Torsion of the Greater Omentum as a Rare Cause of Acute Abdomen: A Case Report and Review of the Literature
Abstract
Background
Torsion of the greater omentum is a highly uncommon cause of acute abdomen in adults and is extremely difficult to diagnose preoperatively. Usually it mimics other surgical emergencies such as acute cholecystitis, acute appendicitis, perforated peptic ulcers and acute diverticulitis and can be easily misdiagnosed leading to deterioration of the patient. Around 300 cases have been reported in the literature and only 26 of them were treated laparoscopically.
Case presentation
This is the case of a 46-year-old Greek woman who presented herself with abdominal pain of acute onset located in the Right Upper Quadrant (RUQ) of her abdomen without any other symptoms. The clinical diagnosis was acute cholecystitis while the Computed Tomography (CT) displayed acute diverticulitis of the sigmoid colon. However, during diagnostic laparoscopy omental torsion was found and was treated with omentectomy.
Conclusion
Greater omental torsion is a very complex diagnosis. A high degree of clinical suspicion is necessary in cases of patients with acute abdominal pain, normal laboratory results and inconclusive imaging studies. The treatment of choice for omental torsion is surgical excision of the necrotized tissue, preferably done laparoscopically.
Keywords
Acute abdomen, Omental torsion, Laparoscopy
Abbreviations
RUQ: Right Upper Quadrant; CT: Computed Tomography
Introduction
Torsion of the greater omentum is a very rare condition in which the organ rotates around its long axis, compromising its vascularity to such a degree that can cause infraction and necrosis [1]. Omental torsion can be primary (Idiopathic) or secondary, relating to the presence of intra-abdominal pathology [2]. Since Eitel described the first primary omental torsion in 1899, around 300 cases have been reported in literature, but only few of them have been correctly diagnosed preoperatively and only 26 of them have been treated laparoscopically with omentectomy, with Valioulis, et al. being the first publishing images of laparoscopic omentectomy performed on a 13-year-old boy and on a 8-year-old girl in 2003 [3-6].
In this article we analyze the case of a 46-year-old Greek woman who presented at our emergency room with clinical symptoms of acute cholecystitis while imaging studies suggested diverticulitis of the sigmoid colon. The patient was subjected to diagnostic laparoscopy where omental torsion and necrosis was found and was treated with omentectomy. Due to the scarceness and the difficulty of the diagnosis and the mismatching of clinical symptoms and imaging findings we present the current aspects of diagnosis and treatment of omental torsion.
Case Presentation
A 46-year-old Greek woman presented at the emergency department complaining about abdominal pain of acute onset located at her RUQ having started 24 hours ago, without any other accompanying symptoms. The patient had a history of arterial hypertension treated with a combination of amlodipine and valsartan and hypothyroidism treated with levothyroxine sodium. She was also subjected to surgical reconstruction of a bicornuate womb 15 years ago. A physical examination revealed rigid pain in the right part of her abdomen, especially in the RUQ, with a positive Murphy's sign and rebound tenderness. Her abdominal sounds were present but diminished while her vital signs were normal.
Her laboratory findings were all normal except for a slight increase in the neutrophils (82.2% with normal range 45-75%) but with normal white blood cells (9960/μl with normal range 3800-10500/μl). The chest and abdominal X-rays revealed no abnormal findings. The abdominal CT scan revealed diverticulitis of the sigmoid colon and a slight distortion of the peritoneal fat around the hepatic flexure of the colon.
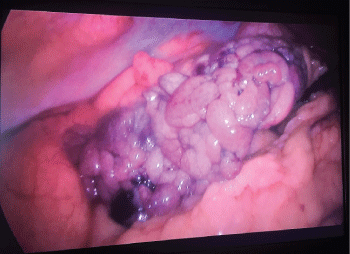
Due to the intensity of the clinical signs, the deterioration of the symptoms and the mismatch between the clinical signs and the imaging findings the patient was subjected to diagnostic laparoscopy. The patient was placed in a split-leg position with the surgeon standing between her legs, the assistant on the right and the scrub nurse on the left. Firstly, a 10 mm umbilical port was created through which the laparoscope was inserted. A second 12 mm port was created in the left iliac fossa and a third 5 mm port on the right midclavicular line in the right iliac fossa. The procedure revealed that a portion of the patient's omentum located in the right part of her abdomen had twisted several times in a clockwise direction resulting in vascular obstruction and necrosis (Figure 1). A thorough examination of the abdominal cavity was conducted, which revealed no other abnormalities in the remaining intra-abdominal organs.
The procedure proceeded with restoration of the twisted omentum and excision of its necrotic part. As an energy source for hemostasis and excision a 5 mm - 37 cm Ligasure device with a dolphin tip was used. The patient recovered safely with immediate resolution of her symptoms and was discharged on the second postoperative day without any complications.
Discussion
Omental torsion is a very rare cause of acute abdomen in adults, which usually mimics more common pathologies that present themselves with acute abdominal pain [7]. Omental torsion consists of 1.1% of all cases of abdominal pain and its incidence is between 0.0016% and 0.37%. When compared with acute appendicitis, it has a ratio of 4 per 1000 cases [1,2,8]. This condition is more commonly encountered in middle-aged males between their third and fifth decade of life [1].
Omental torsion usually develops as the omentum twists clockwise around a proximal fixed point on its long axis [1,9]. The commonest point of torsion is around the distal right epiploic artery because of the greater length and mobility of the omentum on the right side of the body [5,9,10]. As a consequence, venous blood flow is obstructed resulting in vascular congestion and edema [1,5,10]. As the condition progresses, arterial blood flow is compromised, leading to ischemic necrosis of the affected part of the omentum and multiple adhesions formation [4,10].
Omental torsion can either be primary or secondary [7]. Primary torsion, which forms one third of the cases [11] occurs when there is no associated intra-abdominal pathology [10,12]. Secondary torsion occurs as a result of pre-existing intra-abdominal pathologies such as inguinal hernias (most common), cysts, tumors, foci of intra-abdominal inflammation and postsurgical wound or scarring [1,3]. Regarding primary omental torsion, although its etiopathogenesis has not been fully understood yet, many predisposing factors have been described [4]. These include anatomical malformations of the omentum, bifid omentum, irregular distribution of omental fat associated with obesity, narrowed omental pedicle and redundancy of omental veins, which creates fixation points around the shorter and tenser arteries where the omental segment can twist [1,11]. Initiating mechanisms of torsion include conditions that cause omental displacement such as rigorous exercise, sudden cough, abdominal trauma, pregnancy and hyperperistalsis [4,13]. In this article, we report a case of a 46-year-old female patient with omental torsion who did not have any of the above mentioned predisposing and precipitating factors.
Omental torsion presents with non-specific clinical features, thus, it is very difficult to be diagnosed preoperatively [4,10]. Most patients usually present with unremitting abdominal pain of acute onset located in the right iliac fossa, similar to acute appendicitis [1,4,11]. Less often, pain is located in the RUQ, mimicking acute cholecystitis, as in our case [4,13]. The pain may be accompanied with nausea vomiting and low-grade fever, while intestinal movement is preserved [4,10]. Physical examination usually reveals tenderness with signs of localized peritonitis or a palpable abdominal mass [1,4,13]. Depending on age and localization of the pain, differential diagnosis should also include acute diverticulitis, gastroduodenal ulcer, epiploic appendagitis, gynecological diseases and other intra-abdominal inflammatory conditions [10].
Laboratory results in omental torsion are usually normal or show a slight increase in inflammation parameters [10,13], as it was in our case. Advances in imaging techniques with CT scan can help diagnose omental torsion preoperatively [8], by revealing the characteristic findings of a whirling fatty and fibrous mass around a vascular pedicle, a fatty mass with a whirling pattern, spiral fat pattern or a circumscribed fatty mass with hyper-attenuated streaks and a concentric distribution of fibrous folds [1,4,8,10,13]. However, not every omental torsion case reported in the literature showed such characteristic findings due to the axis of rotation not being perpendicular to the transverse scanning plan [10]. In our case, we had no evidence of omental torsion in the CT scan, which instead revealed false positive signs for diverticulitis of the sigmoid colon.
In the literature, both conservative and surgical management of omental torsion has been reported [1,5,8,12]. However, surgical treatment still remains the procedure of choice [10,13], since it results in faster recovery, shorter hospital stay and prevents possible complications such as sepsis, intra-abdominal abscesses or adhesion formation [5,12,13]. The operation can be performed either with a laparotomic approach or laparoscopically and involves the resection of the affected part of the omentum [1]. Laparoscopy is the procedure of choice both for diagnostic purposes and for all the benefits of minimal access surgery [11,14] and, thus, it was the procedure we opted for in our case.
Conclusion
Omental torsion is a highly uncommon cause of acute abdomen and is very difficult to diagnose preoperatively. It presents with non-specific symptoms, mimicking other abdominal pathologies. CT scan may be helpful, but typical signs are not always present. Surgical treatment is the procedure of choice with laparoscopy being the preferable approach. A high index of clinical suspicion is required, especially when clinical symptoms and imaging studies do not match.
References
- A Kumar, J Shah, P Vaidya (2016) Primary omental gangrene mimicking appendicular perforation peritonitis-A case report. Int J Surg Case Rep 21: 67-69.
- S Occhionorelli, M Zese, L Cappellari, et al. (2014) Acute Abdomen due to Primary Omental Torsion and Infarction. Case Rep Surg 2014: 208382.
- Ghosh Y, Arora R (2014) Omental torsion. J Clin Diagn Res 8: 1-2.
- Alexiou K, Ioannidis A, Ioannis D, et al. (2015) Torsion of the greater omentum: two case reports. J Med Case Rep 9: 160.
- Janny Lizbeth Zaleta-Cruza, Javier Rojas-Mendeza, Ulises Garza-Serna, et al. (2017) Omental torsion. Case Report. Cir Cir 85: 49-53.
- Valioulis I, Tzallas D, Kallintzis N (2003) Primary Torsion of the Greater Omentum in Children. A Neglected Cause of Acute Abdomen? Eur J Pediatr Surg 13: 341-343.
- Chul Min Park, Sung Yob Kim (2014) Primary omental torsion diagnosed during hysterectomy. Obstet Gynecol Sci 57: 415-418.
- Mendoza Moreno F, Diez Gago Mdel R, Cordova García DM, et al. (2016) Primary omental torsion as presentation of acute abdomen. Case report. Rev Esp Enferm Dig 108: 105-106.
- Joshi S, Cuthbert GA, Kerwat R (2016) Omental torsion, a rare cause of acute abdomen. BMJ Case Rep.
- Jun-Sik Yu, Woo-Surng Lee, Yong-Hun Kim (2016) Primary Torsion of Lesser Omentum Presented with Acute Abdomen and Successfully Managed with Laparoscopic Surgery. Chin Med J 129: 1625-1626.
- Vijay Borgaonkar, Sushil Deshpande, Mukesh Rathod, et al. (2013) Primary Omental Torsion Is a Diagnostic Challenge in Acute Abdomen-a Case Report and Literature Review. Indian J Surg 75: 255-257.
- Anyfantakis D, Kastanakis M, Karona V, et al. (2014) Primary omental torsion in a 9 year old girl: a case report. J Med Life 7: 220-222.
- Dhooghe V, Reynders D, Cools P (2016) Torsion of a bifid omentum as a rare cause of acute abdomen: a case report. J Med Case Rep 10: 289.
- Ali Tasleem, Qamar Zaman, Daniel A Thomas, et al. (2013) Omental Torsion: An Unusual Cause of Right Iliac Fossa Pain and Role of Laparoscopic Management. Gastroenterology Res 6: 237-239.
Corresponding Author
Georgios Koimtzis, 3rd Department of Surgery, University Hospital of Thessaloniki AHEPA, Aristotle University of Thessaloniki (AUTH), 19 Nathanail Str., Thessaloniki, Greece, Tel: +30697187924.
Copyright
© 2017 Kosmidis C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.