Bilateral Abducens Nerve Palsy due to Pseudotumor Cerebri in a Patient Taking Valproic Acid and Quetiapine: Report of a Case
Abstract
Purpose
To present a case of bilateral abducens nerve palsy due to pseudotumor cerebri in a patient taking valproic acid and quetiapine.
Methods
Single case report.
Results
A 32-year-old overweight woman taking valproic acid and quetiapine because of bipolar disorder, admitted to the outpatient clinic with diplopia. She had not any other ophthalmic history. Ophthalmological examinations demonstrated esotropia in the left eye and papilledema in the both eyes. The abduction of both eyes was insufficient. CSF analysis revealed an extremely high pressure (28 mmHg) with normal CSF indices. These findings indicated that the patient had pseudotumor cerebri (PTC) that caused bilateral incomplete abducens nerve palsy with papilledema. The patient was discharged with oral acetazolamide therapy and three months after papilledema and abducens palsy were regressed.
Discussion
PTC is associated with abducens nerve palsy; but there was a few report of bilateral abducens nerve palsy due to PTC. So, we aim to report this case because of a rare condition that bilateral abducens nerve palsy due to PTC due to valproic acid and quetiapine.
Keywords
Abducens nerve palsy, Pseudotumor cerebri, Quetiapine
Introduction
Pseudotumor cerebri (PTC) is a condition characterized by increased intracranial pressure without intracranial space occupying lesions or hydrocephaly. It is characterized by headaches and bilateral optic disc edema in classical cases. Temporary vision loss and diplopia can be seen. Neurological symptoms are rare apart from the sixth nerve palsy. However, rare neurological cases have been reported [1-6]. PTC is usually seen in young to middle-aged women and often idiopathic. We report a case of PTC with bilateral abducens nerve palsy in a patient taking valproic acid and quetiapine for bipolar disorder.
Case Presentation
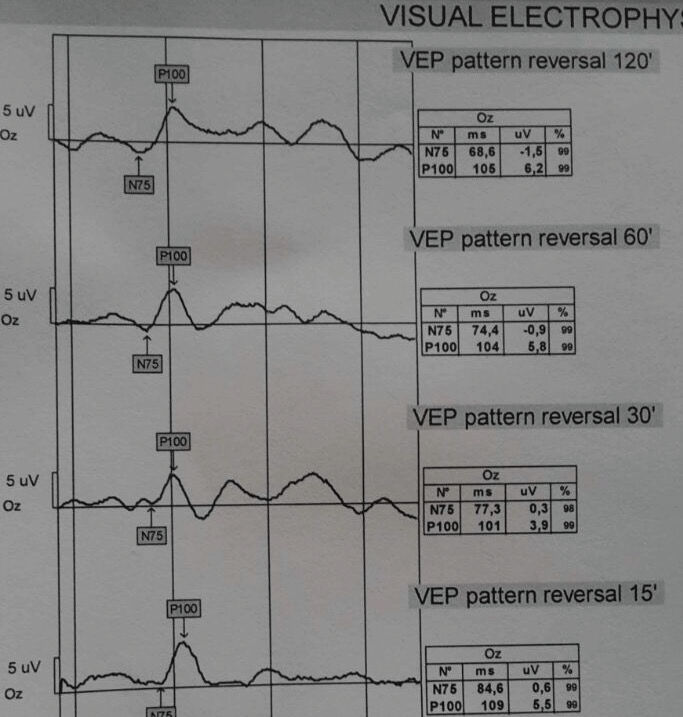
A 32-year-old overweight woman admitted to the outpatient clinic with diplopia for 3 months. She had not any other ophthalmic disorders, ocular surgery or trauma. On examination her vision was 20/20 in both eyes. Esotropia was present the left eye in primary gaze. On neurological examination, the abduction of both eyes was insufficient (left 3/5, right 3/5). Her pupils were symmetric and reactive to light. She had no other cranial neuropathy, no motor or sensory deficits, and no pathological reflexes. Ophthalmological examinations demonstrated bilateral papilledema. The patient�s color discrimination, visual fields were normal. Amplitude and latency of visual evoked potential (Figure 1) were normal.
A full blood count was normal. Brain magnetic resonance imaging (MRI) and computed tomography (CT) showed no findings of mass lesions, hydrocephalus, ischemia, thrombosis or vasculitis. She was taking valproic acid (750 mg) and quetiapine (600 mg) for bipolar disorder for about one and a half years. She was obesity and she gained approximately 40 pounds during this period of topiramate therapy for about ten years. She was not taking topiramate for 2 years. CSF analysis revealed an extremely high pressure (28 mmHg) with normal CSF indices. There was no evidence of malignancy or infection. These findings indicated that the patient had PTC that caused bilateral incomplete abducens nerve palsy with papilledema. She was hospitalized and she was given oral acetazolamide 250 mg 6 hourly. Quetiapine dose was reduced to 300 mg, on the grounds that increase the edema, with psychiatric clinic of the proposal. The patient was discharged with oral acetozalamide therapy. Three months after, her examination, papilledema was regressed and both eyes were 1/5 insufficient. The last examination, after one year, on examination 20/20 in both eyes. Papilledema was regressed and both eyes were 1/5 insufficient, too. She was taking oral acetozalamide 250 mg 6 hourly and she was taking valproic acid and quetiapine for bipolar disorder.
Discussion
PTC was defined by the modified Dandy criteria: 1-Symptoms and signs that may be related to increased intracranial pressure (headache, papilledema, etc), 2-Although the structure of CSF is normal, opening pressure of LP higher than 25 cm H2O, 3-Normal neurological findings except 6th nerve palsy and 4-The absence of space occupying lesion neuroradiologically 5-No other cause of increased intracranial pressure (ICP) identified [7]. The pathophysiology of PTC is not clear. Several risk factors have been reported such as obesity, arterial hypertension, anemia, Addison�s disease, hypothyroidism, hyperthyroidism, uremia, including excessive dosages of some exogenously admin�istered medications (e.g., vitamin A, tetracy�cline, minocycline, nalidixic acid, corticoster�oids), blood dyscrasias, and chronic respiratory insuf�ficiency [8,9].
Abducens nerve palsy is the most common cause of the isolated ocular motor nerve palsies. Patients usually present with binocular horizontal diplopia worse in the distance, and esotropia in primary gaze. Patients also may present with a head-turn to maintain binocularity and binocular fusion and to minimize diplopia. Acquired abducens nerve palsies can be due to trauma, neoplasm, inflammation, and idiopathic etiologies. The sixth nerve is affected frequently in head trauma due to its course of close to the orbital lateral wall and placement in the cavernous sinus. In advanced age, among the reasons for the sixth nerve palsy it is frequently in the vascular pathology as well as the trauma. Rush and Younge reported that the most common cause of abducens nerve palsy was the vascular pathology and trauma. Rush reported that the most frequency etiologic factors in abducens nerve palsy was vascular pathologies in another study involving 277 patients [10-13]. The sixth cranial nerve palsy is rare in young adults but when the abducens nerve palsy is occurred in younger adults, it must be considered a serious underlying pathology. Moster reported that the etiologies of abducens nerve palsy in the study consisting of 49 patients, aged from 15 to 50 years, were vasculopathy 29%, tumors 16% multiple sclerosis 12% [14]. Peter, et al. reported that the most common cause for a sixth nerve palsy in the young adults was a central nervous system mass lesion, although the most common cause for an isolated sixth nerve palsy in this age group was multiple sclerosis [15]. In our case, we thought that bilateral sixth nerve palsy developed secondary to increased intracranial pressure.
Cranial nerve palsies have been reported in PTC by authors with abducens nerve palsy in 10% to 20% of cases [16,17]. There is lot of reports on PTC with unilateral abducens nerve palsy; but there was unique report bilateral abducens nerve palsy due to PTC as the onset of systemic lupus erythematosus [18].
Uddin reported a case in which a patient on chronic valproic acid therapy for a seizure disorder developed PTC [19]. He claimed to changing his antiepileptic medication from valproic acid to topiramate effected a remission of PTC symptoms while maintaining his seizure-free status. In this case, the patient was obesity. Obese women present a significant cohort of PTC; but she gained approximately 40 pounds during topiramate therapy for about 10 years. For 2 years she was not taking topiramate. She was taking valproic acid and quetiapine for bipolar disorder for about one and a half years. Also she diagnosed with PTC 4 months after valproic acid in usage. There was evidence of that quetiapine may produce ocular toxicity [20]. So, we thought it might be due to the use of valproic acid and quetiapine in these patient caused PTC. We aim to report this case because of a rare condition that bilateral abducens nerve palsy due to PTC with valproic acid and quetiapine.
References
- Dandy WE (1937) Intracranial pressure without brain tumor: diagnosis and treatment. Ann Surg 106: 492-513.
- Weisberg LA (1985) Computed tomography in benign intracranial hypertension. Neurology 35: 1075-1078.
- Kesler A, Yaffe D, Shapira M, et al. (1996) Optic nerve sheath enlargement and reversal of optic nerve head in pseudotumor cerebri. Harefuah 130: 457-459.
- Brodsky MC, Vaphiades M (1998) Magnetic resonance imaging in pseudotumor cerebri. Ophthalmology 105: 1686-1693.
- Gass A, Barker GJ, Riordan-Eva P, et al. (1996) MRI of optic nerve in bening intracranial hypertension. Neuroradiology 38: 769-773.
- Hamurcu M, Sarıcaoğlu MS, Koca S, et al. (2015) Visual evoked potential and optical coherence tomography in pseudotumor cerebri. Research 2: 1476.
- Thurtell MJ, Wall M (2013) Idiopathic intracranial hypertension (pseudotumor cerebri): recognition, treatment and ongoing management. Curr Treat Options Neurol 15: 1-12.
- Corbett J (2012) Idiopathic intracranial hypertension. J Neuroophthalmol 32: e4-e6.
- Victorio MC, Rothner AD (2013) Diagnosis and treatment of idiopathic intracranial hypertension (IIH) in children and adolescents. Curr Neurol Neurosci Rep 13: 336.
- Rush JA, Younge BB (1981) Paralysis of cranial nerves III, IV and VI cause and prognosis in 1000 case. Arch Ophthalmol 99: 76-79.
- Richards BW, Jones FR, Younge BR (1992) Cause and prognosis in 4278 cases of paralysis of the oculomotor, trochlear and abducens cranial nerves. Am J Ophthalmol 113: 489-496.
- Rucker CW (1966) The causes of paralysis of the third, fourth and sixth cranial nerves. Am J Ophthalmol 61: 1293-1298.
- Rush JA (1992) Cause and prognosis in 4278 cases of paralysis of the oculomotor, trochlear and abducens cranial nerves. Am J Ophthalmol 114: 777-778.
- Moster ML, Savino PJ, Sergott RC, et al. (1984) Isolated sixth nevre palsies in younger adults. Arch Ophthalmol 102: 1328-1330.
- Peters GB 3rd, Bakri SJ, Krohel GB (2002) Cause and prognosis of nontraumatic sixth nerve palsies in young adults. Ophthalmology 109: 1925-1928.
- Bakshi SK, Oak JL, Chawla KP, et al. (1992) Facial nerve involvement in pseudotumor cerebri. J Postgrad Med 38: 144-145.
- Brackmann DE, Doherty JK (2007) Facial palsy and fallopian canal expansion associated with idiopathic intracranial hypertension. Otol Neurotol 28: 715-718.
- Katsuyama E, Sada K, Tatebe N, et al. (2016) Bilateral abducens nerve palsy due to idiopathic intracranial hypertension as an initial manifestation of systemic lupus erythematosus. Intern Med 55: 991-994.
- Uddin AB (2003) Drug-Induced Pseudotumor Cerebri. Clin Neuropharmacol 26: 236-238.
- Yabe I, Moriwaka F, Notoya A, et al. (2000) Incidence of idiopathic intracranial hypertension in Hokkaido, the northernmost island of Japan. J Neurol 247: 474-475.
Corresponding Author
Mualla Şahin Hamurcu, MD , Ankara Numune Eğitim ve Araştırma Hastanesi, Talatpaşa Bulvarı No: 44 06230 Altındağ/Ankara, Turkey.
Copyright
© 2016 Hamurcu MS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.