequence of the fungal infection. This presentation can be confusing to the parents as well as to the treating physicians. Management includes proper recognition and treatment of the initial infection together with monitoring for further restoration of the original hair color.
Keywords
Tinea capitis, Gray patch type, White hair patch, Poliosis
Presentation
A 7-year-old African American boy is being evaluated for his annual well child visit at the outpatient academic general pediatrics clinic of Children's Hospital of Michigan (CHM). The mother reports a white hair patch on the scalp that has been present for the last 3 months. She also reports that the boy was seen 6 months earlier at CHM and was diagnosed with tinea capitis. He then successfully completed a 6 weeks course of 25 mg/kg/day of Griseofulvin. The mother also noted that within 4 weeks following the initial diagnosis of tinea capitis, there was a slight change in pigmentation of the hair over the affected scalp patch. Mom has been using 1% selenium sulfide shampoo twice a week for the last 6 months although records show that the shampoo was recommended for 4 weeks only. Mother denies applying to the lesion any other topical products including bleach. Also she denies history of hair pulling or a family history suggestive of similar lesions.
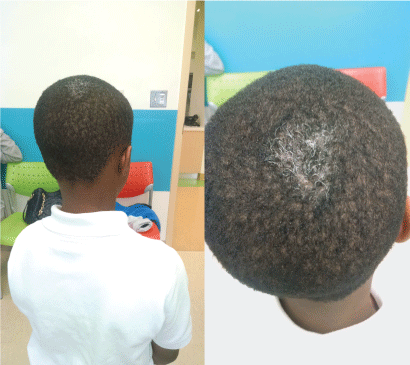
On physical examination, the child appears healthy and well developed. On the posterior aspect of the scalp, there is a 3 × 4 cm slightly scaly patch with scattered depigmented white hairs (Figure 1). The rest of his physical examination is unremarkable.
What's your diagnosis?
A) Resolving Tinea capitis with poliosis; B) Drug/Chemical-induced skin reaction; C) White forelock; D) Bacterial folliculitis
Answer: A) Resolving tinea capitis with poliosis.
Discussion
Tinea capitis is one of the most common dermatophyte infections in children, particularly among African American children [1,2]. Tinea capitis can be caused by several dermatophytes; however, Trichophyton tonsurans is the most prevalent etiologic agent in the United States, responsible for more than 90% of infections [3]. The infection can be transmitted to humans by anthropophilic (between people), geophilic (from soil), and zoophilic (from animals) agents.
Tinea capitis can manifest with a variety of clinical presentations ranging from the subtle seborrheic dermatitis subtype with diffuse scaling and mild inflammatory response, to the more severe kerion pattern, with boggy and tender lesions with significant hair loss and purulent drainage along with cervical or sub-occipital lymphadenopathy.
The most common presentation, however, is the scaly, pruritic multiple patches of alopecia with the involved hair shafts are broken off at the surface giving the appearance of black dots. Depending on the severity, cervical or sub occipital lymphadenopathy can be present [4].
On the other hand, a less common presentation of tinea capitis is the grey patch type which can be found endemically within the United States, and the offending agent is typically M. canis. It is characterized by the involvement of both the surface skin and the infected broken bits of hair shafts with white scales resulting in a mixture of black and white giving the appearance of the grey color [5].
Differential Diagnosis
Tinea capitis lesions can be frequently confused with other common dermatologic scalp disease such as alopecia areata, seborrheic dermatitis, psoriasis, and bacterial folliculitis. In this particular presentation of tinea capitis, poliosis should also be included to the differential diagnosis.
Poliosis is defined as a localized patch of depigmented white hairs regardless of etiology. Poliosis has also been described as "white forelock" when its location involves the frontal scalp, however, poliosis can involve various body areas including the eyebrows, beard, and body site [6,7].
Poliosis can be associated with various genetic diseases such as Waardenburg, piebaldiam, tuberous sclerosis, in addition, poliosis has been described in association with various acquired conditions such as sarcoidosis, vitiligo, and Vogt-Koyanagi-Harada [8]. Medication such as Chloroquine, Cetuximab have been reported to cause poliosis [7].
Looking at the patient's earlier visit records, it seems that he had a mild hair loss at his initial presentation with the tinea capitis 6 months earlier and had no hair loss on the current visit, only the white hair patch, therefore, alopecia areata appeared to be a remote possibility. Seborrheic dermatitis and psoriasis are usually characterized by patchy scaling to widespread, thick crusts over erythematous inflamed skin. Lastly, the possibility of a drug or a chemical-induced skin reaction was entertained, however, there were no history suggestive of applying topical product including bleach or using medications.
It appears that our patient has developed poliosis as a consequence of the initial tinea capitis, a rare presentation of this type of fungal infection leading to the regrowth of a rather depigmented hair patch.
Patient Course
The scalp fungal culture that was obtained during this visit (6 months after initial infection) was negative, however, there was no initial scalp fungal culture obtained at the time of the initial diagnosis of tinea capitis as the clinical features then appeared to be consistent with the diagnosis. At 12th month following the original tinea capitis infection, the discolored white hair patch continued to improve as those white hairs were being replaced with a mixture of both more grayish colored hair mixed with the naturally colored hair. Parents were advised to continue supportive care and monitor for further restoration of the original hair color.
References
- Abdel-Rahman SM, Herron J, Fallon-Friedlander S, et al. (2005) Pharmacokinetics of terbinafine in young children treated for tinea capitis. Pediatr Infect Dis J 24: 886-891.
- Sharma V, Hall JC, Knapp JF, et al. (1988) Scalp colonization by Trichophyton tonsurans in an urban pediatric clinic? Asymptomatic carrier state. Arch Dermatol 124: 1511-1513.
- Elewski BE (2000) Tinea capitis: a current perspective. J Am Acad Dermatol 42: 1-20.
- Skin disorders due to fungi (2011) In: Paller AS, Mancini AJ, Hurwitz Clinical Pediatric Dermatology: A Textbook of Skin Disorders of Childhood and Adolescence. (4th edn), Elsevier Saunders, Philadelphia, PA, USA, 390-415.
- G Sentamilselvi, C Janaki, Sundaram Murugusundram (2009) Trichomycoses. Int J Trichology 1: 100-107.
- Sleiman R, Kurban M, Succaria F, et al. (2013) Poliosis circumscripta: overview and underlying causes. J Am Acad Dermatol 69: 625-633.
- Rodriguez NA, Ascaso FJ (2011) Trichomegaly and poliosis of the eyelashes during cetuximab treatment of metastatic colorectal cancer. Journal J Clin Oncol 29: e532-e533.
- Pan D, Hirose T (2011) Vogt-Koyanagi-Harada syndrome: review of clinical features. Semin Ophthalmol 26: 312-315.
Corresponding Author
Ahdi Amer, MD, Associate Professor, The Carman and Ann Adams Department of Pediatrics, Children's Hospital of Michigan, Pediatric Specialty Center, Wayne State University School of Medicine, Detroit, MI, USA.
Copyright
© 2017 Amer A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.