Comparison of Single-Port and Multi-Port Laparoscopic Methods of Nephrectomy in Young Infants
Abstract
Background
The aim of this study was to compare results of treatment of non-functioning kidneys in neonates and infants using Single-Incision Laparoscopic Nephrectomy (SIL-N) and multi-ports laparoscopy.
Materials and methods
Between January 2013 and December 2016 we have performed 18 nephrectomies for non-functioning kidneys with use of single-incision laparoscopy (Group 1) and 17 operations by means of multi-port laparoscopic technique (Group 2). For implementation a SIL-N in young babies a new technological platform was developed taking into account anatomical and physiological features of the infant body like selection of beneficial access, equipment and practical skills. The analysis of demographic data, intra-and postoperative parameters, immediate and late effects of the procedures, was performed at the final stage of the study.
Results
There were no differences in the pre- and postoperative parameters between the two groups. The compared groups were similar in terms of demographics parameters (diagnosis, age, gender and weight). The mean operative time in Group 1 was 43.33 min. In contrast, the mean duration of the operation in the Group 2 was 48.33 min (p = 0.378). The mean dose of analgesia in Group 1 was 3.67. In contrast, the mean quantity of analgetic doses in the Group 2 was 3.58. Length of postoperative hospital stay was identical in patients of both groups (3 days vs. 2.91 days; p = 0.779). The postoperative course and follow up was uneventful in the all patients. We did not register any complications of the procedure such as hematoma of the bed of the removed kidney or wound infection in the early postoperative period. Follow-up (from 1 month to 1 year) of patients showed no negative effects of nephrectomy that was performed by using a single-incision technique.
Conclusion
The results of this study demonstrate that single incision vs. multiport nephrectomy on non-functioning kidneys in infants are equally effective.
Keywords
Neonates, Infants, Nephrectomy, Single-incision laparoscopic surgery
Minimally invasive surgery is becoming an increasingly common treatment for various urological diseases in children. For patients with non-functioning kidneys, a laparoscopic procedure is a safe and effective alternative to traditional open surgery, and accompanied by the following benefits: rapid recovery of patients after procedure, less postoperative pain and a good cosmetic result [1-3].
The world around us is constantly changing and beauty standards are also changing. More often, patients and their parents are wondering, not only about the effectiveness of a procedure, but also about its cosmetic result. Overcoming these limitations and difficulties, some laparoscopic surgeons have been able to minimize a surgical incision for the removal of a kidney and that has become invisible and hidden in the umbilical fold. Recent technological progress expanded the surgical opportunities for nephrectomy to Single-Incision Laparoscopic Surgery (SILS), which is also known as Single-Incision Pediatric Endosurgery (SIPES). The desire of cosmetic perfection is a challenge for the surgeon, requiring him to utilize innovative manipulation techniques, instruments, and devices for their application in the peritoneal cavity. The number of publications about SIPES method for nephrectomy in young infants is considerably low and limited by the number of cases [4-12].
A single-port laparoscopic approach for nephrectomy is not widely used in newborns and infants. Primarily, this is due to the fact that the majority of pediatric surgeons are satisfied with the cosmetic results of the multi-port endoscopic techniques. Another explanation of this phenomenon is the lack of technology and practical skills to implement a SIPES in small babies. The aim of this study was to compare a result of treatment of non-functioning kidneys in neonates and infants using Single-Incision Laparoscopic Nephrectomy (SIL-N) and multi-ports laparoscopy.
Materials and Methods
Between January 2013 and December 2016 at the Irkutsk Neonatal Surgical Center (Russia) a total of 35 children underwent a laparoscopic nephrectomy. The design of this study was retrospective cohort study. We have compared of 18 cases of non-functioning kidneys with using single umbilical incision (Group 1) and 17 cases of this condition repaired through standard three separate ports laparoscopic technique (Group 2). The indications for nephrectomies were the following: congenital Multi Cystic Dysplastic Kidney (MCDK) in 29 patients and terminal hydro nephrosis in 6 patients. The diagnosis for a nonfunctioning kidney was established on the data obtained from ultrasound diagnostics, contrast X-ray and radio isotope studies. The size of the non-functioning kidneys varied from 45 to 90 mm. Cases on the right side were equivalents in the compared groups (R/L: 9/9 vs. 8/9). Relatively larger liver in small babies wasn't a barrier for manipulation during single-incision surgery and didn't lead to installation of additional laparoports and conversion to multi-ports laparoscopy.
Surgical procedures included the standard laparoscopic nephrectomy as originally described by R. Erlich [1] and modern SIL-N technique that described here. All operations were performed by a single surgeon with established background in standard pediatric Minimally Invasive Surgery (MIS) procedures. To perform a single-incision laparoscopic nephrectomy in 3-month-old infants a new technological platform was developed taking into account anatomical and physiological features of the infant body like selection of beneficial access, equipment and practical skills.
Technique of a SIL-N
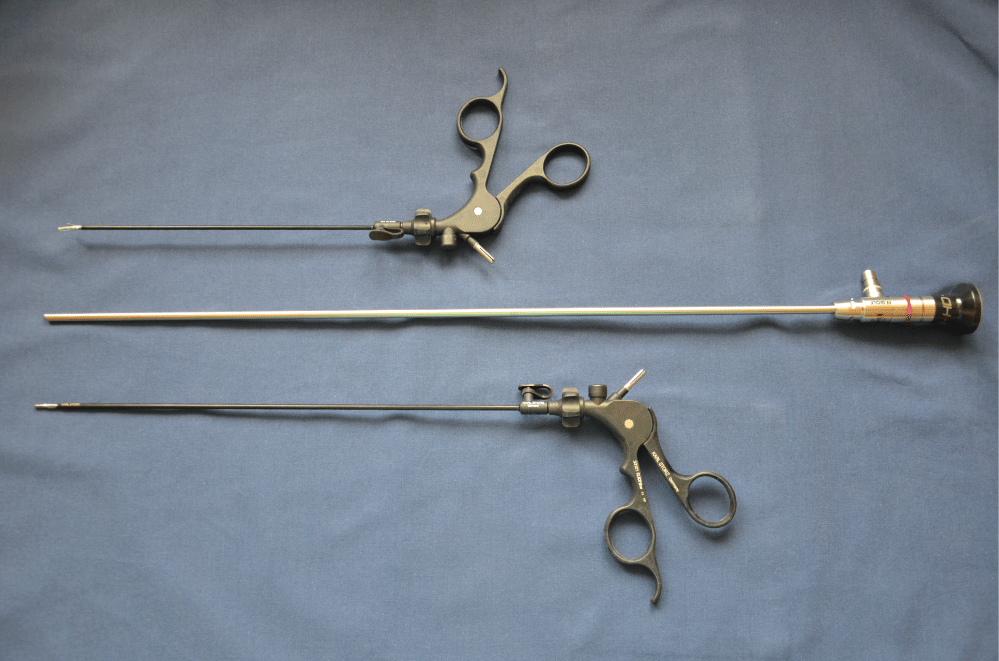
The TriPort® (Advanced Surgical Concepts, Olympus) insertion began by performing a skin and aponeurotic incision in the umbilical area. Then, a distal inner ring of the port system and a silicone sleeve were inserted into the abdominal cavity by using a special introducer. Subsequently, they were joined with the proximal upper ring that was positioned externally on the abdominal wall. After implementation of the outside traction of the inner ring, the excess of the silicone sleeve was cut off and was fixated to the outer ring by a lock. The upper ring is apaddevice that includes the gel ports designed for installation of instruments with a diameter from 2 to 5 mm, the optical system, and the side port for insufflation of Carbon dioxide (CO2). A carbo peritoneum was established in the abdominal cavity by using a constant flow of CO2 under pressure of 8 mmHg. We used a 5 mm endoscope with a length of 45 cm and conventional straight 3 mm instruments with different lengths 20 and 30 cm (Figure 1) to avoid their handles' collision when working outside of the abdominal cavity were inserted through the separate channels of port system.
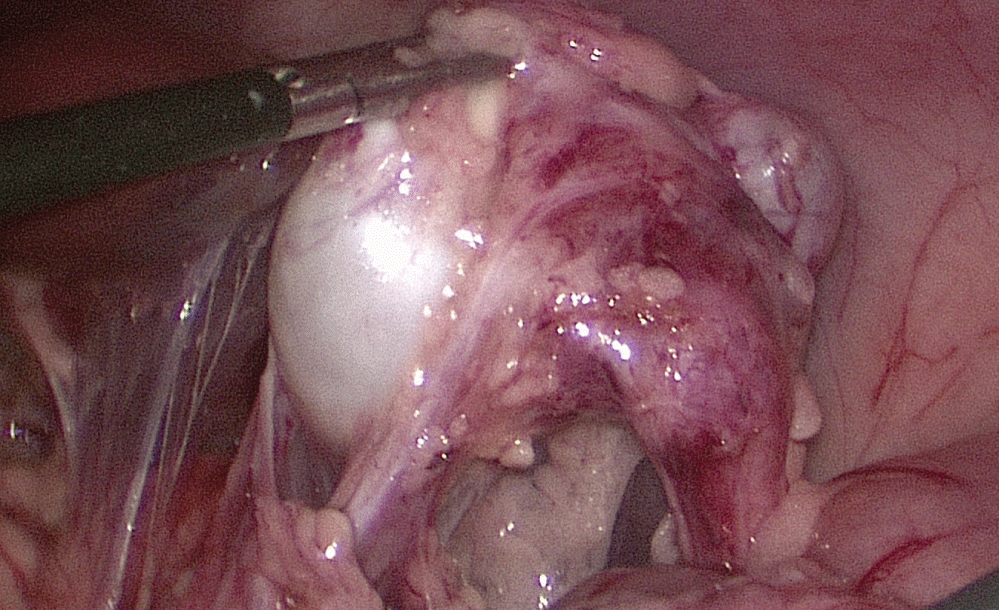
An innovative technique of "cross" manipulation, which was developed to improve the maneuverability of ordinary direct instruments, was utilized. The crossing of the hands with this technique leads to that left hand of the surgeon must manipulate the endoscopic grasper on the right, and the right surgeons hand operate the coagulator and dissector on the left. The kidney that will be to remove was inspected. The peritoneum was incised through the Toldt's line. The Gerota's fascia was dissected and the kidney with renal vessels and ureter were freed (Figure 2). The renal arteries and veins were clipped or ligated by using BiClamp technology (ERBE VIO 300D, Erbe Elektromedizin). The ureter was mobilized and transected at the level of falling into the bladder with the Roeder loop ligature of the distal paravesical segment. Content of cysts or renal pelvis was aspirated with a needle puncture. The kidney was removed through the umbilical incision simultaneously with the TriPort®-device removal. Suture of fascia and skin was performed at the end of the procedure. Analgesia for all patients consisted of acetaminophen given at a dose of 10 mg/kg orally per rectum as needed for absence a pain.
The analysis of demographic data, intra- and postoperative parameters, immediate and late effects of the procedures, was performed at the final stage of the study. The two groups were compared for patients' demographics, operative report and postoperative outcomes. All the variables were stored in a database and analyzed. Pre- and postoperative parameters were compared statistically using analysis of Mann-Whitney U-test for age and weight before surgery, operative time, doses of analgesia and postoperative length of hospital stay. A P value of less than 0.05 was considered statistically significant.
Results
The differences of age and body weight in the groups were not statistically significant (Table 1). Timing of surgery was similar (94.33 day vs. 75.5 day, p = 0.319). The average weight of the patients from Group 1 was 5.64 kg, and that of the patients in group 2 was 5.17 kg (р = 0.562). The gender composition of patients presented was identical (m:w-10:8 and 9:8, p = 1.0). The operative times were nearly identically between 2 approaches with a mean duration of the operation of 43.3 minutes in the SIL-N group compared with 48.33 minutes in the Group 2 (p = 0.378).
There was no significant blood loss during the procedures. Recovery was uneventful in all patients. The mean doses of analgesia in Group 1 were 3.67. In contrast, the mean quantity of analgetic doses in the Group 2 was 3.58. The average length of hospital stay was 3 days and 2.91 days respectively (p = 0.799).
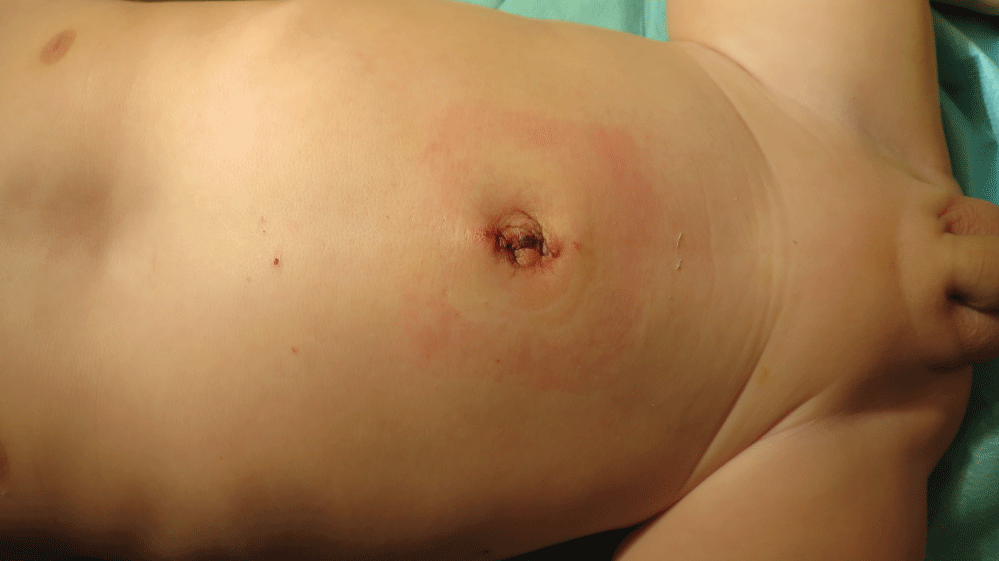
We did not register any complications of the procedures such as hematoma of the bed of the removed kidney or wound infection in the early postoperative period. Follow-up (from 1 month to 1 year) of patients showed no negative effects of nephrectomy that was performed by using a single-multi-port laparoscopic technique. The single umbilical scar was invisible after a few weeks. It was hidden in the umbilical fold (Figure 3). The evidence of use of the additional instrumental laparoports was visible at repeated surveys of the abdominal wall.
Accomplishment of the learning curve was associated with improved outcomes such as decreased operation time. The operative time after SIL-N continually decreased, with the most dramatic reduction achieved following the 8th patient till 40 minutes. Thus overcoming the learning curve is manifested by decreased operative time in single-incision subgroup enough patients and also confirmed our assumption of the fast period of mastering of SIPES technologies.
The results of our study demonstrate that use of a SIPES technique for removal of a non-functioning kidney in infants provides good recovery of patients after surgery that resulted in similar to standard laparoscopy perioperative parameters such as duration of the operation, doses of analgesia, length of hospital stay. In addition, a positive argument in favor of a single-incision nephrectomy is a sustained excellent cosmetic result. The single umbilical scar was invisible after few weeks. The marks from additional laparoports were visible all time during examination of patients at 1, 3, 6 and 12 months after discharge from the pediatric hospital.
Discussion
Nephrectomy in children is a method of surgical treatment of kidney diseases for removing a non-functioning kidney. This procedure is commonly performed in neonates and infants. Some of the indications for nephrectomy are the following: vesicoureteral reflux, obstructive uropathy, MCKD, and urolithiasis [2]. Less common, nephrectomy is used for the treatment of older children to remove a kidney, which is affected by malignant neoplasm. The open nephrectomy, when the surgeon makes an incision in the side of abdomen or dorsal lumbotomy approach has been considered a standard procedure for many years.
Currently, open nephrectomy has been replaced by a laparoscopic procedure, which has minimal traumatic effect on patients' tissues and has better cosmetic results. The first laparoscopic nephrectomy in an adult patient was performed by R. Clayman [13]. Then R. Erlich [1] repeated this success by performing the minimally invasive nephrectomy in a child. For a long time, multicystic kidney dysplasia was the most common reason for a laparoscopic nephrectomy, while J. Valla [3] expanded the indications for this procedure, but considered it only for benign kidney diseases, such as: multicystic kidney dysplasia, a non-functioning kidney due to reflux nephropathy and obstructive uropathy from urolithiasis, which, sometimes, is a cause of uncontrolled hypertension. The reduction of the number of ports, designed to remove a kidney, contributed to the fact that laparoscopic nephrectomy has gradually become possible through a single tiny umbilical incision. In 2007, A. Rane was the first, who reported a kidney removal by utilizing a single-incision technique in adult patients [14]. Later Y. Park [5] and R. Johnson [4] reported about a single-incision nephrectomy in children. This research series, which included 4 to 11 pediatric patients, demonstrated the possibility of removing a kidney through a single laparoscopic approach [6-12]. The lowest average weight and age of patients in the scientific reports was 10.6 kg and 12 months, respectively [10]. Our results demonstrate the smaller weight and age of patients (5.64 kg and 3 months).
The employment of a SIPES technique in children was problematic due to unique technical problems associated with the inability to implement the principle of triangulation of instruments and collision of tools inside and outside of the abdominal cavity, with the requirement to use the innovative technologies for vessels' ligation.
The increased need for an optimal technological platform for single-port access led to the invention a significant number of multi-channel devices. However, the large size of multi-port systems required a fascial incision longer than 2-3 cm for its installation, which limits their employment in children. The exception is the TriPort® system (Advanced Surgical Concepts, Olympus), which requires a minimum fascial incision of 1.0-1.5 cm for its installation. Thus it is possible to perform complex SIPES procedures even in newborns.
Currently, the selection of instruments to perform a single-port surgery in children represents a major problem. The principle of triangulation of instruments is difficult to utilize. To overcome some inconveniences, we employed miniature clamps of different lengths (20 and 30 cm) and turned them on the axis by 180° to avoid the collision of the surgeon's hands and tool handles when using ordinary direct laparoscopic instruments. Finally, the HD-telescopes underwent a further evolution; their length was as high as 45 cm, which allowed better visualization and maneuverability in the port device, crowded by instruments.
Several basic technological principles for successful performance of a single-incision laparoscopic nephrectomy in infants have been formulated by us:
1. The principle of pre-operative planning of stages for a surgical procedure, based on diagnostic imaging studies: ultrasound scanning, excretory urography, multi-slice spiral computed tomography of kidneys, and radioisotope renography;
2. The principle of "cross-handed" instrumentation: instruments that are inserting into the infant body's cavity should form a crisscross angle that allows for manipulation of tissues;
3. The principle of tissue dissection - "pull & coagulate" with a preference to use a monopolar coagulation;
4. The principle of vessels sealing: use of Biclamp technology (ERBE Elektromediz in GmbH, Germany) for electro coagulation of renal arteries and veins.
Despite achievements of a single-incision surgery, its performance in infants is still limited. In one of the first reviews of literature about the SIPES technique in children, T. Ponsky [15] categorically denied the possibility of performing a single-incision surgery with infants during the first three months of life. The number of scientific publications about the SIPES technique in this age group is still small and mostly focused on the narrow range of diseases, where a single-incision surgery has demonstrated its effectiveness. In a recent review of literature, L. Saldan [16] analyzed all publications that were available on websites of the U.S. National Library of Medicine and the National Institutes of Health at http://www.ncbi.nlm.nih.gov.pubmed/ until March 2012 related to single-incision surgery in children. During this search he identified 4212 pediatric patients and only 99 of them were newborns.
The controversy surrounding the SIPES technique will not stop and is mainly concerned with the fact that many surgical procedures cannot be performed by employing single-incision laparoscopic surgery, particularly from the point of view of using the basic principle of endoscopy-triangulation [17]. The unique idea of SIPES consists in the concept of “cross-handed" instrumentation. At first time it can be uncomfortable. We must agree that the ergonomics with “cross-handed" approach creates additional difficulty. With increasing experience and improved technology, we received a comparable operative time.
Also, it remained unknown whether a single-incision technique is safe and effective endosurgical procedure for nephrectomy at young children. The early experience described in this study confirms that SIL-N can be applied for treatment of non-functioning kidneys in infants with outcomes similar to the standard laparoscopic surgery. One limitation of our research is non homogeneous groups of patients with non-functioning kidneys (MCDK and hydronephrosis). However this limitation is the general in pediatric surgery in which case volume and frequency of diseases are low.
Reliable data concerning the advantages of the SIPES technique does not exist due to weak evidence in most publications. No doubt, cosmetic superiority is one of the advantages of the SIPES technique, where the umbilicus is employed as a "keyhole" to hide a postoperative scar. The additional benefit of the umbilical incision is that it can be easily converted into a multi-port laparoscopy or in to an expanded umbilical incision; for example, for performing "hybrid" procedures that merges the principles of laparoscopic and open surgeries.
Conclusion
In our study, we have opened the curtain over an unexplored area of employing the SIPES technique and demonstrated the possibility of widely using it for correcting congenital anomalies of kidneys in an early age group of children.
We demonstrate that single incision vs. multiport nephrectomy on non-functioning kidneys in infants is equally effective. Supported by the results, we conclude that SIL-N can be safely changed conventional pediatric endosurgical procedures without adjusting current surgical protocols. Without any doubt, the most desirable cosmetic result is the biggest advantage of a single-incision nephrectomy that uses the umbilicus as a keyhole for full elimination of a postoperative scar from abdominal wall. Finally, the aesthetic judgment has not been described objectively and "improved cosmetic result" still remains a subjective impression of the surgeon who opposes total virtual absence of the visual scar after SIPES to three small marks on an abdominal wall after insertion of instrumental laparoports when using multi-port laparoscopy. Future comparative studies will determine the cosmesis of single-port laparoscopy for the treatment of kidney diseases in children, based on the known scar scales and subjective impressions of parents of these patients.
References
- Ehrlich RM, Gershman A, Fuchs G (1994) Laparoscopic renal surgery in children. J Urol 151: 735-739.
- Prema Menon, Abhilasha T Handu, Katragadda Lakshmi Narasimha Rao, et al. (2004) Laparoscopic nephrectomy in children for benign conditions: indications and outcome. J Indian Assoc Pediatr Surg 19: 22-27.
- Valla JS (2007) Retroperitoneoscopic surgery in children. Semin Pediatr Surg 16: 270-277.
- Johnson KC, Cha DY, DaJusta DG, et al. (2009) Pediatric single-port access nephrectomy for a multicystic dysplastic kidney. J Pediatr Urol 5: 402-404.
- Park YH, Kang MY, Jeong MS, et al. (2009) Laparoendoscopic single-site nephrectomy using a homemade single-port device for single-system ectopic ureter in a child: Initial case report. J Endourol 23: 833-835.
- Wong K, Chung P, Lan L, et al. (2010) The first report of a single-port laparoscopic nephrectomy in a child. Hong Kong Med 16: 153-154.
- Koh CJ, De Filippo RE, Chang AY, et al. (2010) Laparoendoscopic single-site nephrectomy in pediatric patients: initial clinical series of infants to adolescents. Urology 76: 1457-1461.
- Ham WS, Im YJ, Jung HJ, et al. (2011) Initial experience with laparoendoscopic single-site nephrectomy and nephroureterectomy in children. Urology 77: 1204-1208.
- Luithle T, Szavay P, Fuchs J (2013) Single-incision laparoscopic nephroureterectomy in children of all age groups. J Pediatr Surg 48: 1142-1146.
- Cabezali Barbancho D, Gomez Fraile A, Lopez Vazquez F, et al. (2011) Single-port nephrectomy in infants: initial experience. J Pediatr Urol 7: 396-398.
- Yamada Y, Naitoh Y, Kobayashi K, et al. (2016) Laparoendoscopic single-site surgery for pediatric urologic disease. J Endourol 30: 24-27.
- Patel N, Santomauro M, Marietti S, et al. (2016) Laparoendoscopic single site surgery in pediatric urology: does it require specialized tools? Int Braz J Urol 42: 277-283.
- Clayman RV, Kavoussi LR, Soper NJ, et al. (1991) Laparoscopic nephrectomy: initial case report. J Urol 146: 278-282.
- Rane A, Ahmed S, Kommu SS, et al. (2009) Single port scarless laparoscopic nephrectomies: the United Kingdom experience. BJU Int 104: 230-233.
- Ponsky TA, Krpata DM (2011) Single-port laparoscopy: considerations in children. J Minim Access Surg 7: 96-98.
- Saldana LJ, Targarona EM (2013) Single-Incision Pediatric Endosurgery: a Systematic Review. J Laparoendosc Adv Surg Tech A 23: 467-480.
- Krpata DM, Ponsky TA (2011) Instrumentation and equipment for single-site umbilical laparoscopic surgery. Semin Pediatr Surg 20: 190-195.
Corresponding Author
Yury Kozlov, MD, Department of Pediatric Surgery, Irkutsk State Medical University, 57 Sovetskaya Str, Irkutsk 664009, Russia, Tel: +73952291635, Fax: +73952291566.
Copyright
© 2017 Kozlov Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.